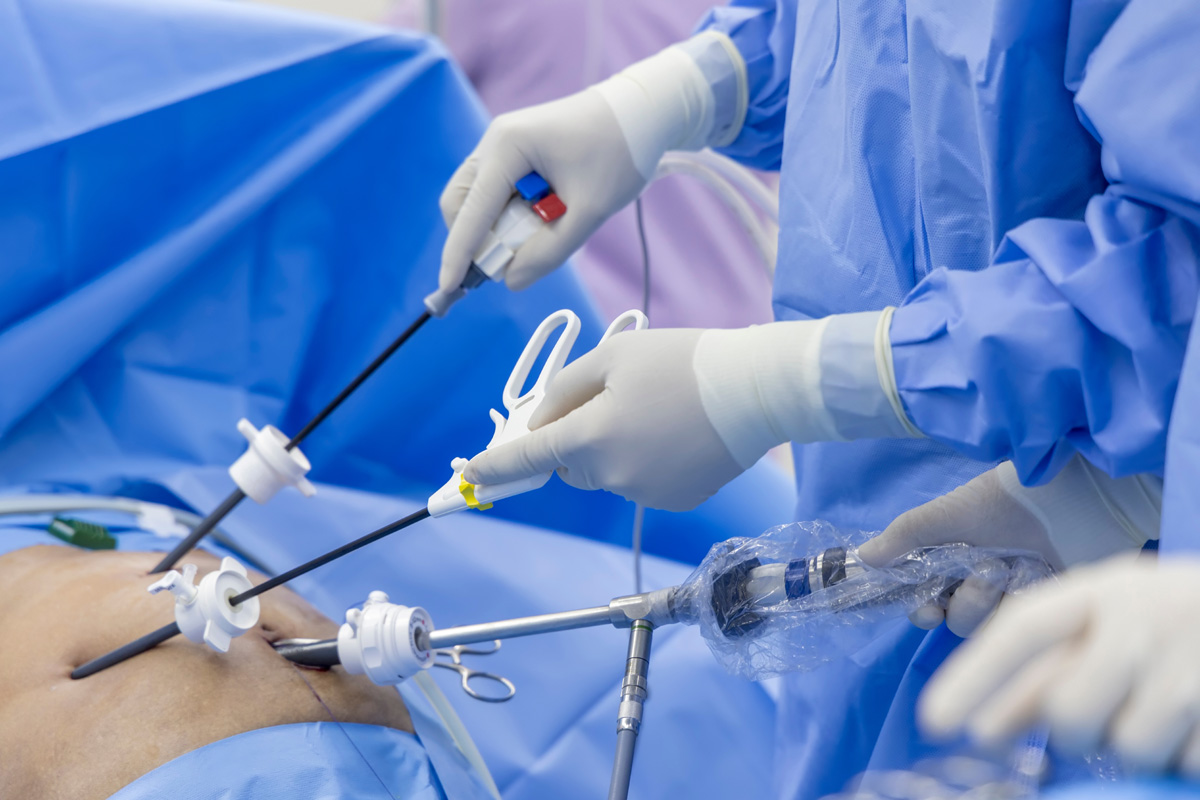
In the constantly advancing medical landscape, the emergence of minimally invasive surgery (MIS) has redefined traditional surgical paradigms, providing patients with less painful alternatives, shorter recovery times, and reduced hospital stays. However, like all medical innovations, MIS also presents its own unique set of challenges and limitations. As we explore the intricacies of this groundbreaking approach, we will also discuss the role of robotics in MIS, the preparation and recovery process, and the future prospects of this surgical technique.
Understanding Minimally Invasive Surgery
Minimally invasive surgery, a revolutionary approach in the medical field, refers to surgical procedures that minimize the size of incisions used, thereby reducing healing time, discomfort, and potential complications. This innovation has significantly transformed the patient experience and has implications for the overall cost of surgical procedures.
A surgery cost analysis of minimally invasive procedures reveals a potentially higher initial cost due to the advanced technology and specialized training required. However, these costs may be offset by shorter hospital stays and reduced post-operative complications, resulting in lower long-term costs.
From a patient experience perspective, insights indicate that patients undergoing minimally invasive surgery report less pain, minimal scarring, and faster recovery times compared to traditional surgical methods. The reduced physical trauma and quicker return to normal activities contribute to improved patient satisfaction rates.
However, it’s essential to note that the suitability of minimally invasive surgery depends on individual patient factors and the nature of the disease. Hence, the decision for this approach should be made carefully, considering both its potential benefits and limitations.
Traditional Surgery Vs. Minimally Invasive
In order to fully appreciate the advantages of minimally invasive procedures, it is imperative to contrast them with traditional surgical approaches, which often involve larger incisions and longer recovery periods.
- Surgery Costs: Traditional surgeries generally incur higher costs. These can include the surgeon’s fees, operating room costs, anesthesia, and post-operative care. In contrast, minimally invasive procedures often require less time in the operating room and shorter hospital stays, leading to overall lower costs.
- Patient Experiences: Traditional surgeries typically involve larger incisions, resulting in more post-operative pain and longer recovery periods. This can significantly impact a patient’s quality of life in the weeks following surgery. Minimally invasive procedures, on the other hand, cause less physical trauma and can often be performed on an outpatient basis, leading to a more comfortable post-operative experience for the patient.
- Risk Factors: Traditional surgeries carry a higher risk of complications such as infection and blood loss. Minimally invasive surgeries, due to their nature, reduce these risks and provide a safer alternative to traditional methods.
Types of Minimally Invasive Procedures
Minimally invasive procedures encompass a broad spectrum of surgical techniques that aim to reduce patient trauma and recovery time. These procedures, while varied, share the common goal of being less invasive than traditional surgeries, thus offering several potential benefits to patients. However, like all surgical interventions, they also carry certain risks and necessitate a specific recovery period, which will be explored further.
Common Minimally Invasive Procedures
While there is a broad spectrum of surgeries that can be performed in a minimally invasive manner, certain procedures have gained particular prominence due to their efficacy and reduced recovery times. These procedures, honed through rigorous surgical training, include:
- Laparoscopy: A technique employed primarily in the abdomen or pelvis, it involves small incisions and the use of a camera for guidance.
- Endoscopy: Used to examine the interior of a hollow organ or cavity, it’s crucial for diagnostics and surgeries in the gastrointestinal tract.
- Robotic Surgery: An advanced form of minimally invasive surgery, where precision and control are paramount.
Patient education plays a vital role in the adoption and success of these procedures. Understanding the surgery aids in better preparation, enabling a smoother recovery.
Benefits of Less Invasive Surgeries
Undoubtedly, less invasive surgical procedures, such as laparoscopy, endoscopy, and robotic surgery, offer numerous benefits, ranging from shorter hospital stays to reduced postoperative discomfort. In terms of surgery affordability, these procedures often result in lower overall healthcare costs due to the reduction in hospital stay length and less need for follow-up treatments.
Patient psychology also plays a significant role in the benefits of minimally invasive surgeries. Studies have shown that patients tend to have less anxiety and faster mental recovery following these procedures, largely due to the minimal scarring and quicker physical recovery. Moreover, the predictability and precision of these techniques afford patients a greater sense of control and understanding, further enhancing their psychological well-being. Thus, the benefits of less invasive surgeries extend beyond the physical, offering significant financial and psychological advantages.
Risks and Recovery Time
Despite the clear benefits of less invasive surgeries, it is crucial to consider the associated risks and recovery time inherent in these procedures.
- Risks: Like any surgical procedure, minimally invasive surgeries carry potential risks such as infection, bleeding, and complications from anesthesia.
- Recovery Time: Typically shorter than traditional surgeries, the recovery period can still vary greatly depending on the individual’s overall health and the complexity of the surgery.
- Cost implications and Insurance coverage: Minimally invasive surgeries may have higher upfront costs due to the use of specialized equipment but could potentially result in lower overall costs due to shorter hospital stays and less need for postoperative care. However, insurance coverage can greatly influence these cost implications, and it’s important for patients to understand their coverage before proceeding.
Tools and Technologies Used
In the realm of minimally invasive surgery, a diverse range of advanced tools and technologies are utilized to increase precision, reduce patient recovery time, and minimize potential complications. This area has seen a significant surgical training evolution, with the introduction of highly sophisticated tools such as laparoscopes, endoscopes, and other specialized instruments. These tools are designed to perform complex procedures through small incisions, thus minimizing tissue trauma and leading to quicker patient recovery.
The technology used in minimally invasive surgery is continually evolving, driven by medical advancements and the demand for safer, more efficient surgical procedures. Innovative imaging systems, for example, provide surgeons with a detailed, real-time view of the operative field, enhancing their ability to perform precise, targeted operations.
Patient awareness campaigns have played a crucial role in promoting these technologies, highlighting the benefits of minimally invasive alternatives over traditional open surgeries. These campaigns have helped to increase the acceptance and uptake of these procedures among patients, contributing to their growing prevalence in modern healthcare systems.
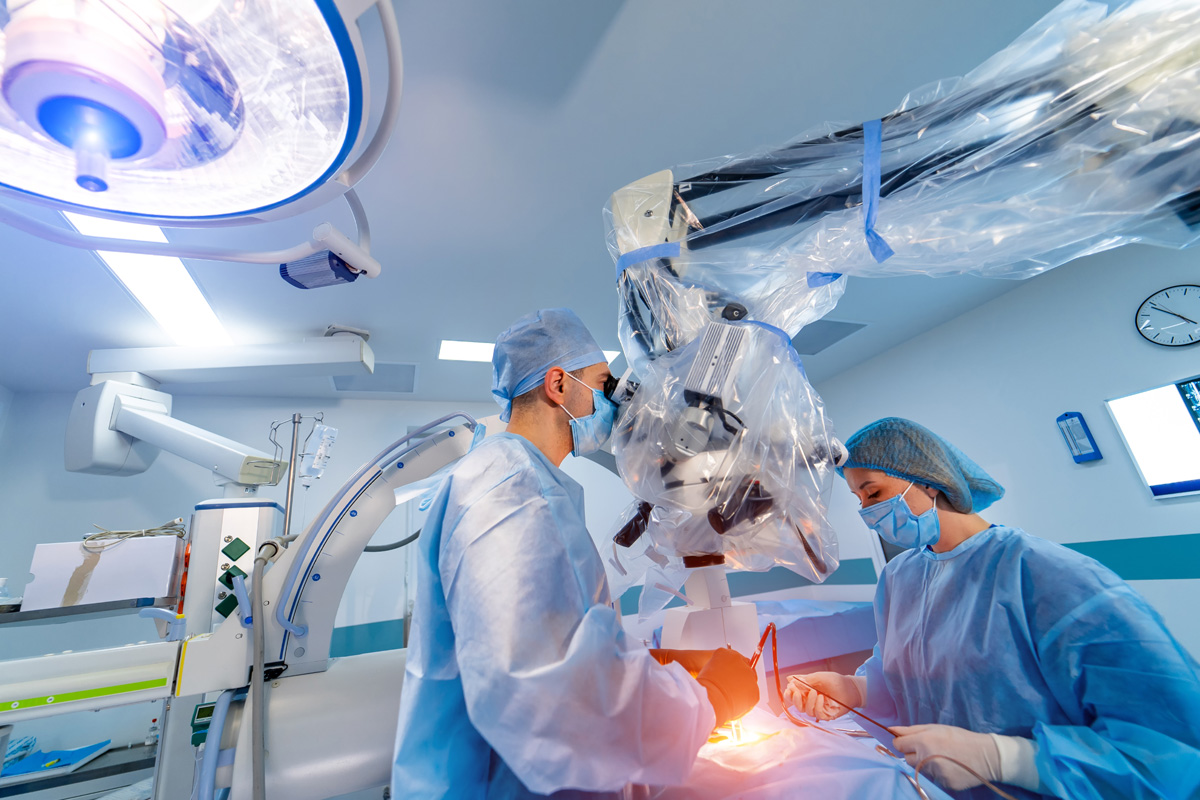
The Role of Robotics in Surgery
The integration of robotics into surgery has marked a significant stride in the field of minimally invasive procedures. As we explore this subtopic, we will focus on the recent advancements in robotic surgery and the consequential impact on surgical outcomes. This discussion will provide a better understanding of how robotics enhances precision, flexibility, and control during operations, thereby improving patient safety and recovery time.
Advancements in Robotic Surgery
Harnessing the power of technological innovation, advancements in robotic surgery have greatly revolutionized the field of minimally invasive procedures, enabling unprecedented precision and control. Three notable advancements include:
- Robotic surgery training: With the advent of virtual reality training, surgeons can now rehearse complex procedures, improving their skills without any patient risk.
- Improved robotic capabilities: Enhanced dexterity and stability of robotic arms provide surgeons with superior control, reducing the risk of human error.
- Cost effectiveness analysis: Despite high upfront costs, robotic surgery can result in fewer complications and shorter hospital stays, potentially offsetting initial expenditures.
These advancements, while still evolving, have significantly transformed the surgical landscape, promising a future where robotic surgery becomes the norm rather than the exception.
Impact on Surgical Outcomes
Undeniably, the incorporation of robotics into surgical procedures has had a profound effect on patient outcomes, enhancing precision, minimizing invasiveness, and potentially improving recovery times. Nonetheless, the benefits have come with their share of challenges. Surgical training implications have surfaced as a critical area of focus. Educating surgeons on the use of these advanced technologies requires a significant investment in time and resources. Furthermore, cultural acceptance barriers present a hurdle. Although robotics offer superior accuracy, the reliance on technology can raise concerns among patients and medical professionals alike, who may be wary of a machine’s role in sensitive procedures. Thus, while robotics have revolutionized surgery, navigating these issues is crucial to maximizing their impact on surgical outcomes.
Benefits of Minimally Invasive Surgery
Often hailed as a significant advancement in medical procedures, minimally invasive surgery presents numerous benefits, ranging from shorter recovery times to reduced post-operative discomfort. These surgeries are often performed through small incisions, using specialized instruments that cause less tissue damage, resulting in faster healing and recovery.
- Reduced Hospitalization Time: Minimally invasive surgeries typically have shorter hospital stays compared to traditional surgeries, leading to lower hospitalization costs. This is a crucial aspect considering the cost implications and the burden it can potentially reduce on the healthcare system.
- Less Post-Operative Pain and Faster Recovery: These procedures generally involve less pain and scarring post-operation. The reduced recovery time allows patients to return to their normal routines more swiftly, improving their quality of life significantly.
- Increased Accessibility: With the advent of technology and insurance coverage for such procedures, minimally invasive surgeries have become more accessible. This not only allows more patients to avail of these procedures but also reduces the financial strain on patients.
Risks and Complications
Despite the myriad benefits, minimally invasive surgeries can also pose certain risks and potential complications which need to be thoroughly evaluated and understood by patients and healthcare providers alike. These range from physical to emotional impacts, and even to surgery cost factors.
Among the physical risks, infection, bleeding, and complications from anesthesia are common. These can lead to extended hospital stays, readmission, or additional procedures, exponentially increasing the overall surgery cost factors. Additionally, while minimally invasive surgeries typically offer shorter recovery times, patients may still experience post-operative pain or discomfort.
The emotional impacts of these surgeries should also not be underestimated. The potential for complications can cause significant anxiety and stress. Even when procedures go as planned, patients may still suffer from post-surgical depression due to the disruption to their daily lives or fear of recurrence.
Economic burdens can also contribute to the emotional stress. High medical bills, potential loss of income during recovery, and the cost of follow-up care can all be financially daunting. Therefore, it is crucial for patients to have a clear understanding of the complete cost implications prior to the procedure.
Ideal Candidates for Minimally Invasive Surgery
Identifying the ideal candidates for minimally invasive surgery requires a comprehensive assessment of the patient’s health status, alongside careful analysis of the types of conditions that can be effectively treated. It is essential to evaluate both the benefits and potential risks involved in the procedure for each individual. This ensures optimal outcomes and minimizes complications associated with this surgical approach.
Assessing Patient’s Health Status
Evaluating a patient’s health status is a crucial step in determining their eligibility for minimally invasive surgery, a process that necessitates meticulous analysis of their overall physical condition, existing medical complications, and tolerance to anesthesia. Health assessment techniques are employed, which include:
- Comprehensive medical history review: This is paramount to identify any potential contraindications that may cause complications during or after the surgery.
- Physical examination: This involves a thorough inspection to evaluate the patient’s physiological status.
- Psychological assessment: This is to ascertain a patient’s psychological readiness, which is an integral part of the preoperative assessment.
Every potential candidate for minimally invasive surgery must undergo these assessments to ensure the highest probability of successful surgical outcomes.
Types of Eligible Conditions
Having established the importance of a comprehensive health assessment, we can now proceed to examine the specific conditions that generally make a patient an ideal candidate for minimally invasive surgery. The primary considerations include the nature and severity of the medical issue, the patient’s overall health, and the potential benefits of a less invasive procedure. For instance, conditions such as gallstones, hernias, and certain types of cancer can often be treated effectively through minimally invasive methods. However, the cost comparison between traditional and minimally invasive procedures also plays a critical role, as does insurance coverage. Patients with comprehensive medical insurance are more likely to be approved for these procedures, provided the benefits outweigh potential risks and costs.
Benefits and Risks Involved
In the realm of medical procedures, minimally invasive surgery often stands out due to its numerous advantages. However, it is essential to weigh these benefits against potential risks before determining the suitability of a patient for this type of intervention.
- Surgery alternatives: While traditional open surgery may be necessary in certain cases, minimally invasive techniques often offer a viable alternative, potentially reducing recovery times, post-operative pain and risk of complications.
- Cost comparison: Minimally invasive procedures can be more cost-effective in the long run, considering lower hospitalization costs and quicker return to work for patients.
- Risks: Despite the benefits, these procedures are not without risk. Possible complications include infection and issues related to anesthesia. Therefore, the patient’s overall health status, the specific condition and the surgeon’s expertise should all be taken into account when considering minimally invasive surgery.

Preparing for a Minimally Invasive Procedure
Understanding how to adequately prepare for a minimally invasive procedure is crucial to ensure a smooth surgical process and recovery. Surgery anxiety is common among patients, and it often arises from a lack of knowledge about the procedure. Therefore, patient education plays a key role in the preparation phase.
Educational sessions aim to provide patients with a comprehensive understanding of the procedure, including the techniques used, potential risks, and expected outcomes. By doing so, it helps to alleviate surgery anxiety and promotes a sense of control and confidence in patients. It is important for patients to ask questions and clarify any doubts during these sessions.
Additionally, patients are advised to follow preoperative instructions, which typically include dietary restrictions, medication guidelines, and hygiene practices. Fulfilling these instructions is essential for minimizing surgical complications and promoting optimal healing post-surgery.
In some cases, psychological support may be beneficial for patients with intense surgery anxiety. Techniques such as cognitive-behavioral therapy, relaxation methods, and guided imagery can be utilized to manage anxiety effectively.
What to Expect During Recovery
Postoperative recovery following a minimally invasive procedure often encompasses several stages, each characterized by distinct milestones and potential challenges. This period may vary in duration and intensity, depending on the patient’s overall health, the specific procedure performed, and the individual’s response to surgery.
- Post surgery diet: The first few days following surgery are crucial for a patient’s recovery and diet plays a significant role. A diet rich in protein, vitamins, and minerals, along with adequate hydration, is commonly suggested to promote healing and boost recovery. It’s also important for the patient to gradually reintroduce certain foods and monitor their body’s response.
- Pain management: Most patients experience some degree of discomfort after surgery. Hence, the use of pain management strategies is necessary. This might include medication, physical therapy, or alternative practices like meditation and deep breathing exercises.
- Physical activity and rest: Balancing rest with gentle physical activity helps in preventing complications like blood clots and pneumonia. However, it’s important not to rush recovery and allow the body adequate time to heal.
Success Stories and Case Studies
While the process of recovery is a critical aspect of minimally invasive surgery, it is equally enlightening to examine the success stories and case studies that demonstrate the efficacy and advantages of these surgical procedures.
Patient testimonials often highlight the significantly reduced recovery time, less post-operative pain, and minimal scarring as major advantages of minimally invasive procedures. For instance, a case study of a patient undergoing minimally invasive cardiac surgery reported returning to normal activities within two weeks, compared to traditional surgery that could require months of recovery.
Financial factors also play a significant role in the success of these procedures. The costs associated with shorter hospital stay, fewer complications, and quicker return to work further enhance the surgery affordability, making it a viable option for a larger portion of the population.
Moreover, the success of minimally invasive surgery is not limited to specific surgical procedures. Case studies across various medical fields such as orthopedics, gynecology, and gastroenterology, consistently report high success rates and patient satisfaction. These success stories evidently reflect the effectiveness of minimally invasive surgery, underlining its potential to revolutionize medical surgery procedures.
Future of Minimally Invasive Surgery
Looking ahead, the future of minimally invasive surgery promises to usher in new advancements and innovations that could further transform the landscape of surgical procedures.
- Surgical Training Evolution: With the advent of virtual reality and artificial intelligence, the training of surgeons for minimally invasive procedures is expected to undergo significant improvements. Advanced surgical simulators will provide trainees with realistic, hands-on experience, enhancing their skills before they step into the operating room.
- Improved Techniques and Technologies: The development of even more refined surgical tools and sophisticated imaging techniques will enhance precision and control during procedures. This, in turn, will minimize the risks associated with traditional surgery and improve patient outcomes.
- Addressing Global Accessibility Issues: The future of minimally invasive surgery also lies in its potential to be accessible to patients worldwide, irrespective of their geographical location. Telemedicine and robotic surgeries can play a pivotal role in closing the healthcare gap in remote and under-resourced regions.
In essence, the future holds immense potential for minimally invasive surgery. It will continue to evolve, driven by technological advancements, innovative training methods, and a commitment to making quality healthcare accessible to all.
Frequently Asked Questions
How Does Minimally Invasive Surgery Impact Health Insurance Coverage and Costs?
Insurance negotiations can be influenced by the type of surgery. Costs may be reduced due to shorter hospital stays and fewer complications, but out-of-pocket expenses may increase depending on the insurance policy’s coverage details.
What Kind of Training and Qualifications Does a Surgeon Need to Perform Minimally Invasive Surgery?
To perform surgical innovations, a surgeon requires specialized training in the specific procedures and techniques, along with board certification. These qualifications ensure enhanced patient recovery and lower risk of complications.
Are There Any Lifestyle Changes or Dietary Restrictions Required Before Undergoing a Minimally Invasive Procedure?
Before undertaking any medical procedure, certain lifestyle modifications like cessation of smoking and dietary restrictions may be required to reduce recovery time and minimize the risk of post-procedure complications. Specifics depend on individual health status.
How Frequently Is Minimally Invasive Surgery Used in Comparison to Traditional Surgery Worldwide?
The frequency of usage between the two surgical methods varies globally, influenced by factors like surgical risks comparison and the impact of technological advancements. Detailed statistics require comprehensive research and may differ based on specific medical specialties.
Are There Any Psychological Effects or Mental Health Considerations Associated With Undergoing Minimally Invasive Surgery?
Yes, psychological effects or mental health considerations can occur with any surgical procedures. Anxiety management and emotional preparedness can play key roles in addressing potential mental health issues related to the anticipation of surgery.