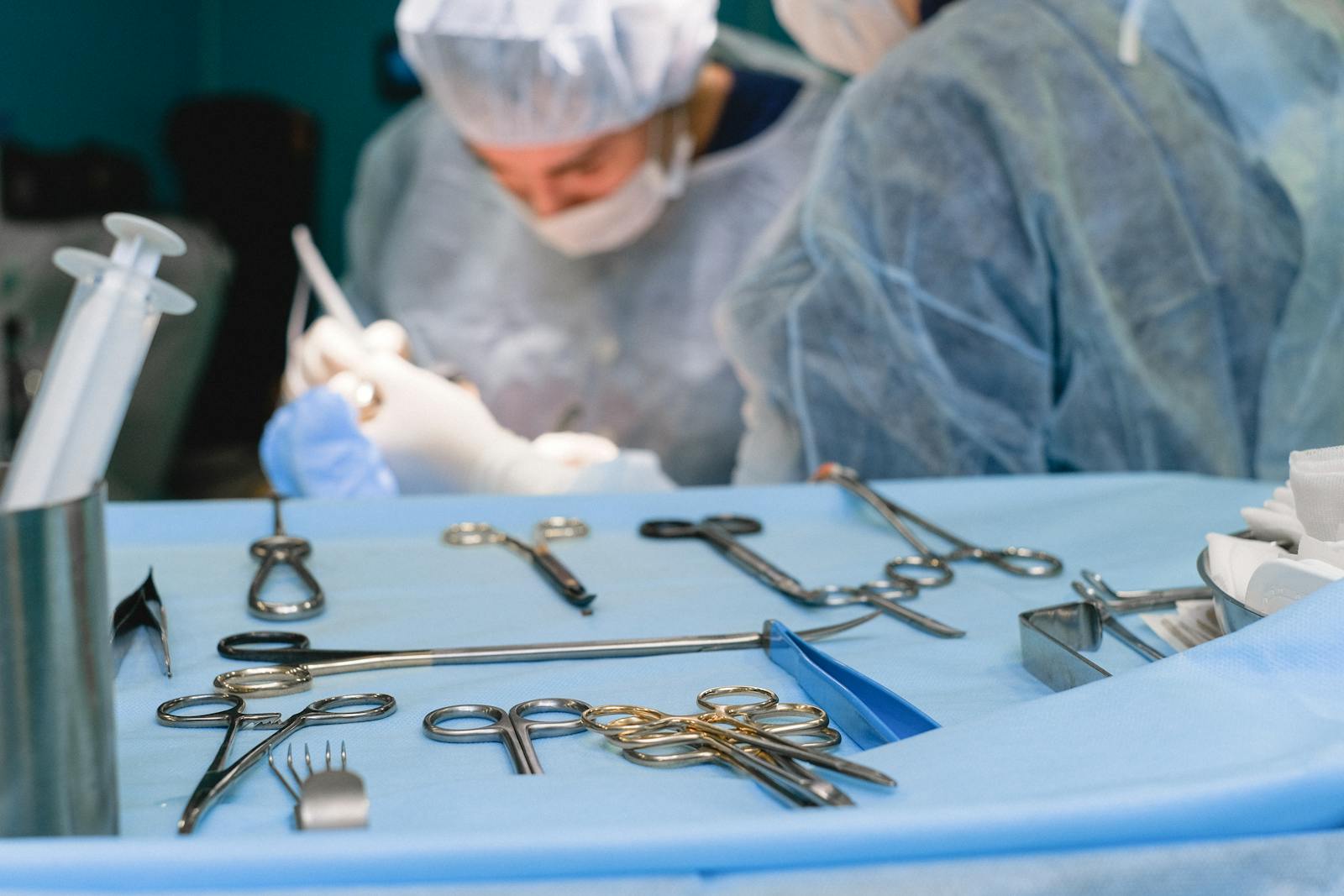
Coccygectomy, a surgical procedure to remove the coccyx or tailbone, is typically performed to alleviate persistent pain. While generally considered safe, a pertinent discussion must be held about a potential and significant post-operative complication: nerve damage. This subject merits our attention due to the close proximity of the coccyx to several pivotal neurological structures. The ensuing discourse will explore the causes, implications, and potential preventative measures for such surgical outcomes.
Understanding Coccygectomy Surgery
To fully comprehend the potential for nerve damage, it is crucial to first delve into the intricacies of coccygectomy surgery, a procedure involving the surgical removal of the coccyx, or tailbone, typically carried out to alleviate persistent and debilitating tailbone pain.
The procedure is often regarded as a last resort after conservative treatments, such as physical therapy and medications, have failed to provide sufficient pain relief. Nonetheless, like any surgical intervention, coccygectomy is not without its potential complications. Notably, nerve damage is a significant concern due to the coccyx’s proximity to vital nerve structures.
Accurate pain management is essential both before and after surgery to minimize the risk of coccygectomy complications. Achieving this goal requires a comprehensive understanding of the patient’s pain levels and the careful administration of analgesics, tailored to individual needs.
Despite these efforts, there’s the potential for complications such as wound infection, hematoma, rectal injury, and most notably, nerve damage. The latter, in particular, can lead to debilitating conditions like coccydynia, characterized by chronic inflammation and pain. Therefore, performing a coccygectomy demands a delicate balance between achieving pain relief and avoiding nerve damage.
Anatomy of the Coccyx
The coccyx, also known as the tailbone, has a unique structure and function within the human skeletal system, serving as an anchor point for multiple muscles and ligaments. Injuries to the coccyx, often caused by falls or direct impact, can lead to chronic pain and mobility issues, necessitating its surgical removal in some cases. However, the removal of the coccyx, or coccygectomy, has implications, including potential nerve damage, that require careful consideration.
Coccyx: Structure and Function
Situated at the base of the vertebral column, the coccyx, colloquially known as the tailbone, serves several critical functions, despite its small size and seemingly insignificant location. It is a vestigial structure, symbolizing the tail that our early primate ancestors once had, highlighting the coccyx evolution. Its significance can be understood by examining its multiple roles:
- It serves as an attachment point for various muscles, tendons, and ligaments, contributing to the stability of the pelvic region.
- It supports and stabilizes a person while sitting and leaning back.
- It plays a crucial role in weight distribution while sitting.
- It aids in the process of childbirth, providing flexibility and support.
These roles underscore the tailbone’s significance, making its potential damage a matter of serious concern.
Coccyx Injury: Causes
Given the vital functions of the coccyx, injuries to this area can cause significant disruption, with the causes of such injuries often rooted in the anatomy of the coccyx itself. It serves as a support structure during sitting and is subject to high pressure, making it vulnerable to injury. Falls, direct blows, childbirth, and repetitive strain from activities like cycling or rowing can lead to coccyx injury. Injury prevention strategies such as the use of protective padding, maintaining proper posture, and avoiding high-risk activities can reduce the likelihood of coccyx injury. Recovery techniques include physical therapy, pain management, and in severe cases, surgery. Despite prevention and recovery efforts, the unique anatomy of the coccyx can make it susceptible to injury and complicated healing processes.
Coccyx Removal: Implications
Often, the removal of the coccyx, or coccygectomy, presents substantial anatomical implications due to the coccyx’s crucial role in supporting and stabilizing the pelvic structure.
Key factors to consider include:
- The coccyx serves as a critical anchor point for numerous muscles, tendons, and ligaments. Its removal may destabilize these structures, potentially affecting mobility and balance.
- Coccygectomy may increase coccyx infection risks due to the invasive nature of the procedure and potential for post-operative complications.
- Psychosocial impacts of coccyx removal can be substantial, including changes in body image, sexual function, and overall quality of life.
- Neurological complications, such as nerve damage, are possible due to the close proximity of the coccyx to significant nerve bundles within the pelvis.
Each of these points warrants careful consideration during decision-making about coccygectomy.
Nervous System Overview
In order to fully comprehend the potential nerve damage from coccygectomy surgery, it is crucial to first understand the intricacies of the nervous system, a complex network that plays a pivotal role in the function and coordination of the body’s numerous physiological activities. The nervous system is primarily composed of the central and peripheral systems, which are responsible for controlling all bodily functions, interpreting sensory information, and enabling responses to changes in the environment.
Neurological disorders can occur when the nervous system’s function is compromised, leading to a wide range of symptoms, from mild discomfort to severe impairment. Particularly, the spinal cord function is essential in transporting nerve impulses between the brain and the rest of the body. Damage or diseases affecting the spinal cord can cause significant disruptions in this critical communication pathway.
Understanding the structure and function of the nervous system, particularly the spinal cord, offers insight into the possible complications following coccygectomy, including nerve damage. In-depth knowledge of the nervous system’s workings can help in predicting, identifying, and managing potential nerve damage and other neurological issues post-surgery. This comprehension forms the basis for further discussion on the specific mechanisms and manifestations of nerve damage, a topic to be elaborated on in the next section.
Nerve Damage Explained
Nerve damage, a potential consequence of coccygectomy surgery, warrants a thorough examination. A detailed analysis of the nature of nerves and their susceptibility to injury in the surgical process can highlight the risks associated with this procedure. By understanding the intricacies of nerve damage, we can better assess the potential outcomes and tailor surgical approaches to minimize this risk.
Understanding Nerve Damage
While it is vital to understand the risks associated with coccygectomy surgery, it is equally crucial to comprehend the concept of nerve damage, a potential side effect that can significantly impact a patient’s quality of life.
Nerve damage can occur due to several factors during a coccygectomy procedure. The nerves might be directly injured or traumatized during surgery, leading to neuropathic pain and potentially hindering nerve regeneration. This can result in persistent pain, numbness, or even functional impairment.
To gain a better understanding, consider these key points:
- Nerve damage can cause neuropathic pain, a chronic condition characterized by burning, stabbing, or shooting pain.
- Depending on the extent of the damage, the body’s capability for nerve regeneration might be affected.
- Nerve damage can lead to loss of sensation or function in the affected area.
- Diagnosis and management of nerve damage require a multidisciplinary approach for optimal patient outcomes.
Risks in Coccygectomy Surgery
Despite its potential benefits, coccygectomy surgery carries inherent risks, among which nerve damage stands as a significant concern that warrants careful examination and understanding. This risk is often due to surgical trauma to the sacral plexus or its branches. The likelihood of nerve damage is influenced by factors such as surgical technique, patient anatomy, and the underlying cause of coccydynia.
Considering these risks, surgery alternatives like non-operative management, including physical therapy and pain management, should be explored. Post-operative care is also critical in mitigating nerve damage risks. This involves careful monitoring of neurological signs, prompt management of post-operative pain, and rehabilitation. Healthcare providers must weigh the potential benefits against these risks before recommending coccygectomy.
Causes of Post-Surgery Nerve Damage
Post-surgery nerve damage, often resulting from coccygectomy procedures, can be attributed to a multitude of factors, including surgical technique, patient anatomy, and post-operative care. The complexity of the coccyx region, the presence of numerous nerves and the proximity to the spinal cord, can increase the risk of nerve damage during surgery.
Factors that contribute to nerve damage include:
- Surgical Technique: A less precise or invasive technique can inadvertently damage nerves.
- Patient Anatomy: Individual anatomical differences can increase the risk of nerve injury during surgery.
- Post-Operative Care: Inadequate post-operative care can lead to complications, including nerve damage.
- Nerve Regeneration: The natural process of nerve repair, nerve regeneration, can occasionally lead to complications, such as neuroma formation, which can result in persistent pain.
The damage prognosis can be influenced by the extent and nature of the injury, as well as the patient’s overall health and ability to recover. It is crucial to consider these factors when planning and conducting a coccygectomy to mitigate the risk of nerve damage and ensure optimal patient outcomes.
Identifying Nerve Damage Symptoms
Recognizing the symptoms of nerve damage following a coccygectomy is crucial for early intervention and optimal recovery, as these manifestations can often be subtle yet significantly impact patient’s quality of life. Symptoms typically vary based on the extent and location of the damage but commonly include numbness, pain, or weakness in the lower extremities.
Analytical data indicates that the progression of such damage can either be acute, developing immediately after surgery, or chronic, resulting from ongoing nerve irritation. It’s noteworthy that the speed and success of nerve regeneration significantly influence symptom manifestation and severity.
In some cases, patients may experience sensory changes, such as hypersensitivity or lack of sensation. These could be compounded by motor symptoms like muscle weakness or paralysis, indicative of severe nerve damage. Altered bowel and bladder function, another potential symptom, is particularly concerning as it points to damage of the autonomic nerves controlling these functions.
Diagnostic Methods for Nerve Damage
Unraveling the complexities of nerve damage following coccygectomy requires specialized diagnostic methods, which hinge on meticulous clinical evaluation and advanced technological tools. These methods help in determining the extent of nerve damage, its location, and the type of nerves affected.
Two of the most widely employed diagnostic tools for nerve damage are nerve conduction studies and electromyography tests. Nerve conduction studies measure the speed and strength of signals traveling between nerves, providing definitive information about the functionality of the nerve. Electromyography tests, on the other hand, record the electrical activity of muscles, which can be disrupted when the nerves supplying these muscles are damaged.
The following are additional diagnostic methods for nerve damage:
- Magnetic Resonance Imaging (MRI): Provides detailed images of the spinal cord and nerves.
- Computed Tomography (CT) Scan: Generates cross-sectional images of the spine for a comprehensive evaluation of the nerve structures.
- Myelography: Uses a special dye injected into the spinal canal to highlight the nerve pathways in X-ray images.
- Discogram: Assesses the intervertebral discs and helps in identifying if an abnormal disc is causing nerve damage.
These diagnostic methods provide a robust framework for understanding and addressing nerve damage after coccygectomy.
Treatment Options for Nerve Damage
For the management of nerve damage resulting from coccygectomy surgery, two primary treatment modalities are typically considered: medicinal management techniques and surgical intervention possibilities. Medicinal approaches often seek to control symptoms and support the body’s inherent healing mechanisms, using a range of pharmaceutical agents. In contrast, surgical interventions may be employed to directly address the physical causes of damage, such as by repairing injured nerves or removing pressure points.
Medicinal Management Techniques
Often, the management of nerve damage resulting from a coccygectomy involves the strategic use of specific medications, which have been clinically proven to alleviate symptoms and enhance patient recovery. This process, known as Pain Management, relies heavily on Medication Efficacy.
The most commonly used medications include:
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): These drugs are effective in reducing inflammation and pain.
- Antidepressants: Certain types are known to help manage chronic pain.
- Anticonvulsants: Originally designed to treat epilepsy, they have proven helpful in nerve pain management.
- Opioids: For severe pain, opioids can be used, but they carry a risk of addiction.
Each medication has its own potential benefits and risks, necessitating a personalized approach to treatment planning.
Surgical Intervention Possibilities
In addition to medication, there are several surgical options available to treat nerve damage resulting from a coccygectomy, each with varying degrees of invasiveness, efficacy, and associated risks. These surgery alternatives, such as neural reconstruction and neurolysis, strive to repair, regenerate, or free the affected nerves. Neural reconstruction involves the rerouting or grafting of nerves, while neurolysis involves the removal of scar tissue compressing the nerves. The choice of surgery is determined by the extent and location of the nerve damage, patient’s overall health, and the surgeon’s expertise. Regardless of the chosen intervention, a comprehensive rehabilitation process follows. This involves physical therapy, occupational therapy, and pain management strategies, all crucial for optimizing patient outcomes and enhancing recovery.

Coping Strategies for Nerve Damage
A considerable number of patients dealing with nerve damage post-coccygectomy surgery require effective coping strategies to manage their symptoms and enhance their quality of life. The psychological impact of the surgery and subsequent nerve damage can be significant, with patients often needing to adjust to a new reality.
Key strategies for coping with this situation include:
- Utilizing nerve regeneration techniques: These can accelerate healing and reduce pain. They often involve physical therapies or specific exercises designed to stimulate nerve growth.
- Psychological support: Counselling can help patients deal with the emotional toll of nerve damage. It can also provide techniques for managing pain and stress.
- Medication management: This involves the careful use of pain relief and nerve repair drugs under medical supervision.
- Lifestyle modifications: Changes to diet, exercise, and sleep habits can all aid in nerve recovery and pain management.
These strategies are not mutually exclusive and are typically most effective when used in tandem. They are evidence-based, with studies showing their efficacy in managing nerve damage symptoms post-coccygectomy surgery. The goal of these strategies is to provide patients with the tools necessary to lead a comfortable and fulfilling life, despite their nerve damage.
Prevention of Nerve Damage
Mitigating the risk of nerve damage associated with coccygectomy surgery demands careful preoperative planning and precise surgical techniques. Thorough preoperative evaluation can help in mapping the patient’s anatomy, identifying potential areas of risk, and planning the surgical approach accordingly.
Intraoperatively, strict adherence to surgical protocols and rigorous nerve monitoring can significantly reduce the likelihood of inadvertent nerve injury. Minimal invasive techniques can be employed to minimize tissue trauma and preserve nerve function. Furthermore, immediate postoperative neurological assessment and early intervention in case of nerve impairment can potentially arrest further damage and promote nerve regeneration.
Neurological rehabilitation is an integral part of prevention strategy for nerve damage. It emphasizes restoring function, preventing complications, and improving the patient’s quality of life. Rehabilitation plans should be tailored to the individual patient’s needs and can include physical, occupational, and speech therapy as well as pain management strategies.
Moreover, research has shown that certain neurotropic factors and drugs can enhance nerve regeneration and recovery. Hence, exploring the potential of pharmacological interventions in preventing nerve damage warrants further investigation. In conclusion, prevention of nerve damage in coccygectomy involves a multifaceted approach combining meticulous surgical technique, vigilant monitoring, and comprehensive rehabilitation.
Patient Stories: Living With Nerve Damage
Understanding the lived experiences of patients who have suffered nerve damage post-coccygectomy provides invaluable insight into the challenges, coping strategies, and adaptive mechanisms employed to manage their condition. These personal experiences reveal the emotional impact and perseverance required to navigate life after surgery.
- Patient A: A young professional who experienced sharp, shooting pain post-surgery. She adopted a combination of physical therapy and medication to manage her symptoms, demonstrating resilience in the face of adversity.
- Patient B: An older patient who reported loss of sensation and movement. He used assistive devices and altered his lifestyle to accommodate his condition, showing adaptability.
- Patient C: A middle-aged woman who experienced bouts of numbness and tingling. Her emotional journey involved acceptance, fear, and finally resolve to live a fulfilling life despite her condition.
- Patient D: A man who suffered from chronic pain and had to quit his physically demanding job, highlighting the significant impact on livelihoods.
These narratives show the breadth and depth of experiences, emphasizing the need for personalized, comprehensive care. They also underscore the importance of emotional support in managing the aftermath of nerve damage from coccygectomy.
Frequently Asked Questions
What Are the Potential Psychological Effects of Living With Nerve Damage After a Coccygectomy Surgery?
Potential psychological effects may include anxiety, depression, and altered body image. Nerve damage coping strategies and the psychological adjustment process play key roles in managing these challenges, promoting resilience, and improving overall mental health.
Can Nerve Damage From Coccygectomy Surgery Affect Sexual Function?
Yes, nerve damage from coccygectomy surgery can indeed impact sexual function. Nerve damage symptoms may include sexual dysfunction, necessitating sexual rehabilitation options to improve function and quality of life post-surgery.
Are There Support Groups or Resources Available for Individuals Dealing With Nerve Damage After Coccygectomy Surgery?
Yes, numerous resources exist for individuals dealing with post-surgical complications. Online platforms offer nerve damage coping strategies and post coccygectomy pain management advice, while support groups provide community and shared experiences.
How Might Nerve Damage From Coccygectomy Surgery Impact a Person’s Career or Ability to Work?
Nerve damage could necessitate significant career adjustments due to physical limitations or discomfort. In severe cases, it may lead to claiming disability benefits if the individual is unable to maintain their previous level of work.
Can Nerve Damage From Coccygectomy Surgery Be Reversed or Significantly Improved With Time or Further Treatment?
Nerve regeneration possibilities after surgery are variable, depending on the severity of damage. Advanced treatment options, including physical therapy and medication, can aid recovery but complete reversal of nerve damage is not always possible.