Spinal injuries, ranging from minor to severe, can profoundly impact an individual’s quality of life, necessitating a thorough understanding of their various types and implications. These conditions, encompassing spinal fractures, dislocations, spinal cord compression, and herniated discs, present unique challenges in diagnosis and treatment. As we navigate through this intricate topic, we shall explore each type of injury, its causes, symptoms, diagnostic procedures and available treatment options. With this knowledge, we can better understand how to prevent future injuries and manage existing ones effectively. Join us as we journey into this crucial aspect of human health.
Understanding the Spinal Structure
To fully understand the various types of spine injuries, it is essential to first explore the intricate structure of the spinal column, a complex assembly of vertebrae, discs, nerves, and muscles. This assembly is not merely a rigid rod, but a flexible and dynamic entity, with each component serving a specific function, making the spinal anatomy basics an integral part of this discussion.
The vertebral column, also known as the spinal column, serves as the main support structure for the body, enabling us to stand upright, bend, and twist. It is made up of 33 vertebrae, cushioned by intervertebral discs that absorb shock and allow flexibility. These vertebrae are divided into regions: cervical, thoracic, lumbar, sacral, and coccyx, each providing a different level of support and mobility.
This column houses and protects the spinal cord, the main pathway for communication between the brain and the rest of the body. Any damage to the spinal structure can disrupt this communication, leading to temporary or permanent physical impairments.
Understanding the vertebral column functions and its complex structure is therefore an important step in recognizing and diagnosing spinal injuries.
Common Causes of Spine Injuries
Having established a fundamental understanding of the spinal structure, we now turn our attention to the various factors that commonly lead to spine injuries.
Spine injuries can be attributed to a multitude of causes, frequently falling into two main categories: traumatic and non-traumatic. Traumatic injuries often result from specific incidents such as car accidents, falls, sports injuries, or violent encounters. Non-traumatic injuries, on the other hand, tend to develop over time due to factors like aging, lifestyle habits, and occupational hazards.
In the context of occupational hazards, workers in industries involving heavy lifting or prolonged periods of sitting or standing are at a higher risk. Similarly, athletes and physically active individuals are more susceptible to spinal injuries due to the increased strain on their backs.
Implementing injury prevention measures is essential in mitigating these risks. These can range from adhering to proper lifting techniques in the workplace to maintaining a regular exercise routine to strengthen the back muscles. Promoting awareness of these causes and prevention methods is a crucial step towards reducing the prevalence of spinal injuries. As we move forward, understanding the cause is the first step in prevention and treatment.
Minor Spine Injuries Explained
Minor spine injuries, while less severe than major ones, still require accurate identification and appropriate treatment. A clear understanding of these injuries, their symptoms, and the necessary therapeutic interventions is vital to guarantee a successful recovery. We will now explore these aspects in detail, along with the rehabilitation process that facilitates a return to normal functionality.
Identifying Minor Spine Injuries
In the domain of spinal injuries, it is important to understand how to identify less severe or minor spine injuries and comprehend their potential implications. Minor spine injuries often result in slight discomfort, minimal disruption to spinal alignment, and are typically caused by strains or sprains. Early identification plays a significant role in injury prevention. Symptoms can include localized pain, stiffness or difficulty moving, and minor swelling. Some people may experience temporary numbness or tingling in extremities. While these injuries are usually not life-threatening, they should never be ignored. Unaddressed, they can lead to chronic pain or further injury. It is advisable to seek professional advice if symptoms persist or worsen over time.
Treatment for Minor Injuries
When addressing the treatment of minor spine injuries, it is important to take into consideration the nature and extent of the injury, as well as the patient’s overall health and lifestyle. Effective treatment often involves a combination of physical therapy, medication, and lifestyle modifications such as posture correction. Regarding injury prevention, maintaining a strong, flexible spine through regular exercise is paramount. Posture correction plays a vital role in minimizing the risk of recurrent injuries. It is crucial to sit, stand, and lift objects correctly to protect the spine. Prescription and over-the-counter pain relievers may be used to manage pain. Additionally, non-surgical interventions such as chiropractic adjustments or acupuncture may also provide relief. By adopting these measures, minor spine injuries can be successfully treated.
Recovery and Rehabilitation Process
After the successful treatment of minor spine injuries, the next phase involves a thorough recovery and rehabilitation process to restore full function and prevent future injuries. This process often includes a combination of pain management techniques and mobility aid usage, designed to facilitate return to normal activities. Pain management techniques can range from medications to non-pharmacological interventions like physiotherapy and cognitive-behavioral therapy. These therapies aim to reduce pain, mitigate discomfort, and enhance the patient’s quality of life. Mobility aid usage, including the use of walkers, crutches, or wheelchairs, is also crucial in this phase. They provide support, improve balance, and promote independent movement. The ultimate goal is to promote excellent healing, improve physical function, and prevent re-injury.
Severe Spinal Cord Damage
A significant proportion of spinal injuries, severe spinal cord damage stands as one of the most debilitating conditions that can drastically alter the life of an individual. Characterized by the sudden loss of normal spinal cord function, this injury can lead to the spinal shock phenomenon. This condition typically manifests shortly after the injury and can last for several weeks, causing temporary or persistent symptoms such as loss of sensation, reflex function, and motor control below the level of the injury.
The implications of severe spinal cord damage extend beyond the immediate physical effects. Paralysis, a common result of severe spinal cord damage, can be either partial or complete, affecting the patient’s ability to move parts or all of their body. This often necessitates long-term rehabilitation and significant lifestyle modifications.
Furthermore, severe spinal cord damage can also lead to secondary complications including respiratory issues, bladder and bowel dysfunction, and neuropathic pain. The management of these complications forms an integral part of the overall treatment strategy, underscoring the complexity and far-reaching impacts of severe spinal cord damage.
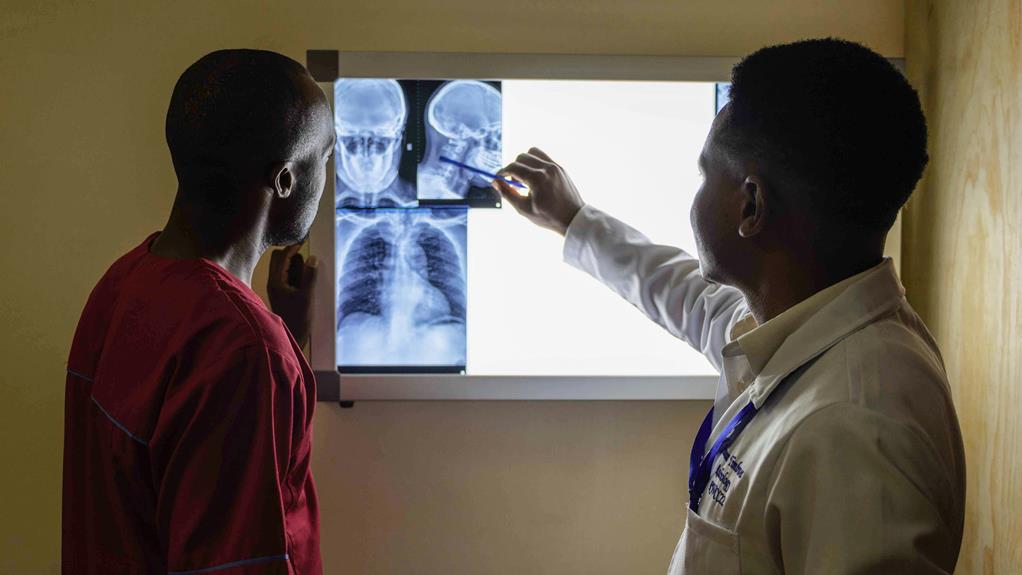
Spinal Fractures and Dislocations
Moving beyond the domain of severe spinal cord damage, it is pertinent to explore another category of spinal injuries – spinal fractures and dislocations. These injuries can manifest in various forms, each with its unique fracture classification and dislocation consequences.
Fracture classification is critical for understanding the severity and potential repercussions of a spinal fracture. It is primarily based on the type of force that caused the fracture, the specific area of the spine involved, and the stability of the affected region. Common types include compression fractures, burst fractures, flexion-distraction fractures, and fracture-dislocations.
Dislocation consequences, on the other hand, refer to the possible outcomes of a spine dislocation. These can range from mild discomfort to severe pain, reduced mobility, and even paralysis in extreme cases. Dislocations typically occur when extreme force is applied to the spine, causing the vertebrae to move out of their normal position. These can be pure dislocations, where there is no associated fracture, or fracture-dislocations, where the dislocation is accompanied by a fracture.
Both spinal fractures and dislocations require immediate medical attention to prevent further damage and ensure optimal recovery.
Understanding Spinal Cord Compression
Exploring further into the domain of spinal injuries, it is essential to comprehend the intricacies of spinal cord compression, a condition characterized by undue pressure on the spinal cord. This pressure can result from a variety of factors, such as tumors, spinal deformities like scoliosis, or osteoarthritis.
Compression consequences are diverse and largely dependent on the severity and location of the compression. These may range from mild discomfort or numbness to severe pain, muscle weakness, and in extreme cases, paralysis. The level of impairment can vary greatly, with some individuals retaining full mobility while others may experience significant loss of function.
Recognizing the symptoms early is vital for effective management. Non surgical interventions can often alleviate symptoms and slow progression. These may include physical therapy, pain management techniques, and medication for inflammation and pain. Depending on the severity, braces or assistive devices may also be recommended to support mobility and independence. In some cases, where non surgical interventions are insufficient, surgical intervention might be required to relieve pressure on the spinal cord.
Herniated Discs: A Closer Look
Delving deeper into the world of spinal injuries, we now turn our attention to the complex issue of herniated discs, a common yet often misunderstood condition. A herniated disc, also known as a slipped or ruptured disc, occurs when the soft interior of a spinal disc protrudes through the outer layer. This can apply pressure on adjacent nerves and cause significant discomfort.
There are several disc herniation myths that can confuse sufferers. To begin with, a herniated disc does not automatically require surgery. Yes, surgical interventions are an option, but they are usually reserved for severe cases where conservative methods like physical therapy and medication have failed. Additionally, a herniated disc is not exclusively an injury of the elderly; it can occur in younger individuals due to factors such as excessive strain or trauma.
Surgical interventions for herniated discs range from minimally invasive procedures to more complex surgeries. A microdiscectomy, for instance, involves removing only the portion of the disc that’s pressing on the nerve. In contrast, a spinal fusion surgery involves fusing two or more vertebrae together to restrict movement and alleviate pain. Each surgical intervention carries its own risks and benefits, necessitating careful consideration and consultation with a spine specialist.
Symptoms Associated With Spine Injuries
Recognizing symptoms associated with spine injuries is essential for early detection and treatment. These symptoms can range from obvious physical manifestations such as pain or limited mobility, to less visible but equally significant psychological effects. This section will explore these varied symptoms in detail, highlighting their importance in the diagnosis and management of spine injuries.
Identifying Spine Injury Symptoms
In the domain of medical science, identifying symptoms associated with spine injuries is of paramount importance, as these signs often serve as the preliminary indicators of severe conditions, warranting immediate attention and intervention.
Symptoms can vary greatly depending on the severity and location of the injury, but three essential indicators often observed are:
- Persistent or worsening back or neck pain, often demanding the implementation of pain management techniques
- Impact on mobility, which might manifest as difficulty walking or moving limbs
- Changes in bodily functions like bowel or bladder control
These symptoms should never be ignored. Early identification can lead to prompt treatment, potentially minimizing the risk of long-term damage. Therefore, understanding these symptoms is critical in the overall management of spine injuries.
Common Physical Manifestations
Expanding on the initial indicators of spine injuries, there are numerous physical manifestations that can provide further insight into the nature and severity of the condition. These symptoms can range from mild discomfort to debilitating pain, impacting mobility to varying degrees. For instance, difficulty in walking, loss of balance, or even paralysis can be observed. Other physical signs may include muscle spasms, reduced sensitivity to heat and cold, or changes in bladder and bowel function. Understanding these manifestations is essential not only for diagnosis but also for spine injury prevention. By recognizing these symptoms promptly, appropriate medical intervention can be sought, potentially limiting the damage and improving the long-term prognosis of those affected by spine injuries.
Psychological Effects of Injuries
How often do we consider the psychological impact that spine injuries can have on an individual? The effects are not merely physical; they extend into the sphere of mental and emotional health.
- Mental resilience strategies become critical in coping with the aftermath of such injuries. The patient needs to develop a mindset capable of overcoming adversity and embracing change.
- There are significant emotional adjustment challenges. Patients may grapple with feelings of loss, anger, or depression as they adapt to their new circumstances.
- Social isolation is another issue, as mobility restrictions can limit social interactions, leading to loneliness and further emotional distress.
Understanding these psychological implications can aid in providing holistic care for spine injury patients.
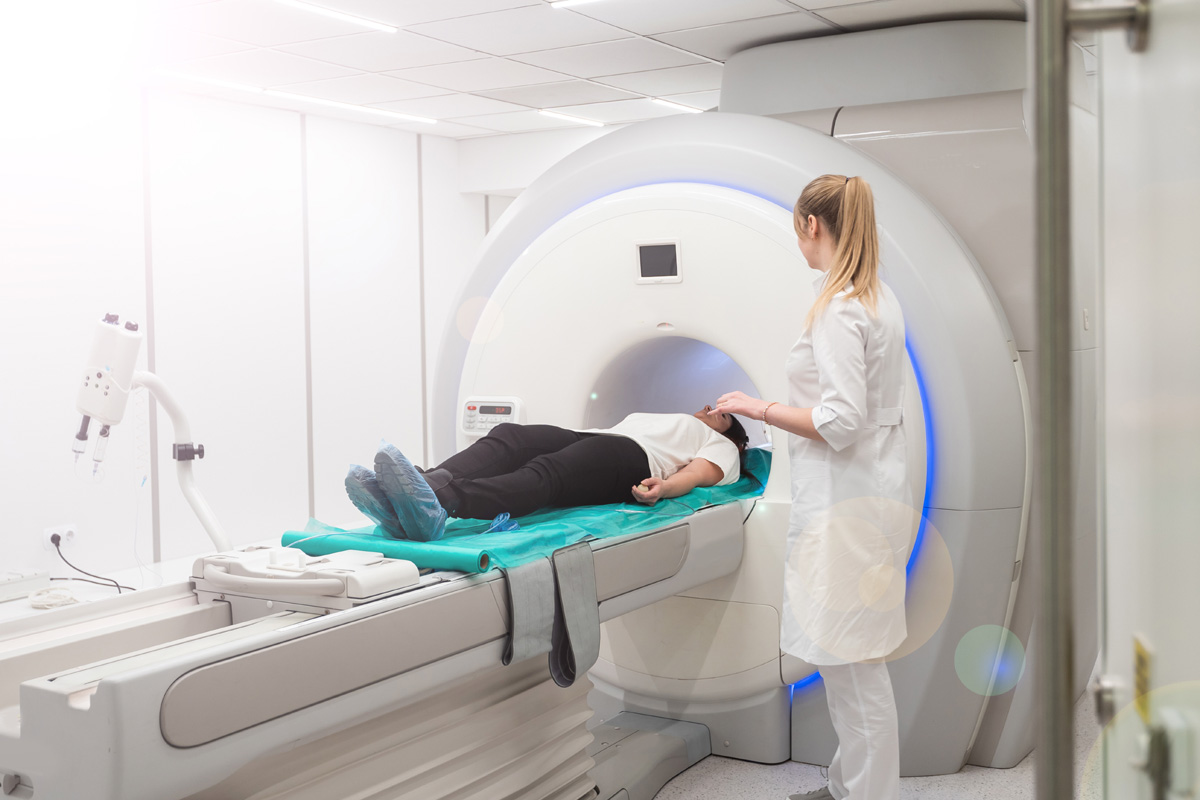
Diagnostic Procedures for Spine Injuries
To accurately diagnose spine injuries, a variety of medical procedures may be utilized, each offering a unique perspective on the patient’s condition. Breaking away from spinal injury myths, medical practitioners rely heavily on diagnostic accuracy to guarantee the correct identification of the injury type and degree of severity.
The diagnostic process often starts with a physical examination. This includes assessment of symptoms, patient history, and neurological function. However, physical examination alone may not provide a full understanding of the injury. As a result, imaging tests such as X-rays, Magnetic Resonance Imaging (MRI), and Computed Tomography (CT) scans are commonly employed. X-rays can reveal fractures or dislocations, while MRI and CT scans provide a more detailed view of soft tissues, including the spinal cord and nerves.
Other diagnostic procedures like a discogram or myelogram might be used to evaluate the intervertebral discs or the spinal canal respectively. In some cases, electromyography (EMG) may be utilized to assess nerve function. The chosen procedures depend on the suspected injury and the patient’s specific symptoms. Regardless of the method, the aim remains consistent: to achieve the highest level of diagnostic accuracy for the most effective treatment plan.
Treatment Options for Spine Injuries
Once a spine injury has been accurately diagnosed, a thorough, personalized treatment plan is meticulously developed to address the specific needs and objectives of the patient. This plan takes into account the type and severity of the injury, the patient’s overall health status, their lifestyle, and their injury prognosis.
The primary goal of treatment for spine injuries is to manage pain, restore function, and prevent further injury. To achieve this, a combination of conservative treatments and surgical procedures may be recommended.
Some common treatment options include:
- Surgery: This is typically reserved for severe cases where conservative treatments have failed or if the patient’s neurological function is at risk. The type of surgery will vary based on the injury.
- Physical Therapy: This form of therapy aims to strengthen the muscles that support the spine and improve flexibility and mobility.
- Medications: Pain relievers, muscle relaxants, and anti-inflammatory drugs are often used to manage pain and inflammation.
In addition, alternative therapies such as acupuncture, massage, and chiropractic treatment may be considered. These therapies can complement traditional treatments and play a significant role in the patient’s recovery and rehabilitation process.
Preventing Future Spine Injuries
Ensuring the preservation of one’s spinal health is paramount to preventing future spine injuries. This involves debunking injury myths, adopting safe practices, and embracing innovative protective gear.
Firstly, let’s debunk injury myths. A common myth is that spine injuries only occur from high-impact activities. In truth, repeated stress or poor posture can also lead to injuries. Hence, maintaining a correct posture and taking regular breaks from sedentary positions are essential.
Secondly, regular exercise should be incorporated into one’s lifestyle. Strengthening core muscles can provide better support for the spine, reducing the risk of injury. Exercise also improves flexibility and posture, thereby further protecting the spine.
Lastly, the importance of using innovative protective gear cannot be overstated. For individuals involved in high-risk activities, such as contact sports or heavy lifting, specialized spinal protection can greatly reduce the risk of injury. Modern technology has given us advanced lightweight materials that offer high levels of protection without hindering mobility.
Frequently Asked Questions
What Is the Recovery Time for Different Types of Spine Injuries?
Recovery time for spine injuries varies greatly depending on severity and type. Emphasis on injury prevention and exploration of surgical options can influence recovery. It ranges from weeks for minor injuries to years for major ones.
How Can Spine Injuries Affect Ones Mental Health?
Spine injuries can greatly affect mental health, potentially leading to conditions like anxiety and depression. Emotional resilience post injury is essential for recovery. Managing anxiety after spine injuries involves psychological support and appropriate therapeutic interventions.
Can Spine Injuries Cause Other Health Problems in the Long Term?
Yes, spine injuries can lead to long-term health problems such as chronic pain, mobility issues, injury-induced insomnia, and complications from related surgeries. As a result, spine injury prevention is essential to maintain overall health and wellbeing.
What Are Some Exercises Recommended for Spine Injury Rehabilitation?
Rehabilitation exercises for spine injuries include gentle stretching, core strengthening, and balance training. Spinal braces provide support during recovery. Aquatic therapy is also effective, as it allows low-impact movement in a buoyant environment, promoting healing.
Are There Support Groups Available for People With Severe Spine Injuries?
Yes, there are numerous support groups for individuals with severe spine injuries. These groups provide emotional support, financial assistance options, and information on accessibility innovations to enhance the quality of life of those affected.