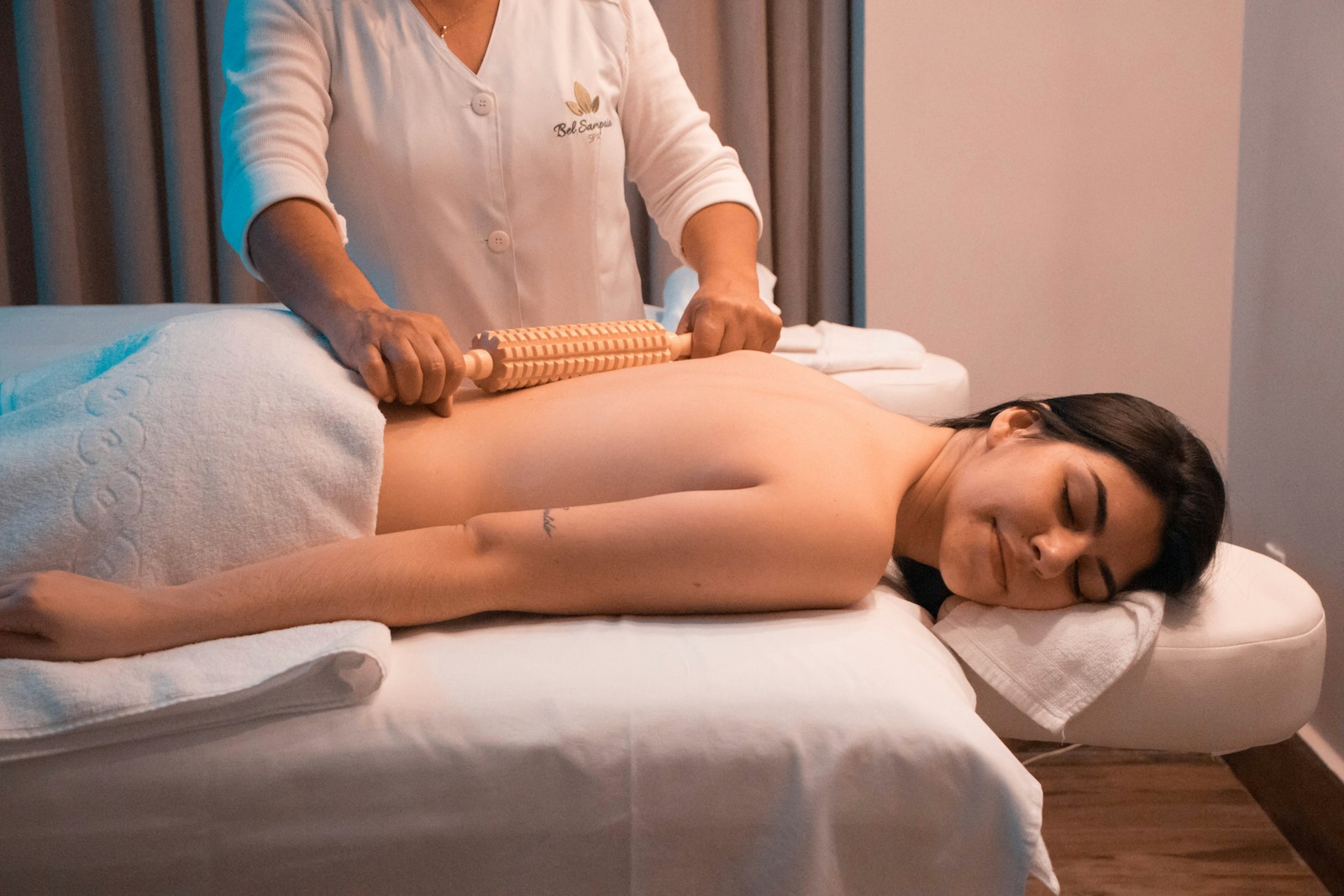
The utilization of physical therapy in the management of sciatica has been gaining considerable attention in the medical community. As a non-invasive and non-pharmacological intervention, it offers a valuable approach to mitigate the debilitating pain and functional impairment associated with sciatica. But how effective is it really? And what are the specific techniques that demonstrate the most promise? In examining these questions, we may uncover some intriguing insights into this widely practiced therapeutic strategy.
Understanding Sciatica
Sciatica, a term often misunderstood, is a medical condition characterized by pain radiating along the path of the sciatic nerve, which branches from the lower back through the hips and buttocks and down each leg. This condition can be both debilitating and persistent, often leading to misconceptions about its cause, severity, and treatment options.
One prevalent misconception is the notion that sciatica can only be effectively treated with invasive surgical procedures or potent pharmaceutical drugs. This belief often discourages individuals from exploring alternative remedies that may provide significant relief. For example, physical therapy, a non-invasive and drug-free approach, has been shown to alleviate sciatica symptoms effectively. Techniques such as stretching, strengthening exercises, and manual therapy can help to alleviate pressure on the sciatic nerve and improve functional mobility.
Another common misconception is that sciatica is a standalone diagnosis, which oversimplifies the condition. In reality, sciatica is a symptom of an underlying condition, often related to spinal issues such as disc herniation or spinal stenosis. Hence, a thorough understanding of sciatica requires an appreciation of the complexities of the condition and the importance of individualized treatment plans.
Causes of Sciatica
To fully grasp the complexities of sciatica, it is imperative to explore the various conditions and mechanisms that can lead to this neuropathic pain. Sciatica often results from conditions that exert pressure on the sciatic nerve, causing inflammation, irritation, and pain. Such conditions can include lumbar herniated disc, degenerative disc disease, and spinal stenosis. In rare cases, sciatica can also arise from direct nerve compression due to tumors or injury.
The associated conditions mentioned above can be exacerbated by certain lifestyle factors. A poor ‘Sciatica Diet’ lacking in anti-inflammatory foods can worsen the inflammation of the sciatic nerve. Foods high in sugar and trans fats can increase systemic inflammation and subsequently contribute to sciatic nerve pain. On the other hand, a diet rich in fruits, vegetables, lean proteins, and whole grains can help reduce inflammation and manage sciatica symptoms.
Additionally, obesity can increase the risk for sciatica since excess weight can add pressure to the spine and discs, leading to conditions like spinal stenosis or herniated disc. Other risk factors include age, as degenerative changes in the spine occur naturally with aging, and physical inactivity, which can lead to weight gain and spine problems.
Common Symptoms
Understanding the common symptoms of sciatica is essential for effective treatment and management. We will discuss the typical pain patterns associated with this condition and the impact these symptoms can have on daily activities. Accurate identification of these symptoms can help guide therapeutic interventions and improve patient outcomes.
Identifying Sciatica’s Common Symptoms
Often, individuals suffering from sciatica experience a range of symptoms, the most common of which include persistent pain in the lower back or hip, radiating down to the leg. Other symptoms may encompass numbness, tingling, or muscle weakness in the affected area. However, Sciatica Misconceptions often lead to an underestimation of these symptoms, with many attributing them to regular back or leg discomfort. This, coupled with Treatment Misunderstandings, can delay appropriate care, resulting in prolonged discomfort. Hence, it is important to correctly identify these symptoms. Importantly, the intensity of sciatica symptoms can vary, from infrequent and irritating to persistent and incapacitating. Early recognition of these symptoms is key to initiating appropriate management and physical therapy strategies.
Pain Patterns in Sciatica
The pain associated with sciatica typically follows a specific pattern, an important aspect that aids in its identification and subsequent management. This pattern can be characterized by sharp, burning pain that originates in the lower back or hip, radiating down the rear or leg. Despite Sciatica’s global prevalence, its pain pattern remains largely consistent across different populations. The intensity of the discomfort can vary from mild to severe, often aggravated by prolonged sitting. The manifestation of these symptoms provides key insights for healthcare professionals to formulate non-surgical interventions. These interventions aim to not only alleviate the pain but also manage the condition more effectively. Understanding the pain patterns in sciatica is vital in the overall treatment approach, ultimately improving the patient’s quality of life.
Impact on Daily Activities
Sciatica’s debilitating symptoms can greatly encroach upon an individual’s ability to perform daily activities, manifesting in various ways that range from difficulty in walking to disruptions in sleep pattern. The influence of sciatica extends to:
- Workplace Ergonomics: It can hinder an individual’s capacity to maintain proper postures, limiting productivity and engagement.
- Mobility: Sciatica may restrict movements, affecting routine tasks like walking or climbing stairs.
- Sleep Quality: The chronic pain can lead to sleep disturbances, reducing overall health and well-being.
- Psychological Impact: The persistent pain and subsequent limitations can lead to emotional distress and anxiety.
Understanding the extensive implications of these symptoms is critical in developing an effective physical therapy plan for sciatica. The goal is to restore function, alleviate pain, and improve the overall quality of life.
Diagnosing Sciatica
The process of diagnosing sciatica commences with a thorough understanding of the symptoms, which mainly includes lower back pain that extends down to the legs. Subsequently, a range of diagnostic tests such as MRI, CT scans, or electromyography may be employed to confirm the diagnosis and assess the severity of the condition. Interpreting the results of these tests will then allow healthcare professionals to devise a tailored treatment plan that best suits the patient’s needs.
Understanding Sciatica Symptoms
In order to accurately diagnose sciatica, it is important to thoroughly understand its various symptoms. Recognizing these symptoms can guide treatment strategies, including sciatica medication options.
The most common symptoms of sciatica include: – Persistent pain in one side of the buttock or leg, rarely on both sides – Pain that worsens when sitting – Sharp pain that may make it difficult to stand or walk – A constant pain on one side of the rear
The emotional impact of sciatica can also be significant, often leading to stress, anxiety, and depression. Understanding these symptoms is crucial in managing the condition effectively, and can help healthcare professionals devise a complete treatment plan.
Diagnostic Tests for Sciatica
Having recognized the symptoms of sciatica, it becomes necessary to undertake specific diagnostic tests to confirm the condition and determine its severity. Accurate diagnosis guides the selection of sciatica medication options and informs the need for surgical interventions. A physical examination, which may include tests for nerve root tension and muscle strength, is usually the first step. Further, imaging tests like an X-ray, MRI, or CT scan provide a detailed view of the spine and can reveal issues like a herniated disc or bone spurs. Electromyography (EMG) might be used to detect nerve conduction issues. Each of these tests offers varied insights into the patient’s condition, contributing to a thorough understanding of their sciatica and facilitating effective treatment planning.
Interpreting Sciatica Test Results
Upon completion of the necessary tests, careful interpretation of the results is imperative in diagnosing sciatica and formulating an effective treatment plan.
A proper understanding of the test results can greatly enhance test accuracy and reduce misdiagnosis risks. Here are some key aspects to take into account:
- Symptom Correlation: The findings should correlate with the patient’s symptoms. A negative result doesn’t always rule out sciatica.
- Repeatability: Consistent findings across multiple tests bolster the diagnosis.
- Clinical Context: Results should be interpreted in the context of the patient’s overall health and medical history.
- Limitations Awareness: Being aware of the limitations of each test can prevent overreliance on a single result, reducing misdiagnosis risks.
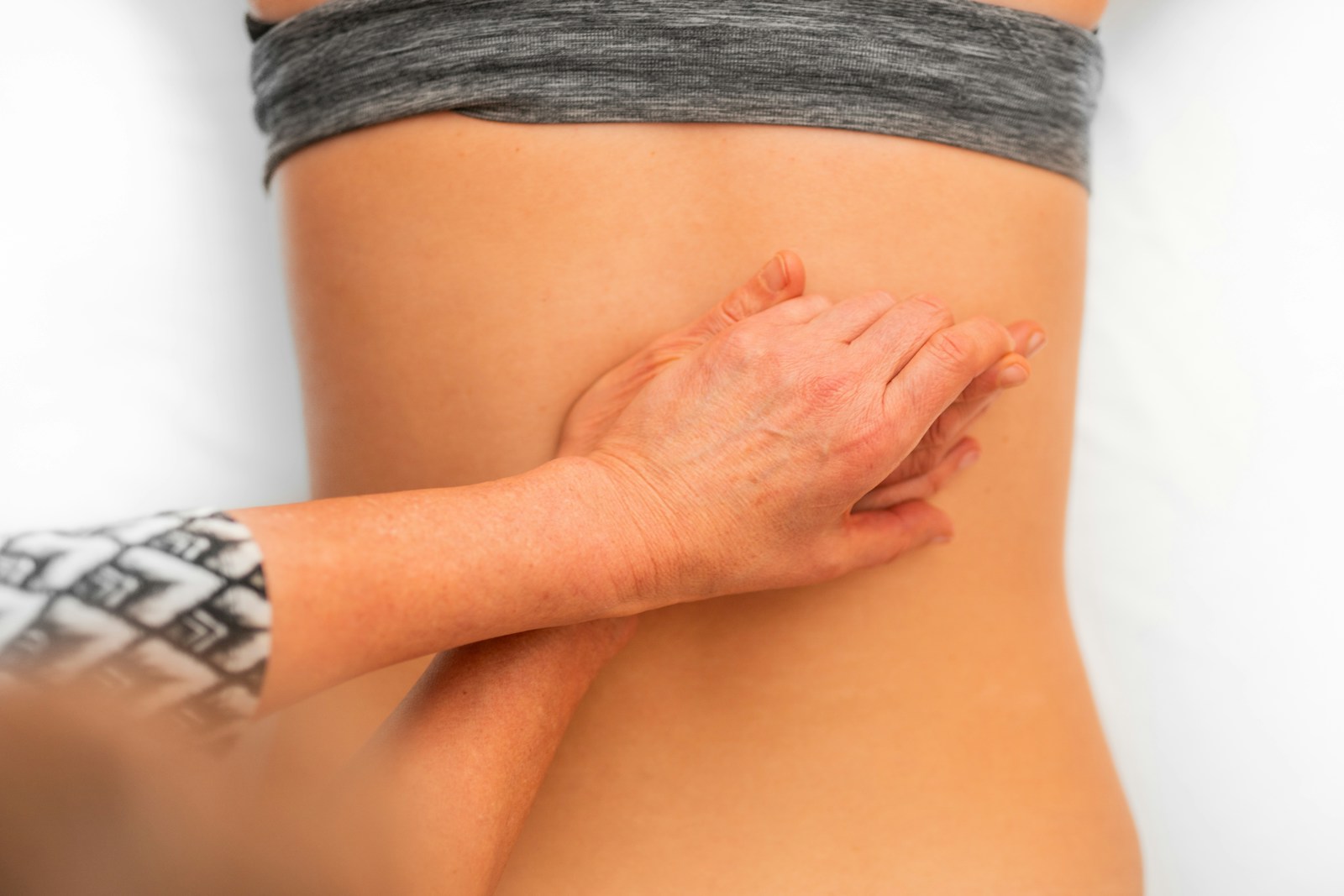
Role of Physical Therapy
Physical therapy plays a pivotal role in managing and alleviating the symptoms of sciatica, offering patients a non-invasive and often highly effective treatment option. The practice involves an array of therapy types, each tailored to address the unique needs and symptomatology of the patient.
Through modalities like manual therapy, exercise therapy, and electrotherapy, physical therapists work to enhance mobility, improve strength, and reduce pain. Manual therapy involves hands-on techniques to improve joint and soft-tissue mobility, while exercise therapy includes targeted movements designed to enhance strength and flexibility. Electrotherapy utilizes electrical equipment to stimulate nerves and muscles, aiding in pain relief and muscle re-education.
The usage of specialized equipment further enhances the efficacy of physical therapy. Equipment such as exercise balls, resistance bands, and specialized machines are used to aid in stretching, strengthening, and restoring normal function. The application of thermal modalities, like heat and cold therapy, can also help in managing inflammation and pain.
The role of physical therapy in sciatica management is thus multifaceted, encompassing a range of therapy types and equipment usage, all aimed at reducing pain, improving function, and enhancing quality of life for patients.
Benefits of Physical Therapy
When managing sciatica, the benefits of physical therapy are multifaceted and significant. Not only does it focus on enhancing mobility and strength, but it also provides a natural, non-invasive method of reducing pain. Understanding these benefits can guide patients in their journey towards improved quality of life and best health outcomes.
Enhancing Mobility and Strength
Through a customized regimen of exercises and stretches, physical therapy can greatly enhance mobility and overall strength, thereby easing the pain and discomfort associated with sciatica. Physical therapy sessions focus on targeted movements that improve flexibility, strengthen the back muscles, and promote healthier posture.
Key components of this therapeutic approach include:
* Posture Corrections: Therapists teach patients how to maintain proper posture to reduce strain on the lower back, thereby mitigating sciatica symptoms.
* Equipment Usage: Therapeutic tools such as resistance bands and stability balls are often used to enhance strength-building exercises.
* Individualized Exercise Programs: Tailored to address each patient’s unique needs and capabilities.
* Education: Empowering patients with knowledge about their condition, helping them to avoid future episodes.
This proactive approach fosters self-management of sciatica symptoms and enhances overall physical wellbeing.
Reducing Pain Naturally
One’s journey towards natural pain relief, especially for sciatica, can be greatly facilitated by the myriad benefits offered by physical therapy. This therapeutic approach not only improves physical mobility but also promotes natural pain reduction through dietary adjustments and mental health improvements. A balanced diet with anti-inflammatory foods can help manage sciatica symptoms, enhancing the effectiveness of physical therapy treatments. Additionally, mental health is intrinsically linked to pain perception. Through techniques such as cognitive-behavioral therapy, patients can learn to cope with their pain better, reducing its impact on their everyday lives. Incorporating these elements into a holistic treatment plan can significantly enhance the benefits of physical therapy, leading to a more substantial and long-lasting relief from sciatica pain.
Sciatica Specific Exercises
A multitude of exercises specifically tailored for sciatica can greatly aid in alleviating the pain associated with this condition and enhancing overall physical functionality. Involving exercise variations can guarantee the targeting of specific areas, thereby increasing the effectiveness of the exercise regimen. Yoga benefits, too, can be significant as it encourages flexibility, strength, and the reduction of stress.
The following list includes some of the exercises recommended for sciatica:
- Knee to chest stretch: This exercise helps to loosen the piriformis and buttock muscles, which can become inflamed and press against the sciatic nerve, causing pain.
- Sciatic mobilizing stretch: This stretch can help to mobilize the sciatic nerve and reduce the intensity of the pain.
- Back extensions: This exercise aids in stretching and mobilizing the spine backward, counteracting the natural inclination to hunch forward.
- Standing hamstring stretch: This stretch helps to elongate the hamstring muscle, which can be indirectly involved in sciatica pain.
Each of these exercises aims to relieve sciatica pain by stretching and strengthening specific muscles. It’s important to remember, however, that consistency is key when it comes to exercising for sciatica. Regular, daily practice can yield the best results.
Pain Management Strategies
In addition to exercise, employing a variety of pain management strategies can greatly alleviate the discomfort associated with sciatica. These strategies encompass a range of treatments, from alternative therapies to surgical options, each with its own unique benefits and considerations.
Alternative therapies, for instance, can include acupuncture, massage, and chiropractic adjustments. Acupuncture can target specific points along the sciatic nerve pathway to relieve pain and inflammation. Massage therapy, on the other hand, can help relax the muscle tension that may exacerbate sciatica symptoms. Chiropractic adjustments can realign the spine to reduce nerve irritability, thereby improving the patient’s mobility and pain.
Surgical options, while generally considered a last resort, can be highly effective for individuals with severe or persistent sciatica. These procedures aim to remove the root cause of the sciatica, whether it’s a herniated disc, bone spur, or spinal stenosis. Discectomy, for instance, involves removing the portion of the disc that’s pressing on the sciatic nerve. Laminectomy, alternatively, removes part of the vertebra to create more space for the nerves. Each surgical option requires careful consideration and consultation with healthcare providers to guarantee patient safety and efficacy.

Lifestyle Modifications
Beyond therapeutic interventions, certain alterations in daily habits can greatly impact the management and prevention of sciatica symptoms. Lifestyle modifications are crucial in achieving ideal health outcomes.
A critical aspect of these modifications is dietary changes. An anti-inflammatory diet, rich in fruits, vegetables, lean proteins, and healthy fats, can alleviate sciatica symptoms. The diet aids in reducing inflammation, a primary cause of sciatica pain.
Mental wellness is another key factor in managing sciatica. Chronic pain can lead to anxiety and depression, worsening the pain perception. Regular mindfulness practices, such as meditation and yoga, can help manage the emotional aspect of chronic pain.
Additionally, maintaining a healthy body weight and engaging in regular physical activity can reduce the stress on the sciatic nerve, thereby managing pain and preventing further complications.
In summary, the following lifestyle modifications are recommended:
- Adopting an anti-inflammatory diet
- Regular mindfulness practices for mental wellness
- Maintaining a healthy body weight
- Regular physical activity
These changes, along with prescribed physical therapy, can greatly improve the quality of life for those living with sciatica.
Preventing Sciatica Recurrence
While lifestyle modifications play an undeniable role in managing sciatica symptoms, they are equally important in preventing the recurrence of this debilitating condition. Dietary changes and sleep positions are two key aspects that can greatly influence the likelihood of a sciatica recurrence.
In terms of dietary changes, maintaining a healthy weight is essential. Excess weight can put undue pressure on the spine, exacerbating sciatica symptoms and potentially leading to a recurrence. A balanced diet rich in anti-inflammatory foods like fruits, vegetables, lean proteins, and whole grains can help manage inflammation, a key factor in sciatica pain. Additionally, staying well-hydrated is crucial to keep spinal discs healthy, further reducing the risk of sciatica.
When it comes to sleep positions, the goal is to keep the spine in a neutral alignment. Sleeping on the back with a pillow under the knees or on the side with a pillow between the knees can help achieve this alignment, minimizing the strain on the sciatic nerve. Furthermore, investing in a supportive mattress and pillow can enhance the benefits of these positions.
Preventing sciatica recurrence requires a holistic approach, including dietary changes, strategic sleep positions, and regular physical therapy.
Success Stories of Physical Therapy
Numerous individuals suffering from sciatica have experienced significant relief and improvement through the application of physical therapy, showcasing its effectiveness in managing and potentially eliminating this painful condition. There are countless inspirational recoveries, demonstrating the transformative power of physical therapy in treating sciatica.
Among these success stories, we find a range of unconventional treatments and approaches that have proven to be effective:
- A 60-year-old marathon runner regained her stride after weeks of physical therapy that focused on stretching, strengthening, and postural exercises.
- A 35-year-old office worker, who had been dealing with debilitating sciatica for years, found relief through aquatic therapy, an unconventional treatment that reduces pressure on the spine while allowing increased mobility.
- A 50-year-old carpenter returned to his work after a series of manual therapy sessions involving hands-on techniques to improve spinal alignment and mobility.
- A 45-year-old teacher was able to return to her active lifestyle after a specialized treatment plan involving nerve gliding exercises and yoga.
These stories, among many others, underscore the potential of physical therapy in achieving long-term relief from sciatica. They illustrate the capacity for innovative and personalized therapeutic strategies to restore quality of life to those struggling with this condition.
Frequently Asked Questions
Can Sciatica Cause Permanent Nerve Damage?
Yes, untreated severe sciatica can potentially lead to permanent nerve damage. This underlines the importance of nerve damage prevention and early treatment to avoid such sciatica complications. Always consult a healthcare professional for proper diagnosis and treatment.
Are There Specific Diets to Help Manage Sciatica?
Yes, certain diets can aid in managing sciatica. Incorporating anti-inflammatory foods, understanding the food inflammation connection, and focusing on dietary pain reduction may help alleviate symptoms and improve overall nerve health.
How Does Weather Affect Sciatica Pain?
Weather sensitivity can potentially impact sciatica pain, with patients reporting increased discomfort during cold, damp conditions. Seasonal flare ups may occur, particularly in winter, due to changes in atmospheric pressure and decreased physical activity.
Does Pregnancy Increase the Risk of Sciatica?
Yes, pregnancy can increase the risk of sciatica. This is often due to pregnancy postures and weight gain that can put pressure on the sciatic nerve, triggering sciatica symptoms such as lower back pain and leg discomfort.
Can Sciatica Affect Sexual Performance?
Sciatica can potentially affect sexual performance due to discomfort or pain. However, modifying sexual positions can aid in sciatica pain management, allowing individuals to maintain sexual activity without exacerbating symptoms. Consult a health professional for personalized advice.