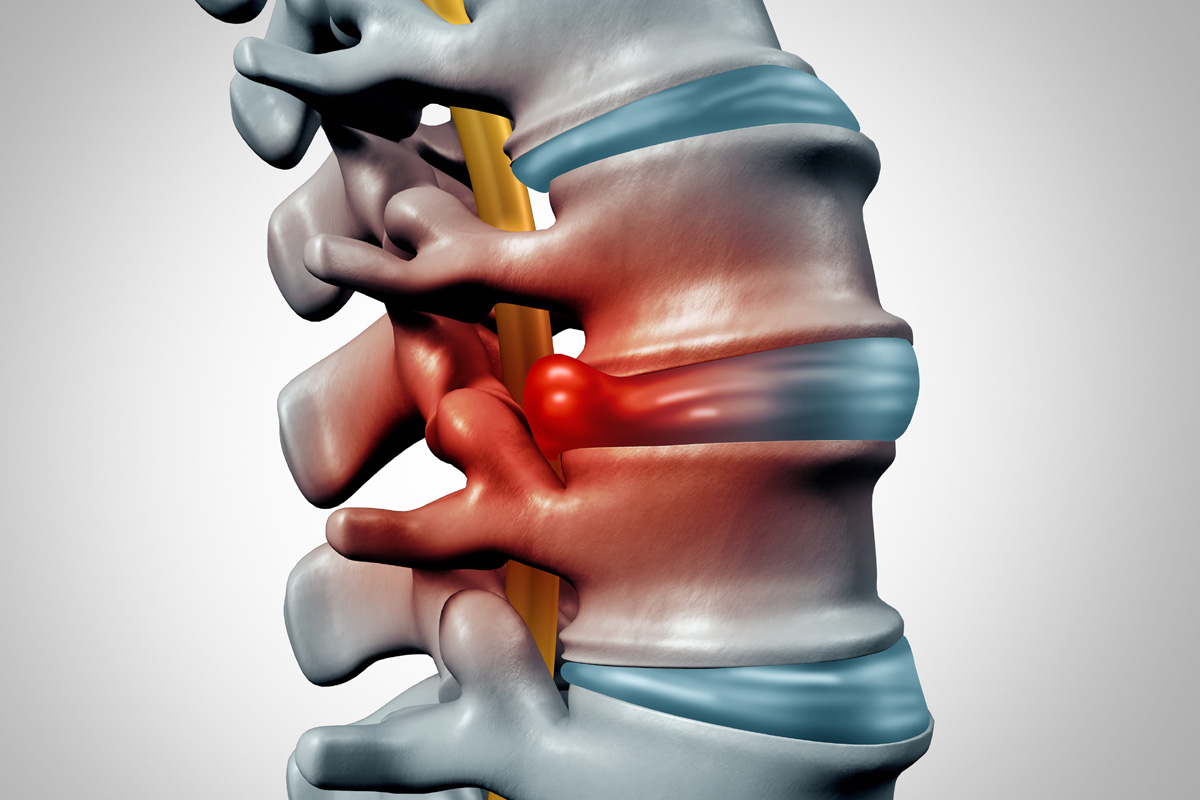
Herniated discs, a common yet often misunderstood condition, can cause significant discomfort and impair daily activities. Symptoms can range from mild to severe, often dependent on the location of the herniation and its degree. The causes of disc herniation are multifaceted, including age, lifestyle, and certain risk factors. As we discuss the complexities of herniated discs, consider this: Are you aware of the potential complications of untreated herniation? Moreover, can you differentiate a herniated disc from other spinal conditions? Let’s explore this further.
Understanding Herniated Discs
Delving into the complexities of a herniated disc, it’s crucial to comprehend that this condition involves an issue with one of the rubbery cushions, called discs, situated between the individual bones that stack up to make your spine. This typically occurs when some of the softer, jelly-like interior pushes out through a tear in the tougher exterior of the disc. This protrusion can irritate adjacent nerves, resulting in disc-related pain.
The intensity and location of the pain can vary greatly depending on the position of the herniated disc. For instance, if it occurs in the lower spine, it may cause intense pain in the buttocks, thigh, and calf. If the herniated disc is in the neck, the pain is usually most intense in the shoulder and arm. This pain may be accompanied by numbness or tingling in the body part served by the affected nerves.
Surgical interventions are considered if conservative treatments fail to alleviate symptoms or if neurological deficits, such as weakness or loss of bowel or bladder control, develop. The goal of surgery is to remove the herniated portion of the disc to relieve pressure on the nerve tissue and alleviate pain.
Anatomy of the Spine
To fully comprehend the nature and implications of herniated discs, a foundational knowledge of spinal anatomy is instrumental. This involves an overview of the spine’s structure, a detailed explanation of the spinal vertebrae, and an understanding of the discs within the spinal column. By exploring these key areas, we can better appreciate the impact a herniated disc can have on this complex system.
Spine Structure Overview
Understanding the anatomy of the spine, a complex structure comprised of vertebrae, discs, nerves, and muscles, is crucial to comprehending the intricacies of a herniated disc. The spine’s form, which includes the spinal curvature, is designed to bear weight, facilitate movement, and protect the spinal cord. Abnormalities in spinal curvature, such as those seen in scoliosis, can impact vertebral alignment, potentially leading to increased stress on the discs. This stress might escalate the risk of disc herniation. Moreover, the spine’s intricate network of nerves and muscles maintains balance and enables motion. Any disruption within this network can result in pain or dysfunction, which are often present in herniated disc conditions. Hence, understanding this structure is vital for comprehensive herniated disc knowledge.
Understanding Spinal Vertebrae
Building upon the general overview of the spine structure, the focus now shifts to a more detailed examination of the spinal vertebrae, a critical component of the spinal anatomy. These bony segments are the building blocks of your spine, providing structural support and protecting the spinal cord.
- Vertebrae Structure: Each vertebra has a robust body for weight-bearing and a circular arch to enclose the spinal cord.
- Vertebrae Classification: The spine contains 33 vertebrae classified into cervical, thoracic, lumbar, sacral, and coccyx regions.
- Spinal Health Maintenance: Regular exercise, proper posture, and a balanced diet contribute to the health of your vertebrae.
- Vertebrae Injury Prevention: Avoiding heavy lifting, using correct body mechanics, and doing regular spine strengthening exercises can prevent vertebrae injuries.
Discs in Spinal Column
Nested between each of your vertebral bodies are the intervertebral discs, a critical component of the spinal column that serves as shock absorbers, ensuring flexibility and movement of the spine. These discs are composed of a tough outer layer, the annulus fibrosus, and a gel-like center, the nucleus pulposus, which together contribute to disc flexibility. This combination allows the disc to compress and expand based on the body’s movements, maintaining spinal health. However, wear and tear or injury can cause the inner gel to herniate or protrude through the outer layer, leading to a herniated disc. This condition can cause pain, weakness, or numbness as it may press on nearby nerves. Understanding the structure and function of these discs is essential for prevention and treatment of such conditions.
Process of Disc Herniation
The human body’s intricate spinal structure may undergo a process called disc herniation, a condition where the intervertebral discs, which act as shock absorbers for the spine, experience undue pressure causing them to rupture or bulge. The disc location plays a crucial role in the severity and symptoms of the condition. Surgical interventions may be necessary depending on the extent of the herniation and the impact on the patient’s quality of life.
The process of disc herniation involves four key stages:
- Disc Degeneration: Normal aging and wear and tear contribute to a reduction in the disc’s water content, making it less flexible and more prone to tearing or rupturing with a minor strain or twist.
- Prolapse: The disc’s form distorts slightly, leading to a bulge that protrudes from its normal location in the spinal column.
- Extrusion: The gel-like nucleus pulposus breaks through the disc’s outer layer but remains within the disc.
- Sequestration: The nucleus pulposus breaks through the disc wall, moves outside the disc, and enters the spinal canal.
Understanding this process is vital in the management and treatment of herniated discs.
Common Causes of Disc Herniation
The common causes of disc herniation can be broadly classified into three categories: impact of physical activity, age-related disc degeneration, and occupational risk factors. Physical activities, especially those involving heavy lifting or sudden movements, often contribute to disc damage, leading to herniation. Age-related degeneration and certain occupational hazards further exacerbate the risk, creating a complex interplay of factors leading to this condition.
Physical Activity Impact
Physical strain resulting from vigorous activities often leads to disc herniation, a condition marked by extreme back pain and discomfort. Exercise precautions and posture correction are key preventive strategies. Physical activity impacts the spinal disc health in several ways:
- Heavy Physical Work: Frequent lifting, bending, and twisting can increase the pressure on your spine, leading to disc damage.
- Inactive Lifestyle: Lack of regular exercise can weaken the muscles that support your spine, increasing the risk of disc herniation.
- Poor Posture: Incorrect posture while sitting, standing, or working can put extra strain on your spine.
- Trauma or Injury: Accidents or sports injuries can cause severe damage to your discs, leading to herniation.
Understanding these impacts can help in preventing disc herniation and managing existing conditions effectively.
Age-Related Disc Degeneration
In addition to the impact of physical activities, age-related disc degeneration also plays a significant role in the occurrence of disc herniation. As individuals age, degenerative patterns begin to emerge, which slowly erodes disc resilience, thereby increasing susceptibility to herniation. These patterns involve changes such as loss of disc water content, leading to reduced flexibility and shock absorption. This condition is further exacerbated by the natural wear and tear of the disc’s outer layer, making it more prone to cracks and tears. Moreover, the reduced blood flow and nutrient supply to the discs with aging contributes to their degeneration. Thus, understanding these degenerative patterns and factors affecting disc resilience is crucial for preventive strategies against disc herniation.
Occupational Risk Factors
Could your job be contributing to your risk of developing a herniated disc? Occupational factors often play a significant role in the onset of this condition.
- Workplace ergonomics: Poorly designed workspaces can force you into unnatural postures, leading to spinal stress and possibly a herniated disc.
- Heavy lifting techniques: Incorrect methods of lifting heavy items can put enormous pressure on your lower back, increasing the risk of disc herniation.
- Sedentary jobs: Long hours of sitting, especially with poor posture, can impose excessive load on your lumbar discs.
- Physically demanding jobs: Occupations requiring repetitive bending, twisting, or lifting can cause wear and tear on the spinal discs.
Consider these factors and evaluate if your work environment or habits need changes.
Risk Factors for Herniated Discs
Certain lifestyle choices and genetic predispositions can significantly increase an individual’s risk of developing a herniated disc. Genetic predisposition plays a vital role as it is observed that individuals with a family history of spinal disc problems are more likely to develop a herniated disc. This indicates a genetic component in the susceptibility to disc degeneration and herniation.
The impact of obesity on the risk of herniated discs is also noteworthy. Excessive body weight places additional stress on the discs in the lower back, elevating the risk of disc herniation. The extra burden caused by obesity accelerates the natural wear and tear process of the discs, making them more prone to herniation.
Other risk factors include age, as disc herniation is more common in middle-aged and elderly individuals due to the natural degeneration of the discs over time. A sedentary lifestyle, characterized by prolonged periods of sitting and lack of physical activity, has also been linked with an increased risk of herniated discs due to the pressure it puts on the spinal column. It is crucial to understand these factors to mitigate the risk and protect spinal health.
Herniated Disc Symptoms Overview
Understanding the symptoms of a herniated disc is crucial for early detection and effective treatment. This section will provide an overview of the most common indicators of a herniated disc, which may include but are not limited to, pain, numbness, and weakness in affected areas. Along with this, we will also touch upon the potential causes that lead to the development of herniated discs.
Identifying Disc Herniation Symptoms
Recognizing the symptoms of disc herniation is a critical step towards effective diagnosis and treatment of this common spinal condition. Disc herniation prevention and understanding herniation recovery time are integral to managing this condition.
The following symptoms may indicate the presence of a herniated disc:
- Pain in the arm or leg: A herniated disc in the lower back may cause intense pain in the buttocks, thighs, or calves. If the herniation is in the neck, the pain is usually felt in the arm and shoulder.
- Numbness or tingling: Patients often experience these sensations in the body part served by the affected nerves.
- Weakness: Muscles served by the affected nerves tend to weaken, affecting your ability to lift or hold items.
- Loss of bladder or bowel control: Although rare, this is a serious symptom requiring immediate medical attention.
Causes of Herniated Disc
While it is essential to identify the symptoms of a herniated disc, it is equally important to comprehend the underlying causes that lead to such a condition. A herniated disc can be attributed to a variety of factors, including genetic predisposition and lifestyle choices. Certain people are genetically more likely to experience disc degeneration, which can eventually result in a herniated disc. The role of genetics, however, is not the sole determinant. Obesity implications, for instance, play a significant role in this context. Excessive body weight exerts additional pressure on the discs in your lower back, making them more susceptible to herniation. Therefore, maintaining a healthy body weight and understanding your genetic vulnerabilities can significantly reduce the risk of developing a herniated disc.
Physical Symptoms of Herniated Discs
The physical symptoms of a herniated disc can manifest in varied ways, often depending on the location and severity of the condition. A vital aspect to consider is the role of a Disc Diet in mitigating these symptoms. The consumption of nutrient-rich foods that support spinal health can alleviate inflammation and aid in recovery. Alongside this, the importance of posture cannot be overstated. Misalignment and undue strain on the spine can exacerbate the condition, causing intensified pain and discomfort.
The physical symptoms of a herniated disc typically include:
- Localized Pain: This is generally felt in the area of the herniated disc, often intensifying with movement.
- Muscle Weakness: The affected area may exhibit loss of strength, impacting daily activities.
- Numbness or Tingling: Patients often report a sensation of pins and needles in the area served by the affected nerves.
- Radiating Pain: This can extend to the extremities, such as down the leg (sciatica) in the case of a herniated lumbar disc.
Understanding these symptoms is essential for early diagnosis and intervention, thereby preventing further damage and facilitating effective treatment.
Neurological Symptoms of Herniated Discs
In addition to these physical manifestations, herniated discs can also induce a range of neurological symptoms, primarily associated with nerve compression and irritation. These symptoms may vary depending on the location of the herniation, but commonly include numbness, weakness or tingling in the extremities.
Arm or leg pain is a typical complaint, with neck-based herniation often leading to discomfort radiating down the arm, while lower back herniation may be felt in the buttocks, thigh and calf. This pain can often be aggravated by certain movements or positions. Furthermore, patients may experience reflex diminution or loss, which can affect balance and coordination.
In terms of Disc Herniation Prevention, it is crucial to maintain a strong and flexible core, practice good posture, and employ safe lifting techniques to reduce the risk of disc damage. Regular physical activity and maintaining a healthy weight can also contribute to spinal health. Lastly, Pain Management Techniques can be used to control the discomfort associated with these neurological symptoms. These techniques can range from over-the-counter or prescription medications, to physical therapy, or in some cases, surgical intervention. These strategies are critical in managing the neurological implications of a herniated disc.
Complications From Untreated Herniation
Should a herniated disc remain untreated, it can pave the way for severe complications, including profound nerve damage, chronic pain, and in rare cases, loss of bowel or bladder control. It is essential to understand the potential risks associated with untreated herniation to prevent unnecessary suffering and to maintain quality of life.
- Profound nerve damage: Continuous pressure on the nerves can lead to permanent nerve damage, which may manifest as numbness, weakness, or even paralysis in extreme cases.
- Chronic pain: Persistent untreated herniation can result in chronic back or neck pain, significantly affecting daily activities and quality of life.
- Surgical complications: When herniation becomes severe, surgery may become necessary. However, surgery carries its own risks, including infection, bleeding, and in some cases, failed back surgery syndrome.
- Psychological impacts: Chronic pain and the limitations it imposes can lead to psychological distress, including depression, anxiety, and sleep disturbances.
Differentiating Herniated Discs From Other Conditions
Distinguishing herniated discs from other spinal conditions requires a keen understanding of the specific symptoms and diagnostic procedures involved. It is important to appreciate that different spinal conditions may present similar symptoms, complicating the diagnosis. Disc misalignment detection is one method used to differentiate a herniated disc from other conditions such as spinal stenosis, sciatica, or degenerative disc disease.
Pain patterns, for instance, can provide significant clues. Patients with a herniated disc typically experience symptoms on one side of the body, whereas conditions like spinal stenosis may cause bilateral symptoms. The type of pain can also vary. For example, herniated disc pain may intensify with certain movements or positions, whereas pain from spinal stenosis may worsen with walking or standing.
Non surgical interventions can further help discern the root cause of the symptoms. Physical examination, patient history, and response to treatments such as physical therapy or medication can all play a role in the differential diagnosis process. Notably, while non surgical interventions can alleviate symptoms in many spinal conditions, their effectiveness in addressing the underlying cause varies, further assisting in the differentiation process.
Diagnosis of Herniated Discs
Accurate diagnosis of herniated discs begins with a comprehensive evaluation of the patient’s medical history, followed by a thorough physical examination. During this process, information about onset, intensity, and location of the pain, as well as any associated symptoms is gathered. This helps in eliminating alternative diagnoses and focusing on the root cause.
Next comes the relevance of discography, a diagnostic procedure that involves injecting a contrast dye into the disc to make it visible on X-ray or CT scans. This allows the healthcare provider to identify any disc abnormalities and confirm the diagnosis.
The diagnostic process typically involves:
- Neurological examination: This checks nerve function and muscle strength.
- Imaging tests: MRI or CT scans provide detailed images of the spinal structures.
- Discography: This confirms the presence of a herniated disc and helps determine the exact disc that is causing symptoms.
- Electrodiagnostic tests: These include electromyography (EMG) and nerve conduction studies (NCS) to evaluate nerve damage.
These steps, when done in sequence, ensure an accurate diagnosis of herniated discs, paving the way for effective treatment plans.
Treatment Options for Herniated Discs
Once the diagnosis of a herniated disc is confirmed, a variety of treatment options are available, each tailored to the patient’s specific condition and severity of symptoms.
Non-surgical treatments are usually the first course of action and may include physical therapy, pain medication, and lifestyle modifications such as weight loss and cessation of smoking.
Alternative therapies like acupuncture, chiropractic adjustments, and yoga can also be beneficial. They focus on whole-body health, potentially reducing pain and promoting healing. However, their effectiveness varies across individuals and should be pursued under the guidance of a trained professional.
If conservative treatments don’t alleviate symptoms, surgical interventions may be considered. Microdiscectomy, a minimally invasive procedure, removes the portion of the disc causing nerve compression. Another surgical option, a lumbar fusion, can provide stability if multiple discs are affected.
The choice of treatment depends on various factors including the patient’s overall health, the location and size of the herniation, and the severity of symptoms. It’s crucial that patients discuss these treatment options with their healthcare provider to make an informed decision.
Frequently Asked Questions
Can a Herniated Disc Heal on Its Own Without Medical Intervention?
Yes, a herniated disc can sometimes heal on its own through natural remedies like rest, physical therapy, and lifestyle changes. However, severe cases may require surgical options for complete healing and pain relief.
What Lifestyle Changes Can Help Prevent Herniated Discs?
Lifestyle changes to prevent herniated discs include dietary adjustments to maintain a healthy weight, thereby reducing strain on the spine. Posture correction, regular exercise, and avoiding heavy lifting can also significantly lower the risk.
Are Certain Types of Exercise More Harmful or Beneficial to Individuals With Herniated Discs?
Individuals with herniated discs should focus on disc friendly workouts, such as swimming or pilates, which offer low-impact strength training. Pain management techniques can be beneficial, while high-impact exercises may exacerbate the condition.
How Does the Severity of a Herniated Disc Impact the Recovery Process and Time Required for Healing?
The severity of a disc herniation significantly impacts the recovery process. Greater disc severity often results in longer healing times due to increased tissue damage. Therefore, understanding the severity is crucial for effective treatment planning.
Can a Person With a Herniated Disc Perform Regular Daily Activities or Will They Be Limited?
A person with a herniated disc may experience disc-related pain that could limit daily activities. The severity of limitations varies per individual. Surgical options might be considered if pain severely impedes normal function.