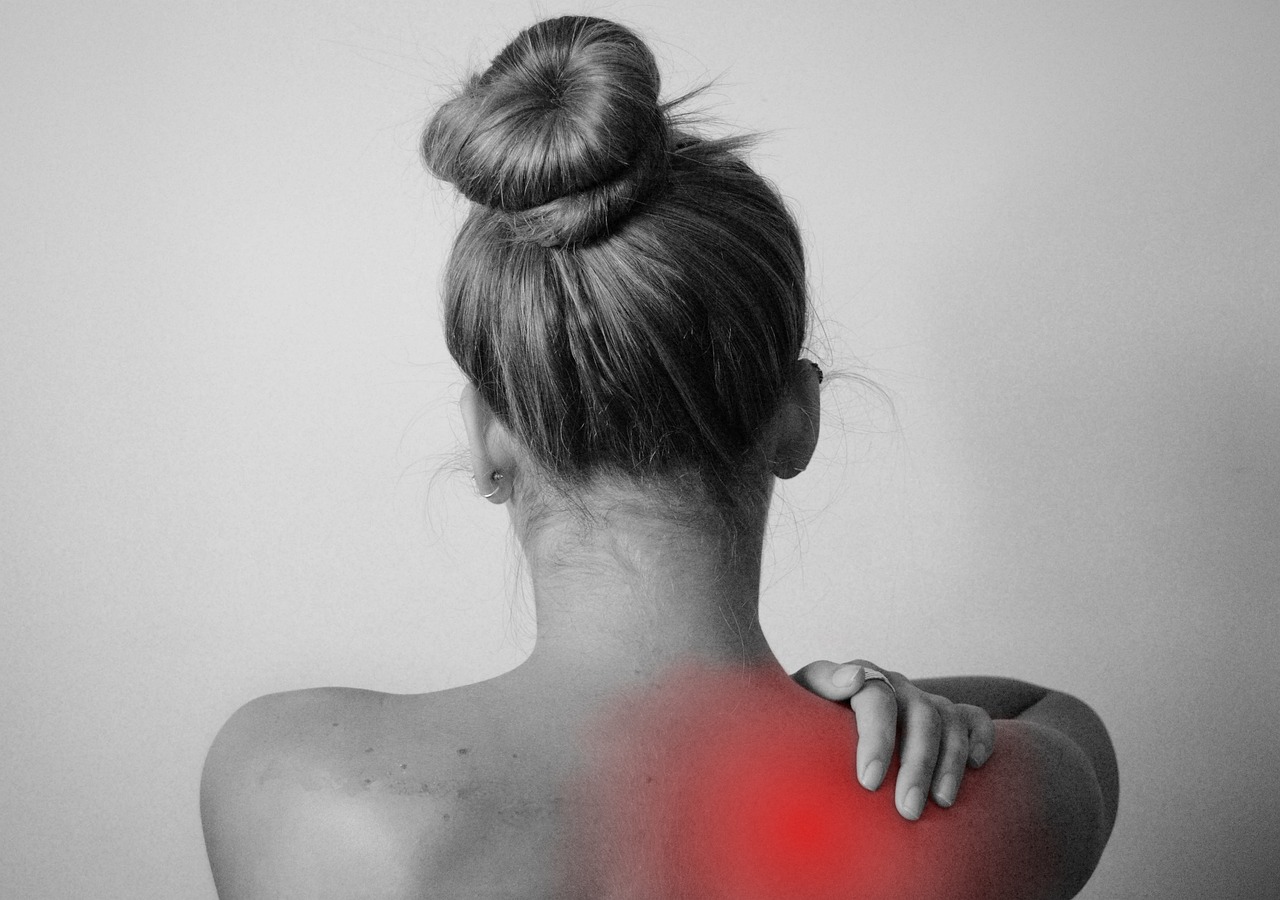
In the field of neurosurgery, one common procedure involves addressing cervical radiculopathy, or more commonly known as a pinched nerve in the neck. When non-invasive treatments fail to alleviate the discomfort and potential debilitation of a pinched nerve, surgical intervention may become essential. Methods such as discectomy, laminectomy, and cervical fusion are often employed, each with its own merits and considerations. This prompts the question: how are these surgeries performed and what factors contribute to their success? Let us explore the surgical landscape for treating pinched nerves in the neck.
Understanding Pinched Nerves
The intricate labyrinth of the human nervous system occasionally encounters an impediment, known as a pinched nerve, characterized by undue pressure on a nerve by surrounding tissues such as bones, cartilage, muscles, or tendons. This neurological dilemma manifests through symptoms such as numbness, tingling, or pain radiating along the nerve pathway.
Nerve compression prevention is vital in averting the debilitating effects of this condition. It involves a strategy of maintaining body alignment through correct posture during sitting, standing, and sleeping. Regular physical activity aids in muscle flexibility and strength, reducing the chances of nerve impingement. Ergonomic adaptations in daily activities and workspaces can also mitigate the risk of nerve compression.
In addition to these preventive measures, holistic healing methods can play a significant role in managing pinched nerves. Techniques such as yoga and acupuncture can help alleviate pressure on the nerve, while massage therapy can promote blood flow and relax tense muscles contributing to nerve compression. Dietary changes, particularly anti-inflammatory diets, can support overall nerve health. Understanding the nature of pinched nerves and implementing preventative and holistic healing strategies can greatly improve nerve health and alleviate discomfort associated with this condition.
Causes of Pinched Nerves in Neck
Understanding the causes of pinched nerves in the neck is critical for implementing effective treatment strategies. The etiology often involves a combination of common neck nerve irritants and certain lifestyle factors. In this section, we will analyse these causes, their mechanisms of action, and their impact on the occurrence of neck nerve impingement.
Common Neck Nerve Irritants
Numerous elements, ranging from degenerative diseases to traumatic injuries, can serve as irritants to the neck nerves, leading to the highly uncomfortable and disabling condition known as a pinched nerve. Vital in managing this condition is nerve irritant identification, a process which entails thorough exploration of the patient’s medical history, physical examination, and possibly diagnostic imaging. This facilitates the identification of the exact irritant causing the nerve compression.
Next comes irritant avoidance strategies, which may involve modification of activities, physical therapy, or in severe cases, surgical intervention. Degenerative diseases such as osteoarthritis or disc herniation, repetitive motion injuries, and even poor posture can all contribute to nerve irritation. Hence, understanding these irritants and implementing avoidance strategies can greatly mitigate the consequences of a pinched nerve in the neck.
Lifestyle Factors and Pinching
In analyzing causes of pinched nerves in the neck, lifestyle factors play a significant role, with certain habits and practices potentially leading to nerve irritation and compression. Three key lifestyle factors include:
- Posture: Poor posture, particularly during prolonged sitting, can place excess pressure on the neck. Healthy posture tips such as maintaining a neutral spine and avoiding forward head posture can alleviate this.
- Stress: Chronic stress leads to muscle tension and stiffness, exacerbating nerve compression. Stress management techniques like mindfulness and deep breathing can help reduce muscle tension.
- Physical Activity: Sedentary behavior can weaken neck muscles, increasing the risk of nerve pinching. Regular exercise, especially strength training, can help maintain muscle health and prevent nerve compression.
These lifestyle factors highlight the significant role of prevention in managing pinched nerves in the neck.
Symptoms Indicating a Pinched Nerve
When a nerve in the neck becomes compressed or irritated, it can cause a range of symptoms that may vary in severity and duration. Nerve compression triggers can be multifaceted, often stemming from degenerative disc disease, herniated discs, bone spurs, or even rigorous physical activities.
Patients may experience a spectrum of discomfort, from mild twinges to debilitating pain. One of the most common symptoms is a sharp or burning pain that radiates down the arm. This can be accompanied by numbness or a tingling sensation, often described as pins and needles. Additionally, some patients may face difficulties in certain neck movements, or experience muscle weakness affecting arm or hand dexterity.
It’s important to understand that pinched nerve remedies are largely dependent on the severity and persistence of these symptoms. Mild cases can be managed with non-surgical treatments such as physical therapy, medication, or lifestyle adjustments. However, persistent and severe symptoms may indicate the need for surgical intervention to alleviate nerve compression.
Diagnosing a Pinched Nerve
Establishing an accurate diagnosis for a pinched nerve involves a thorough clinical evaluation that may incorporate a detailed patient history, physical examination, and advanced imaging techniques.
The process of diagnosing a pinched nerve is multi-faceted and includes:
- Patient History: This involves a detailed conversation where the patient describes their symptoms, lifestyle, and any potential incidents that may have led to the onset of symptoms. This can provide important clues about the possible location and cause of the nerve compression.
- Physical Examination: The clinician may perform a variety of tests to assess nerve function and identify the affected area. This includes checking for areas of tenderness, evaluating range of motion, and examining muscle strength and reflexes.
- Advanced Imaging and Nerve Conduction Studies: These are essential for confirming the diagnosis and identifying the exact location of the nerve compression. MRI significance lies in its ability to produce detailed images of the body’s soft tissues, including nerves and spinal discs. This can reveal any abnormalities that may be causing nerve compression. Nerve conduction studies, on the other hand, measure the speed and strength of signals traveling along the nerves, helping to pinpoint any disruptions caused by the compression.
Traditional Treatment Methods
How do medical professionals address a diagnosed pinched nerve in the neck using traditional treatment methods? Primarily, traditional treatment methods focus on pain management and restoration of normal functionality. This involves a combination of medications, physical therapy, and lifestyle modifications.
Pain management is the first line of treatment. Non-steroidal anti-inflammatory drugs (NSAIDs) or corticosteroids are commonly prescribed to reduce inflammation and alleviate pain. Muscle relaxants may also be used to lessen muscle spasms often associated with a pinched nerve.
Physical therapy plays a pivotal role in the traditional treatment of a pinched nerve. Therapists guide patients through a series of exercises to strengthen neck muscles, improve posture, and increase flexibility, thereby relieving pressure on the nerve.
Lifestyle modifications are suggested to minimize further nerve compression. These include maintaining a healthy weight, adopting proper posture, and avoiding activities that strain the neck.
In addition to these, alternative therapies are considered. Acupuncture, massage, and chiropractic treatments have shown beneficial effects in some patients, providing another avenue for pain management and recovery. However, their effectiveness varies among individuals and should be pursued under professional guidance.
When Surgery Becomes Necessary
Despite the effectiveness of traditional treatment methods, there are instances where surgical intervention becomes necessary to alleviate the symptoms of a pinched nerve in the neck. These circumstances generally fall into three categories:
- Severity of Symptoms: If symptoms are severe or progressively worsening despite conservative treatment, surgery may be required. These could include extreme pain, significant weakness or loss of motor function.
- Unresponsive to Non-Surgical Treatments: This includes cases where physical therapy, medication, and other non-surgical treatments have not resulted in substantial improvement after a reasonable period.
- Evidence of Nerve Damage: This is determined through diagnostic procedures like MRI or EMG. Persistent nerve compression can lead to permanent damage, making surgery essential.
When these conditions are present, surgery alternatives such as cervical decompression, discectomy, or fusion may be considered. Each surgical option carries its own risks and benefits, necessitating a thorough discussion with the healthcare provider.
Insurance considerations play a key role in the decision-making process. The cost, coverage, and out-of-pocket expenses for surgical procedures differ greatly, influencing the choice of treatment. Therefore, consultation with insurance providers is important to understand the financial implications before proceeding with surgery.
Preparing for Neck Surgery
As we pivot towards the topic of ‘Preparing for Neck Surgery’, two vital areas will be examined: Pre-Surgery Consultation Essentials and the Post-Operative Care Plan. The former will encompass key aspects such as patient evaluation, surgical risk assessment, and informed consent while the latter will elucidate on post-surgery management strategies, patient support, and rehabilitation. Through this analysis, we will provide a thorough view of the preparation process, equipping patients with knowledge to navigate their surgical journey.
Pre-Surgery Consultation Essentials
Before undergoing surgery for a pinched nerve in the neck, there are several important aspects to take into account during your pre-surgery consultation to guarantee a successful surgical outcome and ideal recovery.
- Addressing Consultation Anxieties: It’s vital to overcome any fear or apprehension about the upcoming surgical procedure. Open communication with your medical team can dispel myths and clarify expectations.
- Medical History Importance: A thorough review of your medical history is essential. This includes prior illnesses, surgeries, and allergies, as these can greatly influence the surgical approach and potential outcomes.
- Preoperative Evaluation: This involves a series of tests to assess your overall health status, ensuring your body’s readiness for surgery. These evaluations can range from blood tests to imaging studies, providing invaluable information for your surgeon.
Post-Operative Care Plan
Planning a thorough post-operative care strategy is an essential step in preparing for neck surgery, as it lays the groundwork for a smooth recovery and rehabilitation process. Pain management is a crucial element of this plan. Pain levels can be meticulously tracked and treated with a combination of pharmaceutical interventions and physical therapy. The use of non-opioid analgesics, anti-inflammatory drugs, and nerve blocks may be considered. Scar care is another integral part of the post-operative plan. The application of silicone sheets or gels can aid in reducing scar visibility. Regular inspection of the surgical site is crucial to detect any signs of infection. The plan should be designed meticulously, with a focus on the patient’s comfort and recovery.
Types of Surgery for Pinched Nerve
Often, three primary types of surgery are considered when treating a pinched nerve in the neck: Anterior Cervical Discectomy and Fusion (ACDF), Artificial Disc Replacement (ADR), and Posterior Cervical Foraminotomy.
- ACDF involves the removal of an intervertebral disc or bone spurs pressing on neural structures. After discectomy, the adjacent vertebrae are typically fused to provide stability.
- ADR is an alternative to ACDF, where an artificial disc is inserted instead of fusing the vertebrae. This maintains neck mobility post-surgery.
- Posterior Cervical Foraminotomy is a minimally invasive procedure where the surgeon works from the back of the neck, removing tissue to enlarge the neural foramen and alleviate nerve root compression.
While these surgeries can relieve symptoms, they come with varying surgery cost estimates. ACDF and ADR are more expensive than Foraminotomy due to the complexity of the procedures and the use of implants.
Following surgery, lifestyle changes are often necessary. These may include physical therapy, changes in physical activities, and adopting ergonomic practices at work or at home. It is important to follow the prescribed post-surgery routine to ensure excellent recovery and prevent recurrence of the pinched nerve.
Minimally Invasive Surgical Options
Minimally invasive surgical options for a pinched nerve in the neck offer promising outcomes with fewer complications. Procedures such as Cervical Microdiscectomy, Anterior Cervical Discectomy, and various Endoscopic Discectomy techniques will be examined thoroughly regarding their methodologies, benefits, and comparative effectiveness. This rigorous analysis will provide an understanding of the options available to patients seeking less invasive solutions.
Understanding Cervical Microdiscectomy
Cervical microdiscectomy, a minimally invasive surgical technique, is primarily employed to alleviate the debilitating symptoms associated with a pinched nerve in the neck by removing the herniated disc material causing the compression.
- Cervical microdiscectomy cost: The cost can vary considerably based on factors such as geographical location, surgeon’s experience, and the complexity of the case.
- Microdiscectomy success rate: This procedure has a high success rate, with a majority of patients reporting significant improvement in symptoms and return to daily activities post-surgery.
- Procedure: The surgery involves a small incision, through which a specialized microscope guides the surgeon to remove the problematic disc material, thereby releasing the pinched nerve and relieving pain.
This procedure represents a significant stride in minimally invasive spine surgery, promising effective relief with less surgical trauma.
Benefits of Anterior Cervical Discectomy
While the aforementioned cervical microdiscectomy represents a significant breakthrough in the domain of minimally invasive surgeries, another technique that has proven its efficacy in treating pinched nerves in the neck is the Anterior Cervical Discectomy. This method offers several benefits including high discectomy success rates and effective post discectomy pain management. A systematic review of multiple research studies indicates an average success rate of 92.7% for anterior cervical discectomy, testifying its reliability. Moreover, the anterior approach allows the surgeon to directly visualize and access the herniated disc, ensuring a more precise intervention. Postoperative pain is also effectively managed through a combination of pharmacological and physical therapies, resulting in enhanced patient comfort and a faster return to daily activities. This method combines efficacy, precision, and patient comfort.
Comparing Endoscopic Discectomy Techniques
In the domain of minimally invasive surgical options, an assortment of endoscopic discectomy techniques have emerged, each characterized by unique methodologies, advantages, and potential drawbacks that warrant rigorous comparative analysis.
- Endoscopic equipment advancements: The evolution of endoscopic tools has allowed for greater precision and less invasive operations. Advancements have ranged from the development of high-definition imaging systems to the refinement of surgical instruments, enabling efficient removal of the offending disc material.
- Surgeon’s skill proficiency: The efficacy of endoscopic discectomy largely depends on the surgeon’s expertise in manipulating the tools and interpreting the endoscopic images. Continuous training and experience play a significant role in influencing surgical outcomes.
- Technique variability: Different techniques present unique challenges and benefits. For instance, some methods may offer faster recovery times but require greater surgical proficiency. Therefore, a thorough understanding of these techniques is essential for excellent patient care.
Risks and Complications of Surgery
Exploring the intricate terrain of surgical intervention, it is important to take into account the potential risks and complications associated with a procedure for a pinched nerve in the neck. Despite the effectiveness of surgical alternatives, post-surgery complications may arise, which can greatly impact the patient’s health and recovery.
Largely, the risks fall into the categories of general surgical risks and those specific to the operation. General surgical risks include infections, blood clots, allergic reactions to anesthesia, and heart complications. Specific to the procedure, nerve damage is a significant risk factor. This could result in increased pain, sensory changes, or, in severe cases, paralysis.
Aside from these, there are potential post-surgery complications. These include failed back surgery syndrome (FBSS), characterized by chronic pain despite successful surgery. Other complications may include a recurrence of disc herniation, spinal fluid leaks, or pseudarthrosis (non-union of the fused bones).
While these risks and complications can be challenging, it is important to remember that modern surgical practices are designed to minimize these risks. They are rare, but understanding them is essential for informed patient decision-making and preparation. Deciding on surgical intervention should involve a thorough discussion with the healthcare team about these potential risks and complications.
Recovery and Rehabilitation
Post-operative care and structured rehabilitation form the cornerstone of recovery from surgery for a pinched nerve in the neck, necessitating a detailed understanding of the healing process, potential challenges, and strategies to regain strength and mobility. The recovery phase often involves a multidimensional approach that includes physical therapy benefits, pain management strategies and patient education.
- Physical Therapy: The benefits of physical therapy are manifold in the rehabilitation process. It provides patients with targeted exercises to improve neck strength and flexibility, thereby aiding in the best possible recovery. Physical therapists also educate patients on proper posture techniques to alleviate undue pressure on the neck.
- Pain Management: Pain management strategies are essential in the post-operative period. These strategies may include medication, nerve block injections, and alternative methods like acupuncture or massage therapy. Effective pain management not only enhances comfort but also facilitates active participation in physical therapy.
- Patient Education: Educating patients about their condition, the recovery process, and self-care strategies prove pivotal in successful rehabilitation. This involves teaching patients about the early warning signs of complications, the importance of regular follow-up visits, and adherence to prescribed therapy regimes.
In essence, a holistic approach to recovery and rehabilitation can greatly improve surgical outcomes, reduce the risk of complications, and expedite the return to normal activities.
Preventing Future Pinched Nerves
Understanding how to prevent future occurrences of pinched nerves in the neck requires a thorough understanding of the contributing factors, along with the implementation of proactive strategies that promote overall spinal health and well-being. The first preventive measure is regular exercise, which yields numerous benefits for spinal health. Exercise strengthens the muscles that support the spine, reducing the strain on the neck and decreasing the likelihood of nerve compression. A robust exercise regimen includes a mix of cardio, strength training, and flexibility exercises.
Another preventive strategy is posture correction. Poor posture, especially during prolonged periods of sitting or standing, can contribute to nerve compression in the neck. Ergonomic adjustments in the workplace, such as adjusting the height of your computer monitor or using a chair that supports the natural curve of your spine, can help promote better posture. Additionally, mindful practices like yoga and pilates can also help in the cultivation of proper alignment and body awareness.
Frequently Asked Questions
Can Physical Activities or Exercises Worsen a Pinched Nerve in the Neck?
Yes, certain physical activities or exercises can potentially exacerbate a pinched nerve in the neck. Nerve irritation prevention is vital, and maintaining proper posture importance cannot be overstated to avoid worsening the condition.
Is It Possible to Have a Pinched Nerve Without Experiencing Any Symptoms?
Yes, it is possible to have a symptomless pinching of a nerve, known as asymptomatic nerve compression. However, in most cases of nerve compression diagnosis, patients will experience some form of discomfort or pain.
How Can a Pinched Nerve Affect Other Parts of the Body?
A pinched nerve can affect other body parts through nerve compression consequences such as radiating pain, numbness, or weakness. Prevention can include maintaining good posture, regular exercise, and avoiding repetitive movements.
Can Alternative Therapies Like Acupuncture Help in Managing a Pinched Nerve?
Yes, acupuncture can be beneficial for managing a pinched nerve. As an alternative to traditional treatments, it may provide pain relief by stimulating the body’s natural healing processes and reducing inflammation in the affected area.
Does Age or Gender Influence the Likelihood of Getting a Pinched Nerve in the Neck?
Age and gender can influence the likelihood of developing a pinched nerve in the neck, but genetic predisposition and lifestyle factors such as physical activity and occupation play a more significant role.