In the ever-evolving realm of medicine, surgical interventions stand as a crucial cornerstone, encompassing a myriad of procedures with varying degrees of complexity. As we scrutinize its historical evolution, delve into categories of surgical procedures, and explore the role of technology, we look to stimulate a discourse that encompasses not only the present state of this critical field but also its future. As we embark on this journey, we invite you to join this intellectual exploration, promising a wealth of knowledge that could potentially shape our understanding of this indispensable aspect of medical science.
Understanding Surgical Interventions
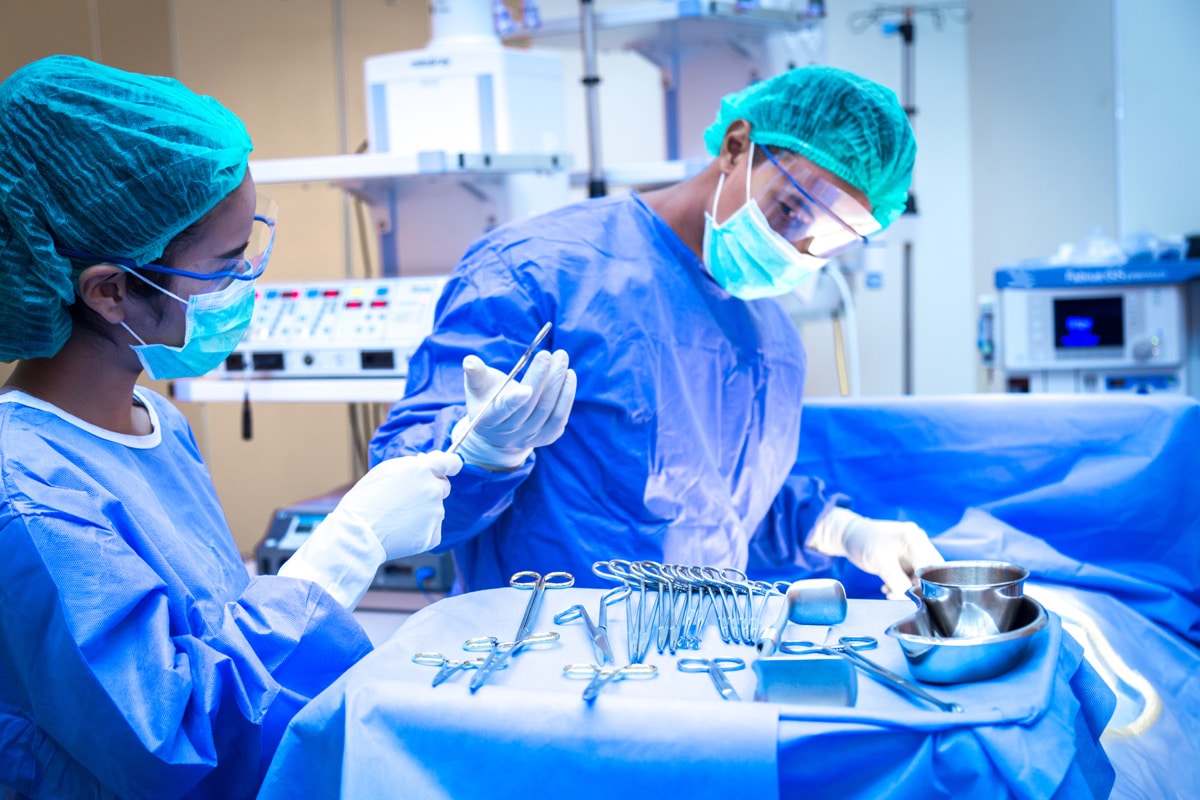
In the realm of modern medicine, surgical interventions stand as a vital tool, their understanding crucial for both healthcare professionals and patients alike, as they provide a direct, often efficient, solution to a myriad of health complications. Two key aspects of these interventions are surgical sterilization and patient consent, both of which are imperative for a successful and ethical surgical procedure.
Surgical sterilization refers to the process of eliminating all microbial life, including highly resistant spores, from the surgical instruments and operative field. This ensures a safe environment, minimizing the risk of postoperative infections, which according to the World Health Organization, is one of the top concerns in surgical safety.
Equally important is the issue of patient consent. Informed consent, a principle undergirded by legal and ethical standards, entails that a patient voluntarily agrees to a proposed surgical intervention after understanding its nature, purpose, risks, benefits, and alternatives. Evidence-based studies reveal that inadequate patient consent can lead to litigation, thus emphasizing its importance.
Historical Evolution of Surgeries
The historical trajectory of surgical interventions encapsulates a journey from rudimentary ancient practices to today’s sophisticated advancements. A comprehensive evaluation of this evolution requires a thorough review of the significant milestones, including the shift from empirical, often perilous, ancient surgical practices to the safer, evidence-based modern surgical procedures. The transformation has been underpinned by a variety of factors such as scientific breakthroughs, technological innovations, and an enhanced understanding of human anatomy and physiology.
Ancient Surgical Practices
Dating back to the Stone Age, ancient surgical practices, underscored by archaeological evidence such as trepanned skulls and rudimentary surgical tools, provide critical insights into the historical evolution of surgeries. Ancient civilizations including Greeks, Egyptians, and Indians laid the foundation for surgical trainings in antiquity. These training methods were often based on trial and error, with a focus on observation and practice. A wealth of knowledge on human anatomy was accumulated through these practices, which are documented in texts like the ‘Sushruta Samhita’. Alongside, use of ancient medicinal plants played a significant role in surgery. Plants like willow bark, myrrh, and opium were used as analgesics and antiseptics, underscoring the integrative approach of ancient surgical practices.
Modern Surgical Advancements
Transitioning from rudimentary methods, the evolution of surgeries underwent a paradigm shift with the advent of modern surgical advancements, characterized by the integration of scientific knowledge, technological innovation, and surgical expertise.
Modern surgical advancements include:
– Telemedicine surgeries: Enabled by robust communication networks, these allow surgeons to perform operations remotely, overcoming geographical barriers.
– Nano technology applications: They have revolutionized drug delivery and cancer treatment, significantly improving patient outcomes.
– Advanced imaging techniques: These provide clearer and more accurate diagnostic insights, leading to more effective surgical interventions.
– Robotic surgery: This advancement improves precision, reduces human error, and shortens recovery time.
These advancements demonstrate how the marriage of technology and medical science has revolutionized surgical interventions, transforming patient care and outcomes.
Categories of Surgical Procedures
Surgical procedures can be broadly classified into major and minor surgeries, elective procedures, and emergency surgeries. Major and minor surgeries are differentiated by the level of invasiveness and complexity, while elective procedures are those that are scheduled in advance, as they are not urgent. Conversely, emergency surgeries are critical interventions that need to be performed immediately due to life-threatening conditions.
Major Versus Minor Surgery
Delineating the differences between major and minor surgeries, it is imperative to understand that the categorization of surgical procedures primarily hinges on the complexity of the operation, the degree of risk involved, and the patient’s recovery time. This directly impacts surgery psychology and surgery costs.
- Major surgeries usually involve high complexity, potentially extensive recovery periods, and significant risks. Examples include open-heart surgery or organ transplants.
- Minor surgeries typically have fewer complexities, shorter recovery times, and lower risks. They often involve superficial alterations, like mole removals.
- Surgery psychology plays a pronounced role in major surgeries due to the potential for high stress and anxiety levels.
- Surgery costs can fluctuate wildly, with major surgeries generally costing significantly more than minor ones due to resources required.
Thus, understanding these distinctions is crucial for patient preparation and decision-making.
Elective Surgical Procedures
In addition to the categorization based on complexity, risk, and recovery time, surgical procedures can also be classified into elective or emergency procedures, with elective surgeries offering unique characteristics that merit close examination. Elective procedures, unlike emergency ones, are preplanned and non-life-threatening, allowing patients and providers significant leeway in scheduling. Interestingly, this flexibility has fueled surgical tourism trends, with patients often opting to receive surgery in foreign countries due to cost-effectiveness, advanced technology, or superior expertise. However, such trends have implications for insurance coverage nuances, as policies may not fully cover overseas procedures. Furthermore, elective procedures may be postponed due to insurance pre-approvals, potentially impacting patient outcomes. Hence, understanding these aspects is crucial for informed decision-making in elective surgical procedures.
Emergency Surgery Essentials
Contrary to elective surgeries, emergency surgical interventions are typically necessitated by urgent, life-threatening conditions and thus demand immediate attention and swift action. The process of managing such surgeries revolves around several key elements:
- Emergency triage protocols: Quick assessment and prioritization of patients based on the severity of their condition.
- Immediate surgical intervention: Often crucial in saving the patient’s life or preventing further harm.
- Trauma patient management: Involves the immediate and ongoing care for patients suffering from major physical injuries.
- Post-operative care: Critical in ensuring successful recovery and preventing complications.
Emergency surgical interventions are complex and multi-dimensional. The team’s ability to swiftly execute emergency triage protocols and adeptly manage trauma patients directly influences patient outcomes. Thus, understanding the essentials of emergency surgery is vital in the medical field.
Pre-Surgical Preparations: An Overview
Before a surgical procedure, thorough preparations are essential to ensure the safety and success of the operation, encompassing a wide array of tasks from medical evaluations to patient counseling. One of the most critical aspects is securing patient consent. An informed consent process is indispensable, allowing the patient to understand the procedure’s benefits, risks, and alternatives. The consent form should be detailed, clear, and understandable to the patient, ensuring their autonomy and respect for their decision-making.
Moreover, the importance of nutrition cannot be overlooked. Optimal nutritional status enhances wound healing, reduces hospital stay, and lowers postoperative complications. Evidence-based guidelines suggest a nutritional risk screening for all surgical patients, especially those undergoing major surgeries or having a medical condition that could impact their nutritional status. High protein intake, supplementation with specific nutrients like vitamins A and C, and zinc are often recommended.
Furthermore, preoperative assessments include evaluating the patient’s medical history, physical examination, laboratory tests, and imaging studies. These assessments help identify potential risks and optimize the patient’s health status prior to surgery. Lastly, patient education and counseling about the surgery, possible complications, and postoperative care are vital for patient preparation. These measures collectively contribute to the successful outcome of surgical interventions.
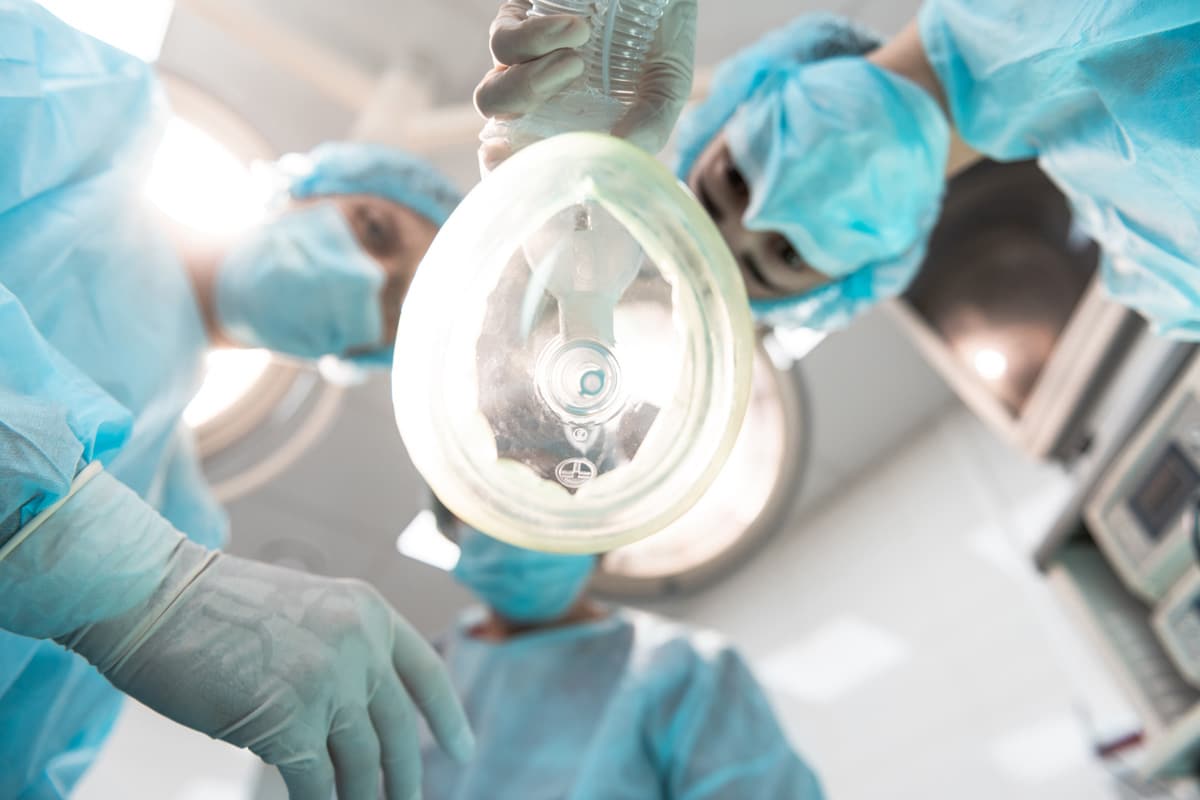
The Role of Anesthesia
Anesthesia, a critical component in surgical interventions, aids in the suppression of pain and other sensations. It exists in various forms, each with specific applications and potential risks, which are essential to understand for both physicians and patients. The forthcoming discussion will provide a detailed, evidence-based analysis of the types and uses of anesthesia, and an assessment of the associated risks.
Anesthesia Types and Uses
The surgeon’s toolkit would be incomplete without the crucial component of anesthesia, a medical innovation that has multiple types and uses, each playing a pivotal role in ensuring patient comfort and surgical success.
Anesthesia, which is derived from the Greek words meaning “loss of sensation,” can be broadly categorized into:
- General Anesthesia: This involves the entire body and causes the patient to lose consciousness.
- Regional Anesthesia: This type is used to numb only the area of the body that requires surgery.
- Local Anesthesia: This is used for smaller areas where surgery or a procedure is being done.
- Sedation: This type reduces patient anxiety and creates a state of calm or sleepiness.
The careful selection and use of these types, along with anesthesia alternatives, are integral to effective pain management post anesthesia.
Risks Associated With Anesthesia
While anesthesia plays a key role in facilitating surgical procedures by managing pain and anxiety, it is critical to consider the potential risks associated with its use. Studies show that anesthesia allergies, although rare, can lead to severe reactions including anaphylaxis. Symptoms may range from hives and difficulty breathing to a drop in blood pressure. Patients with a history of allergies should discuss potential risks with their anesthesiologist prior to surgery. On the other hand, sedation alternatives such as regional or local anesthesia can minimize these risks, but they also carry their own set of complications like nerve damage or infection. Therefore, the choice of anesthesia should be tailored to the patient’s health status, the surgical procedure, and the risk-benefit trade-off.
Key Surgical Techniques and Tools
In the realm of surgical practice, there are numerous key techniques and tools that have been developed and refined over time, each with its own unique contribution to the success and efficiency of surgical procedures. Intricately linked to the principles of surgical ethics, these techniques and tools are designed to maximize wound healing and patient recovery.
Delving into the specifics, these are some of the essential techniques and tools:
- Suturing Techniques: Used to close wounds, suturing techniques vary based on the type and location of the wound. The choice of technique can significantly impact wound healing.
- Surgical Scalpels and Blades: These tools have evolved over centuries, with modern versions offering higher precision and less tissue damage.
- Electrosurgical Devices: These allow for cutting, coagulation, and desiccation, minimizing blood loss during surgery.
- Laparoscopic Tools: Minimally invasive surgery is made possible through the use of laparoscopic tools, leading to quicker recovery times and less post-operative pain.
Analytical research has shown that a surgeon’s mastery of these techniques and tools, combined with a robust understanding of surgical ethics, directly influences the efficacy of wound healing and overall patient outcomes.
Post-Operative Recovery Process
Having extensively explored the various surgical techniques and tools, it is equally important to consider the post-operative recovery process, a critical phase that greatly determines the overall success of any surgical intervention. This phase is complex, multifaceted, and necessitates the employment of evidence-based strategies to optimize patient outcomes.
Central to this is the use of effective pain management strategies. Analgesic regimens, including pharmacological and non-pharmacological approaches, are tailored to individual patient needs and can significantly reduce post-operative pain, facilitating the recovery process. Studies suggest that optimizing pain control can enhance patient mobility, decrease hospital stay, and ultimately, reduce healthcare costs.
Equally integral are rehabilitation programs. These are designed to restore function, improve quality of life, and minimize disability following surgery. Rehabilitation may include physical therapy, occupational therapy, and patient education. Each program is individualized, considering the patient’s health status, type of surgery, and recovery goals. Evidence suggests that early initiation of rehabilitation programs post-surgery can expedite recovery, prevent complications, and improve long-term outcomes.
Therefore, the post-operative recovery process, underpinned by pain management strategies and rehabilitation programs, plays a pivotal role in the success of surgical interventions.
Risks and Complications in Surgeries
Despite the meticulous planning and execution of surgical procedures, the potential for risks and complications remains, ranging from minor post-operative infections to severe life-threatening events.
Adherence to surgery ethics is crucial to mitigate these risks. However, even with the strictest adherence, unforeseen complications may occur. These complications can be stratified into four major categories:
- Intraoperative Complications: These may include accidental damage to surrounding tissues or organs, anesthetic complications, or excessive bleeding.
- Immediate Postoperative Complications: This includes infections, postoperative bleeding, or reactions to anesthesia.
- Delayed Postoperative Complications: These may include wound dehiscence, deep vein thrombosis, or pulmonary embolism.
- Long-Term Complications: This encompasses complications that affect the patient’s overall health and quality of life, such as chronic pain or organ dysfunction.
Effective post-surgery rehabilitation is crucial in managing these complications. It aims to restore function, improve quality of life, and prevent long-term disability. It should be noted that the occurrence of these complications is not always reflective of the surgeon’s competence, but more often due to the patient’s individual health condition and response to surgery. The key is to anticipate, prevent where possible, and manage these complications effectively when they arise.
Breakthroughs in Minimally Invasive Surgery
Recent years have seen remarkable advancements in the field of minimally invasive surgery, largely driven by technological innovations and enhanced surgical techniques. One such notable development is the advent of telemedicine surgeries. This method enables surgeons to perform procedures remotely using advanced communication technologies and robotic interfaces. Studies indicate a considerable reduction in post-surgical complications and recovery times with telemedicine surgeries, underscoring their potential in improving patient outcomes.
Laser-assisted procedures represent another significant leap in this domain. These procedures employ highly focused light beams to make precise incisions, thereby minimizing tissue damage. Furthermore, laser technologies facilitate increased control over depth and extent of the surgical field, reducing intraoperative risks. A systematic review by Kallam et al., 2019, revealed a lower rate of surgical site infections and shorter hospital stays in patients undergoing laser-assisted surgeries, exemplifying its effectiveness.
These breakthroughs in minimally invasive surgery not only enhance surgical precision but also promise improved patient safety. However, widespread adoption requires addressing challenges such as high setup costs and the need for specialized training. Despite these hurdles, the advancements in minimally invasive surgery serve as a testament to the ongoing evolution of surgical interventions.

The Impact of Robotics in Surgery
Undeniably, the advent of robotics has revolutionized surgical practices by providing unparalleled precision, increased control, and the capacity to execute complex procedures with minimal invasiveness. The impact of robotics is evident in various facets of surgical practices, particularly in terms of robotic precision and training surgeons.
- Robotic precision: Robots offer exceptional accuracy, reducing the risk of human error. Surgeons can perform intricate operations with more exactitude and less physical strain.
- Training Surgeons: Robotic platforms facilitate advanced training opportunities for surgeons, enabling them to master new techniques in a controlled environment.
- Minimally invasive procedures: Robotic systems enable surgeons to perform complex surgeries through small incisions, reducing patient trauma and recovery time.
- Improved patient outcomes: The precision of robotic systems often results in fewer complications, decreased blood loss, and shorter hospital stays for patients.
Research supports these benefits, with a meta-analysis of 50 studies finding that robotic surgery resulted in fewer complications and shorter hospital stays than traditional surgery (Liao et al., 2019). However, the high cost and extensive training required for robotic surgery are significant challenges that need to be addressed. Despite these hurdles, the impact of robotics in surgery is substantial, promising a future of improved surgical outcomes and patient care.
Future Trends in Surgical Interventions
Looking ahead, emerging technologies and innovations are poised to further transform the landscape of surgical interventions, potentially leading to more efficient, precise, and minimally invasive procedures. One such advancement is telemedicine surgery, a practice that leverages digital platforms to perform surgical procedures remotely. This could drastically reduce geographical barriers to surgical care, enabling patients in remote areas to access high-quality surgical care without the need for physical proximity with the surgeon.
Moreover, the integration of augmented reality (AR) applications into surgical procedures is another promising trend. AR could enable surgeons to overlay digital information onto the physical world, providing real-time visual guidance during operations. This could result in enhanced precision, reduced surgical times, and potentially improved patient outcomes.
However, these advancements also pose challenges. For telemedicine surgery, issues like latency and the need for reliable, high-speed internet connectivity are significant hurdles. Likewise, for AR, potential concerns include the accuracy of overlaid information and the need for user-friendly interfaces. Nevertheless, with ongoing research and technological development, these future trends could revolutionize surgical interventions, enhancing their efficiency, precision, and accessibility.
Case Studies: Successful Surgical Interventions
In order to illustrate the remarkable progress and effectiveness of surgical interventions, it is instructive to examine a few case studies that highlight the successful application of these methods in different contexts.
- Case 1: A 50-year-old male patient underwent a minimally invasive cardiac bypass surgery. Patient experiences showed improved quality of life post-surgery, with a significant reduction in chest pain. Additionally, the surgical costs were less compared to traditional open-heart surgery due to shorter hospital stay and fewer complications.
- Case 2: A female patient with early-stage breast cancer opted for a lumpectomy followed by radiation, instead of a mastectomy. Her patient experience was positive, highlighting the preservation of her breast and a quicker recovery.
- Case 3: Laparoscopic gallbladder removal in a 60-year-old patient resulted in lower surgical costs and a quicker return to normal activities compared to open surgery.
- Case 4: Minimally invasive spine surgery was performed on a patient suffering from chronic lower back pain. The patient’s experience was favorable, with significant pain reduction and a quicker return to work.
These cases underscore the potential of surgical interventions in improving patient outcomes, reducing recovery time, and managing the overall costs of surgery.
Frequently Asked Questions
What Are the Emotional and Psychological Impacts of Undergoing a Surgical Intervention?
Undergoing any major life-altering event can lead to significant emotional and psychological impacts. These may include anxiety, stress, and fear, which can be mitigated through emotional preparation and addressing underlying fears effectively.
How Can a Patient Manage Post-Surgical Pain at Home?
Post-surgical pain management at home involves a combination of prescribed pain medication management and non-drug remedies, such as physical therapy and mindfulness techniques, tailored to the individual’s specific needs and tolerance levels.
What Role Does Diet and Nutrition Play in the Recovery Process After a Surgical Intervention?
Diet and nutrition play a pivotal role in recovery, influencing wound healing and overall health. Consuming nutritional supplements can replenish essential elements, expedite tissue repair, and bolster the immune system to prevent postoperative complications.
Are There Any Specific Exercises or Physical Therapies Recommended for Patients After a Surgical Procedure?
Specific exercises and physical therapies are often recommended to enhance recovery, minimize complications, and manage scars. The duration of this rehabilitation phase depends on the individual’s overall health and the nature of the procedure undertaken.
How Does a Patient’s Age and Overall Health Condition Influence the Success of a Surgical Intervention?
A patient’s age and health status significantly influence the success of medical treatments due to factors like anesthesia effects and surgical risks. Elderly or unhealthy individuals may face increased complications and recovery times.