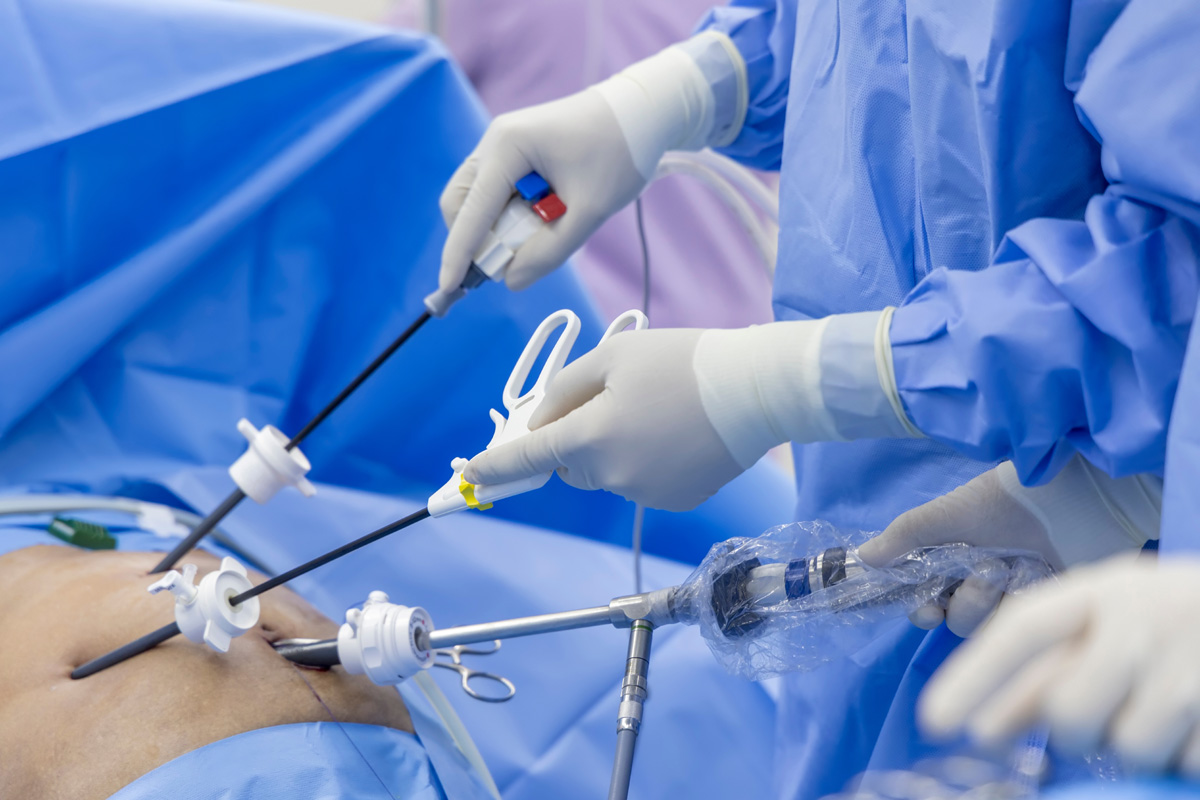
Endoscopic spine surgery, a minimally invasive procedure, has been gaining attention in the medical field owing to its reported success rate of 80% to 90%. These compelling statistics, however, are influenced by a myriad of factors such as the surgeon’s skill, patient’s health condition, the specific spinal disorder, and the progression of surgical equipment. Although these initial figures may seem important, it’s vital to examine the intricate dynamics that contribute to the success of this surgical intervention.
Understanding Endoscopic Spine Surgery
Exploring the domain of endoscopic spine surgery, it is essential to comprehend that this procedure is a minimally invasive surgical technique employed to treat spinal conditions which otherwise would necessitate open surgery. The procedure’s success rate is largely influenced by the surgeon’s qualifications and a deep understanding of spine anatomy basics.
The spine, a complex structure made up of vertebrae, intervertebral discs, and the spinal cord, requires a high degree of precision in surgical interventions. The surgeon’s knowledge of spine anatomy basics is critical in ensuring the success of endoscopic spine surgery, minimizing the risk of damage to surrounding tissues and maximizing patient recovery.
In terms of surgeon qualifications, a profound knowledge in neurosurgery or orthopedics, combined with specialized training in endoscopic techniques, is essential. The surgeon’s skill set, experience, and competence directly impact the success rate of the procedure. Additionally, a surgeon’s ability to interpret diagnostic imaging, understand pathological variations, and execute meticulous surgical planning contributes to the overall effectiveness of endoscopic spine surgery.
Procedure of Endoscopic Spine Surgery
The actual procedure of endoscopic spine surgery involves a detailed and meticulous process, necessitating careful execution of each step to guarantee a successful outcome. The surgical instruments used and the role of anesthesia are pivotal elements in this procedure.
- Preparation: Prior to the surgery, the patient is prepped and positioned in a way that facilitates ideal access to the surgical site. The role of anesthesia is essential at this stage, ensuring the patient is pain-free and comfortable throughout.
- Incision & Insertion: A small incision is made and the endoscope is carefully inserted. Advanced surgical instruments are used, including a high-definition camera and light source, providing a clear view of the spine.
- Disc Removal or Decompression: Utilizing specialized surgical instruments, the surgeon removes the damaged disc or decompresses the nerve, relieving pressure.
- Closure: The endoscope is removed, and the incision is closed using sutures or surgical staples.
An endoscopic spine surgery is less invasive compared to traditional spine surgery, reducing recovery time and potential risks. However, it’s a complex procedure requiring a high level of expertise, precision and selection of appropriate surgical instruments to ensure a successful outcome.
Success Rate Statistics
In evaluating the performance of endoscopic spine surgery, it is essential to rigorously examine the success rate statistics. These statistics, which represent the percentage of successful procedures, provide a quantitative measure of the efficacy of this surgical approach. Additionally, understanding the factors influencing these outcomes allows for a more thorough grasp of the circumstances under which endoscopic spine surgery is most effective.
Analyzing Success Percentages
An in-depth analysis of success rate statistics reveals important insights into the effectiveness of endoscopic spine surgery. Vital factors such as spine health maintenance and pre-surgery preparations contribute substantially to these figures.
- Thorough spine health maintenance reduces the risk of complications, resulting in a higher success rate.
- Pre-surgery preparations, including patient education and physical readiness, greatly influence the outcome.
- An average success rate of 80%-90% reported in recent studies underscores the efficacy of this procedure.
- A closer look at the statistics reveals a higher success rate in patients with localized spinal conditions, compared to those with multiple issues.
These findings affirm the critical role of comprehensive patient care in enhancing the success rates of endoscopic spine surgeries.
Factors Influencing Outcomes
Building upon the previously discussed success rates, it is important to elucidate the specific factors that play a crucial role in shaping the outcomes of endoscopic spine surgeries. Primarily, the surgeon’s expertise heavily influences the success rate. A highly skilled and experienced surgeon can adeptly navigate the complexities of the spine, minimizing potential risks. Conversely, a less experienced surgeon may encounter difficulties, potentially impacting the success rate negatively. The patient’s lifestyle also plays a pivotal role. For instance, those who maintain an active, healthy lifestyle generally recover faster post-surgery. Additionally, patients who avoid smoking or excessive alcohol consumption significantly increase their chances of successful recovery. As a result, a combination of surgeon’s expertise and patient’s lifestyle greatly influences the outcome of endoscopic spine surgeries.
Factors Influencing Success Rates
Various elements play a pivotal role in the success rate of endoscopic spine surgery, including the patient’s overall health, the surgeon’s experience and skill, as well as the specific nature of the spinal condition being treated. The role of Surgical Equipment Advancements is also essential, as they provide the precision and efficiency required for this minimally invasive procedure. Moreover, Patient Lifestyle Impact, like smoking or physical activity levels, can influence the healing process post-surgery.
The success rate can be significantly influenced by:
- The Surgeon’s Expertise: A surgeon’s skill and familiarity with endoscopic techniques can greatly affect the outcome.
- Patient Health: Patients with good overall health and a disciplined lifestyle generally have better recovery rates.
- Spinal Condition: The specific nature of the spinal issue can also dictate the success rate. Some conditions may be more amenable to endoscopic surgery than others.
- Technological Advancements: The ongoing development of surgical technology results in improved accuracy and less invasive procedures, which can enhance the success rate.
Comparing Traditional and Endoscopic Surgery
A thorough analysis of traditional and endoscopic spine surgery accentuates their fundamental procedure differences, recovery periods, and associated risks. These surgical methods, while sharing a common goal of mitigating spinal issues, utilize distinctively different techniques and yield varying postoperative outcomes. It is essential to scrutinize these aspects in order to gain a detailed understanding of their success rates.
Procedure Differences
In evaluating the differences between traditional and endoscopic spine surgery, one must consider several critical aspects such as surgical approach, invasiveness, recovery time, and potential complications. Understanding the spine anatomy basics is key.
- Surgical Approach: Traditional open surgery involves a larger incision to expose the anatomy, whereas endoscopic surgery uses smaller incisions and a camera to navigate.
- Invasiveness: Traditional surgery is more invasive, often requiring muscle dissection, while endoscopic surgery is less so.
- Recovery Time: Endoscopic surgery typically results in faster recovery times due to its minimally invasive nature.
- Patient Eligibility Criteria: Patients with certain medical conditions may not be eligible for endoscopic surgery, whereas traditional surgery may be more broadly applicable.
Each procedure has its own pros and cons which must be weighed carefully.
Recovery and Risks
While the surgical approach, invasiveness, and patient eligibility are important considerations, the recovery process and potential risks associated with traditional and endoscopic spine surgery also have significant implications for patient outcomes. With traditional spine surgery, recovery can be lengthy and pain management strategies often include potent medications. Conversely, endoscopic procedures typically involve shorter recovery periods and less reliance on narcotics for pain control. Post surgery lifestyle changes, such as physical therapy, are usually necessary for both, but the intensity and duration can differ. Risks, such as infection or nerve damage, are inherent to any surgical procedure. However, the minimally invasive nature of endoscopic surgery can potentially reduce these risks, thereby further enhancing patient outcomes.
Benefits of Minimally Invasive Surgery
Minimally invasive surgery, specifically endoscopic spine surgery, offers numerous advantages, including reduced trauma to surrounding tissues, lower infection rates, and expedited recovery times. This underscores the surgical advancements made in recent years, which aim to maximize patient comfort and post-operative outcomes.
Let’s categorize these benefits into four main points:
- Reduced Trauma: By using small incisions and specialized instruments, endoscopic spine surgery minimizes damage to the surrounding tissues. This results in less post-operative pain and a quicker return to normal activities.
- Lower Infection Rates: The minimal exposure of the surgical site to external environment reduces the risk of post-operative infections, enhancing the overall safety of the procedure.
- Expedited Recovery: The decreased trauma and lower infection rates collectively contribute to a faster recovery period. This allows patients to resume their daily activities sooner than traditional surgery methods.
- Increased Patient Comfort: The combination of less invasive techniques, lower infection rates, and quicker recoveries notably enhances the patient’s comfort during the post-operative period.
These points underline the importance of minimally invasive methods in modern spine surgery, showcasing the balance between effective treatment and patient wellbeing.
Risks and Complications
While endoscopic spine surgery is generally successful, it does not come without potential risks and complications. It is important to understand and discuss these possible issues, such as common post-operative complications, to make informed decisions regarding treatment. Additionally, strategies for mitigating these surgical risks will be explored to guarantee the highest degree of patient safety and maximize surgical success rates.
Common Post-Operative Complications
Despite the high success rate of endoscopic spine surgery, it is important to take into account the potential post-operative complications, which can range from minor issues such as temporary numbness to more severe complications like infection or nerve damage. Robust complication management and infection prevention protocols are key to reducing these risks.
- Temporary numbness or weakness: This can occur due to nerve manipulation, usually resolving over time.
- Infection: Despite stringent infection prevention measures, surgical site infections can occur, requiring antibiotic treatment or additional surgery.
- Nerve damage: This rare but serious complication can result in chronic pain or paralysis.
- Dural tear: An unintentional tear in the dural membrane can lead to cerebrospinal fluid leakage, causing headaches or infection.
Mitigating Surgical Risks
In order to mitigate the risks and complications associated with endoscopic spine surgery, stringent operative strategies and robust preoperative planning are essential. Risk management plays an important role in this process, as it involves careful patient evaluation, selection, and preparation. These steps help to identify any potential medical conditions that may increase the risk of complications during or after surgery. Surgical innovations have also immensely contributed to reducing surgical risks. Evolving techniques like minimally invasive endoscopic procedures, which cause less trauma to surrounding tissues compared to traditional open surgery, have led to improved surgical outcomes. Therefore, through meticulous risk management and embracing surgical innovations, it is possible to reduce surgical risks associated with endoscopic spine surgery.

Post-Surgery Expectations
After undergoing endoscopic spine surgery, patients can typically anticipate a range of specific outcomes based on a multitude of factors including their overall health, the nature of their spine condition, and the specifics of their surgical procedure.
- Pain Management: Post-operative pain is expected but is generally manageable with prescribed medication. The intensity of discomfort generally diminishes within a few days, and most patients can shift to over-the-counter pain relievers within a week.
- Lifestyle Modifications: Patients are advised to gradually reintroduce physical activities into their daily routine. This can include light walking and limited household chores. A rehabilitation plan might also be recommended, involving physiotherapy or targeted exercises to strengthen the back.
- Healing and Recovery: The healing process varies from person to person but patients should expect progressive improvement over weeks or months. Regular follow-up appointments are necessary to monitor recovery and manage any potential complications.
- Long-Term Expectations: The ultimate goal of endoscopic spine surgery is to alleviate pain and improve functionality. Most patients experience significant relief and an improved quality of life, although the exact degree of improvement is dependent on the specific condition and the patient’s overall health.
Patient Testimonials and Experiences
Drawing on the first-hand experiences of patients who have undergone endoscopic spine surgery provides invaluable insights into the real-world outcomes and individual perceptions of the procedure’s efficacy. The compilation of these testimonials has allowed for a thorough analysis of patient satisfaction and surgery affordability.
The analytical review of patient testimonials consistently indicates a high level of satisfaction post-operation. This satisfaction stems from greatly reduced pain levels and enhanced mobility, thereby improving overall quality of life. Moreover, the minimally invasive nature of the procedure reduces the risk of complications, enhancing patient confidence and satisfaction in the surgical outcome.
In terms of affordability, the advanced endoscopic technique often results in shorter hospital stays and quicker recovery times compared to traditional open surgery. This translates to reduced medical costs and less time off work, making the surgery more cost-effective for many patients.
However, it is important to note that individual experiences vary and are influenced by numerous factors, such as overall health, age, and the specific spinal condition treated. Hence, while patient testimonials provide critical insights, they should be considered as part of a broader analysis of endoscopic spine surgery’s success rate.
Recovery and Rehabilitation Process
The process of recovery and rehabilitation following endoscopic spine surgery is an essential component of evaluating the procedure’s overall success and patient satisfaction rates. This period allows for a thorough assessment of pain management techniques’ effectiveness and the endurance of rehabilitation exercises.
The recovery and rehabilitation process can be categorized into four important stages:
1. Immediate Post-Operative Phase: This phase mainly focuses on pain management techniques, including medication and non-pharmaceutical strategies, to guarantee patient comfort.
2. Early Rehabilitation: Once the immediate post-operative pain is managed, a series of rehabilitation exercises are introduced to promote mobility and flexibility.
3. Mid Rehabilitation: The patient continues with the exercises, progressively increasing intensity and complexity to strengthen the spine and surrounding muscles.
4. Long-Term Rehabilitation: This phase emphasizes the maintenance of exercise routines to prevent future spine-related complications.
Each stage is underpinned by a dual focus on pain management techniques and rehabilitation exercises, designed to expedite recovery and facilitate a return to everyday activities. It’s important to note that the timeline and progression through these stages may vary, contingent on individual factors like the patient’s overall health status and the complexity of the surgery performed.
Making the Right Choice
While evaluating the recovery and rehabilitation stages is a crucial part of the endoscopic spine surgery process, another significant consideration is making the informed decision to proceed with the surgery itself. This necessitates a thorough exploration of surgical options and an understanding of the potential risks and benefits.
Surgical options exploration is a intricate process that involves evaluating the patient’s medical history, current health status, and the severity of the spine condition. Detailed imaging studies, such as MRI, CT, or X-ray, are typically used to provide a detailed view of the spine’s anatomy. This data aids surgeons in determining the most suitable surgical approach and allows patients to fully grasp the procedure.
Informed decision-making is a collaborative process involving the patient, surgeon, and sometimes the patient’s family. It requires a detailed discussion of the potential risks, benefits, and alternative treatment options. The patient should be given ample time to reflect on the information, ask questions, and, if needed, seek a second opinion.
This detailed, scientific approach guarantees that the decision to proceed with endoscopic spine surgery is not taken lightly, but is instead an informed choice based on thorough analysis and understanding.
Frequently Asked Questions
Are There Any Conditions That Would Disqualify Me From Endoscopic Spine Surgery?
Certain conditions may disqualify a patient from endoscopic spine surgery. Preoperative evaluation is essential to assess suitability. Factors such as severe obesity, significant spinal instability, or large herniated discs may suggest spine surgery alternatives.
Does Insurance Typically Cover Endoscopic Spine Surgery?
Insurance coverage for endoscopic spine surgery often relies on individual policies, with varying insurance limitations and coverage discrepancies. Consultation with your insurance provider is crucial to understand the extent of your coverage.
What Are the Qualifications for a Surgeon to Perform Endoscopic Spine Surgery?
To perform endoscopic spine surgery, surgeons require extensive training through specific Surgeon Training Programs. Additionally, they must possess specialized equipment knowledge, ensuring proficiency in the latest endoscopic surgical techniques and tools.
Are There Any Lifestyle Changes Recommended Prior to Undergoing Endoscopic Spine Surgery?
Prior to endoscopic spine surgery, certain lifestyle changes are often recommended. These include diet modifications for best nutrition and an exercise regimen to strengthen the back muscles, both aimed at facilitating a successful recovery.
Can Endoscopic Spine Surgery Be Combined With Other Treatments or Procedures?
Yes, endoscopic spine surgery can be combined with other treatments or procedures such as post-surgery rehabilitation. Additionally, alternative treatment options can be integrated to potentially enhance recovery and improve long-term outcomes.