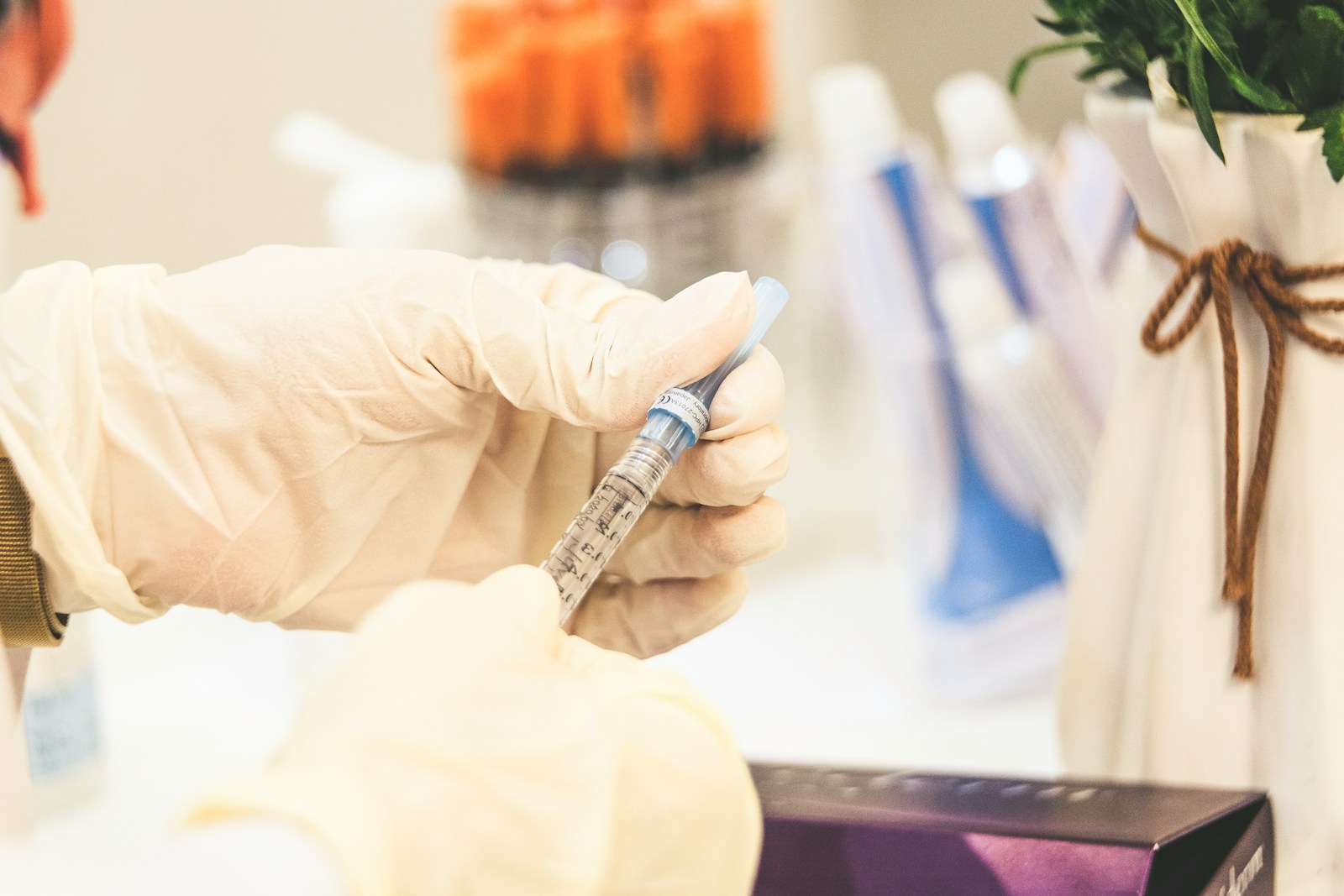
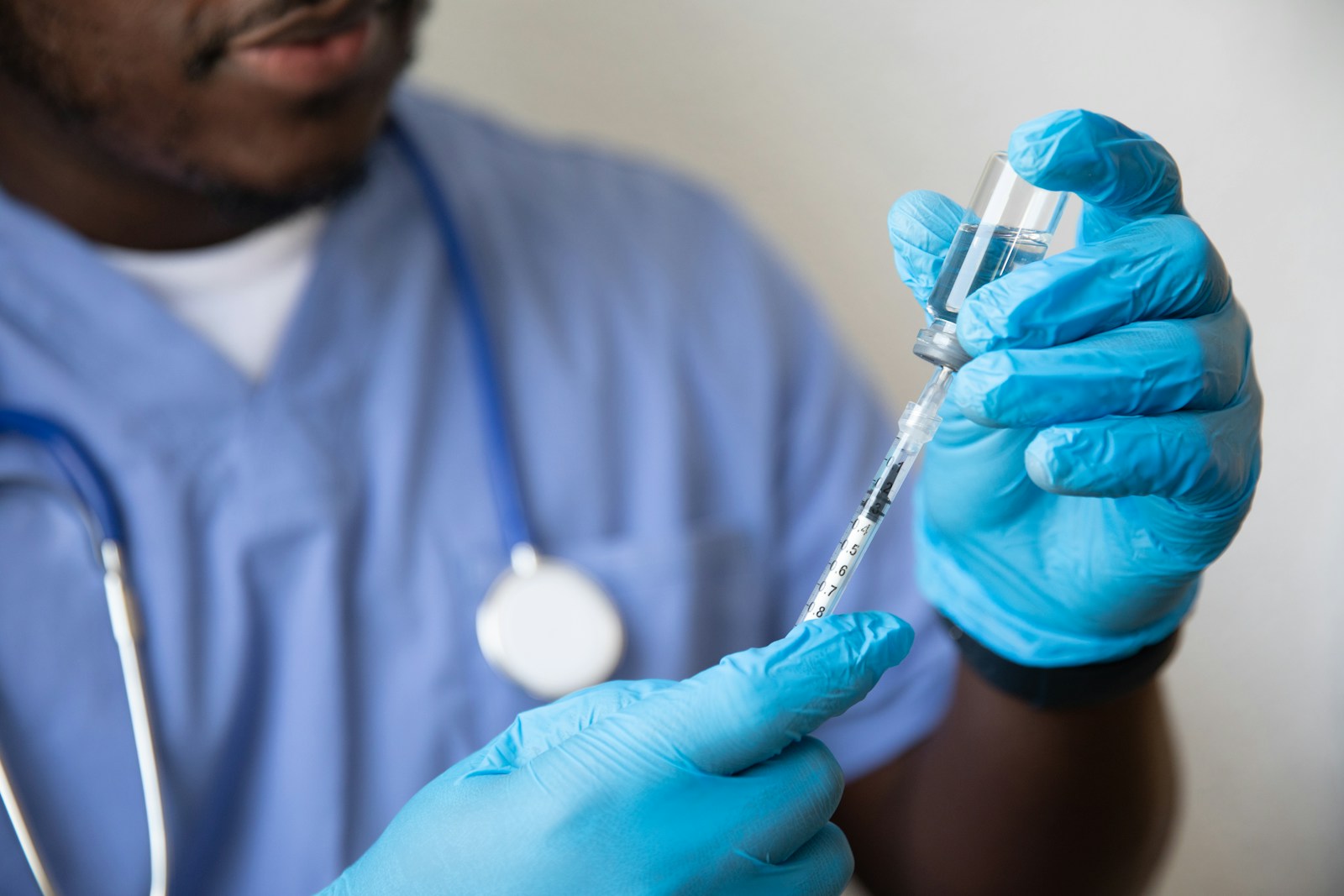
Epidural injections, a common method of pain management in various medical conditions, have become a topic of extensive discussion among healthcare professionals. While they are known for their potential to provide immediate relief and reduce the necessity for surgery, the procedure does not come without its share of controversies and risks. The question that arises is, how do the benefits weigh against the potential risks? This necessitates an in-depth understanding of epidural injections, their effectiveness, and the recovery process.
Understanding Epidural Injections
To understand the concept of epidural injections, one must explore the intricate details of this medical procedure, which involves the administration of drugs directly into the epidural space of the spine. This procedure is commonly used for pain management in various medical conditions such as labor, chronic back pain, and certain types of surgeries.
However, there are several epidural misconceptions that permeate public understanding. One common misconception is that epidural injections are inherently dangerous. While the procedure does carry risks, as does any medical intervention, it is generally considered important when conducted by a trained professional. Another misconception is that epidural injections always provide immediate and complete pain relief. The reality is that the efficacy of this procedure varies among individuals, and it may take time for the full effects to manifest.
Concerning the injection cost, it is essential to note that the price can vary significantly. Factors influencing the cost include the complexity of the procedure, the type and amount of medication used, the healthcare provider’s fees, and the geographical location. It is important for patients to discuss the potential costs with their healthcare providers to make an informed decision about their treatment options.
Anatomy of the Epidural Space
Exploring the anatomy of the epidural space, it is essential to note that this area, situated between the protective covering of the spinal cord and the vertebrae, serves as the targeted site for the administration of epidural injections. This space is filled with fat and small blood vessels, providing a cushioning effect for the delicate spinal cord.
Understanding epidural space functions is important to appreciate the role it plays in spinal cord protection. The epidural space acts as a protective barrier, shielding the spinal cord from any potential damage caused by the bony vertebrae. In addition, the epidural space also houses nerve roots that exit the spinal cord, further emphasizing its crucial role in maintaining spinal integrity.
The epidural space is not uniform in size throughout the vertebral column. It varies in dimension depending on the specific area of the spine, with the lumbar region typically having a larger epidural space than the cervical region. The variability in size can influence the distribution and effectiveness of epidural injections, underscoring the importance of a thorough understanding of the epidural space’s anatomy for effective pain management.
Types of Epidural Injections
Exploring the domain of epidural injections, it becomes evident that there are several different types, each specifically designed to target and alleviate pain in distinct regions of the spine. The types include lumbar, thoracic, and cervical epidural injections, tailored to the lower back, mid-spine, and neck regions respectively.
Lumbar epidural injections, often used for sciatica or low back pain, generally have a moderate epidural injection cost, considering their high efficacy in pain management. Thoracic epidural injections target the mid-spine area and are beneficial in treating pain related to spinal stenosis or disc herniation. The cervical epidural injections, while slightly more expensive, are essential for neck and arm pain, often resulting from conditions like cervical radiculopathy.
The injection duration depends on several factors, including the type of medication used, the severity of the patient’s pain, and the targeted region. Typically, the relief from an epidural injection can last from one week to one year. However, it’s important to note that the duration of relief varies among patients and the type of injection administered. The efficacy and duration of the pain relief, combined with the related costs, play an important role in determining the appropriate type of epidural injection for each patient.
The Procedure: Step-by-step Guide
The process of administering epidural injections involves a series of steps that demand professional expertise and precision. The first point of discussion will be a thorough understanding of the procedure itself, followed by the necessary preparations that must be undertaken prior to the procedure. Lastly, we will examine the crucial post-epidural care procedures to guarantee maximum recovery and effectiveness of the treatment.
Understanding the Epidural Procedure
Delving into the step-by-step process of an epidural injection procedure can provide valuable insights into its intricacies and technicalities. As a prominent tool in the array of pain management alternatives, the procedure begins with the patient lying face down. Following local anesthesia, a needle is guided into the epidural space in the spine using fluoroscopic guidance. A contrast dye confirms the correct placement of the needle, after which the epidural medication is administered.
It’s essential to debunk prevalent epidural injection myths, such as the misconception of immediate pain relief. The full effects of the injection can take up to a week to manifest. The procedure’s complexity underscores the importance of seeking treatment from experienced medical professionals.
Pre-Procedure Preparations
Before undergoing the epidural injection procedure, there are several preparatory steps to be taken, designed to guarantee the efficacy and safety of the treatment. Patient Eligibility is determined by thorough medical examination to identify contraindications such as infection, bleeding disorders or allergies to medication used. Patients are also advised to disclose any medication they are currently taken, as some may interfere with the efficacy of the procedure. Fasting Guidelines are also provided, with patients typically required to fast for six to eight hours prior to the procedure to avoid complications during sedation. Pre-procedure preparation also involves arranging for a responsible adult to drive the patient home post-procedure, given the temporary mobility limitations that follow.
Post-Epidural Care Steps
Following the completion of the epidural injection procedure, a specific set of post-operative care steps must be followed to guarantee the best possible recovery and the success of the treatment.
- Pain Management Techniques: Post-operative pain can be expected after the procedure. Patients should be equipped with the appropriate pain management techniques which may include medications, rest and certain physical activities.
- Emotional Support Post Epidural: Emotional support is vital in the healing process. Patients may experience anxiety or depression post-procedure. It’s important to have a support system in place, including healthcare professionals, family, or friends.
- Follow-up Appointments: Regular follow-ups with the healthcare provider are necessary to monitor the patient’s progress and to make any necessary adjustments to the treatment plan.
Uses of Epidural Injections
Commonly used in pain management, epidural injections serve a multitude of purposes in both medical and surgical settings. These injections are frequently utilized for the relief of lower back pain, labor pain, and chronic pain conditions such as sciatica and herniated discs. They deliver steroids or anesthetics directly into the epidural space of the spine, providing immediate and often long-lasting relief.
Epidural injections, however, are not devoid of controversies. Some medical professionals argue about their effectiveness and the appropriateness of their use, specifically for non-surgical pain management. Critics cite the lack of substantial evidence to support their long-term benefits and raise concerns about potential overuse.
Insurance coverage issues add another layer of complexity to the use of epidural injections. The cost of these procedures can be significant, and not all insurance policies cover them. This can create financial burdens for patients seeking this form of pain relief. It is essential for healthcare providers to discuss these issues with patients, ensuring they are fully informed about the potential costs and benefits associated with epidural injections, before proceeding with this treatment option.
Potential Risks and Complications
While epidural injections are a frequently utilized therapeutic approach, they are not without potential risks and complications. It is important to thoroughly understand the possible side effects that may arise post-procedure. A detailed analysis of preventive measures in mitigating injection-related complications will also be discussed in this section.
Understanding Epidural Side Effects
In the domain of anesthetic procedures, epidural injections, despite their widespread use and efficacy, carry a certain degree of potential risks and complications that must be thoroughly understood. Differing from general anesthesia, epidurals specifically target the spinal area, which can lead to unique complications.
- Epidural vs. General Anesthesia: Epidurals are localized, unlike general anesthesia which affects the whole body. This difference can result in complications such as nerve damage, dural puncture, and headaches.
- Epidural Impact on Labor: In childbirth, epidurals can occasionally lead to longer labor durations, and in rare cases, necessitate instrumental delivery.
- Potential Risks: Allergic reactions to the anesthetic, low blood pressure, and temporary loss of bladder control are potential side effects.
Understanding these risks allows patients to make informed decisions about their anesthetic options.
Preventing Injection Complications
Given the potential risks associated with epidural injections, it is imperative to discuss preventative measures that can minimize the occurrence of complications. Adequate Epidural Training is vital in preventing complications. The provider must be well-versed in the technique, anatomy, and potential pitfalls of the procedure.
Furthermore, the use of high-quality Injection Equipment can contribute to reducing risks. The equipment should be reliable, sterile, and specifically designed for performing epidurals. The use of ultrasound guidance can improve the accuracy of needle placement, further reducing potential complications.
In addition, a thorough patient evaluation is essential to identify any contraindications or risks specific to the individual. Finally, proper post-procedure care and patient education can help prevent complications, such as infection or prolonged pain post-procedure.
Benefits of Epidural Injections
Epidural injections, often utilized for pain management, offer a range of significant benefits, especially when it comes to reducing inflammation and alleviating acute or chronic discomfort. These injections are a non-surgical treatment option that can provide relief for a wide range of conditions such as spinal stenosis, herniated discs, and sciatica. Understanding the benefits of this procedure can help patients make informed decisions regarding their healthcare.
- Rapid Pain Relief: Epidural injections deliver medication directly into the epidural space, which surrounds the spinal cord. This direct delivery can result in immediate relief from pain and discomfort.
- Reduced Need for Surgery: For some patients, epidural injections can provide sufficient pain relief to avoid or delay the need for spinal surgery. This can lead to significant savings in terms of ‘Epidural Injection Costs, Insurance Coverage’.
- Improved Quality of Life: By managing pain effectively, epidural injections can assist patients in resuming daily activities, thereby improving their overall quality of life.
Effectiveness: What Research Says
When evaluating the effectiveness of epidural injections, numerous research studies have provided valuable insights. However, it’s essential to take into account the research limitations. For instance, most studies are based on patient self-reporting, which can be subjective, and the control groups used in clinical trials may not perfectly match the broader patient population.
Furthermore, studies often focus on short-term pain relief, leaving a knowledge gap about long-term effects and potential complications. Another limitation is the heterogeneity of treatment protocols across studies, making it challenging to compare results and draw robust conclusions.
Despite these limitations, the overall body of research suggests that epidural injections can offer significant pain relief for a variety of conditions, including sciatica, spinal stenosis, and herniated discs. This relief can improve patients’ quality of life and enable them to resume normal activities.
It’s also important to take into account injection costs. Epidural injections are more expensive than some alternative treatments, but they can be cost-effective when they reduce the need for other interventions or surgery. However, cost-effectiveness depends on individual patient factors, such as the severity and duration of pain, the patient’s overall health status, and the specific treatment protocol used.

Preparing for an Epidural Injection
Before undergoing an epidural injection procedure, a thorough preparation process is essential to guarantee maximum pain relief and minimize potential complications. Understanding these steps can help to mitigate common issues such as injection anxiety and financial considerations.
The preparation for an epidural injection involves:
- Medical assessment: This includes a complete review of your medical history, current medications, allergies, and any previous reactions to anesthesia. Important tests, such as blood tests or imaging studies, may be required to assess your overall health and pinpoint the exact area for the injection.
- Managing Injection Anxiety: It’s common to experience anxiety before the procedure. The healthcare team will provide resources and techniques to manage this, such as relaxation exercises, guided imagery, or in some cases, mild sedation.
- Financial Planning: Prior to the procedure, you should understand the costs involved, which can help alleviate financial stress. This includes knowing what your insurance covers, the out-of-pocket expenses, and discussing payment plans if necessary.
Preparation plays a significant role in the success of an epidural injection. By understanding what to expect and taking steps to prepare, you can increase the chances of a successful outcome, reduce anxiety, and manage financial considerations effectively.
Recovery and Aftercare
Following the administration of an epidural injection, a patient’s care and recovery process is crucial to guarantee excellent results and mitigate potential complications. This section will examine essential elements of post-injection home care, and strategies to manage potential side effects. We will explore the time frame for recovery, the importance of rest, recognition of adverse reactions, and when to seek professional medical intervention.
Post-Injection Home Care
The period after receiving an epidural injection requires careful home care to guarantee excellent recovery and efficient pain management. This phase is vital as it can greatly contribute to the success of the treatment. It will often involve pain management strategies and certain lifestyle modifications post injection.
Here are three key steps to follow:
- Pain Management: Implement strategies such as over-the-counter pain medication, heat or cold therapy, and rest. The goal is to alleviate discomfort while the body heals.
- Activity Modification: Gradually resume activities. Avoid heavy lifting or strenuous exercise. It’s crucial to balance rest and movement to prevent stiffness and promote healing.
- Follow-Up: Attend all scheduled follow-up appointments. Your healthcare provider will monitor your progress, adjust pain management as necessary, and provide personalized advice.
Managing Potential Side-Effects
While adhering to post-injection home care instructions aids in a successful recovery, it is equally important to understand and manage potential side-effects that may arise during the recovery and aftercare period. These side-effects may vary in duration and frequency. Side effects duration typically ranges from a few hours to several days, with most subsiding within a week. Side effects frequency depends on various factors including the patient’s overall health, type of medication used, and individual response to the injection. Common side effects include localized pain, headaches, and minor bleeding. If these persist beyond the usual duration or occur at a high frequency, medical attention should be sought immediately. Management includes rest, over-the-counter pain medication, and frequent monitoring.
Alternative Treatments to Consider
Numerous alternative treatments, ranging from physical therapy to acupuncture, can be considered if epidural injections are not suitable or effective for pain management. These non-pharmaceutical alternatives are often preferred by patients due to their vital nature and thorough understanding of their medical conditions.
- Physical Therapy: This involves exercises and movements designed to improve mobility and strength, and alleviate pain. Techniques such as heat and cold therapy, massage, and electrical stimulation may also be incorporated.
- Acupuncture: Originating from traditional Chinese medicine, acupuncture involves inserting thin needles at specific points on the body to stimulate nerves, muscles, and connective tissue. This is believed to increase blood flow and trigger the body’s natural painkillers.
- Mind-Body Therapies: These include techniques such as meditation, deep breathing, and yoga that help in managing pain by improving mental health. They focus on the interaction between the mind, body, and behavior to affect physical functioning and promote health.
For any treatment approach, it’s essential to have a thorough understanding of the patient’s medical history, the intensity, duration, and location of the pain, and the patient’s personal preferences and lifestyle. A multidisciplinary approach that combines different techniques often yields the best results.
Frequently Asked Questions
Can Pregnant Women Receive Epidural Injections Safely?
When contemplating pain management options for pregnant women, it is essential to weigh the potential benefits and risks. Although generally safe, any medical procedure, including those for pain relief, carry some level of risk.
Does Insurance Typically Cover the Cost of Epidural Injections?
Insurance coverage for medical procedures can vary widely. Typically, insurance limitations and plan specifics dictate coverage. Patients may face out-of-pocket expenses depending on their deductible, copayment, and coinsurance obligations. Always verify with your insurance provider.
Are There Any Dietary Restrictions Before or After an Epidural Injection?
Generally, there are no specific dietary restrictions related to injection preparation or post-injection exercise. However, it is advisable to maintain a healthy diet and hydration level for best recovery and overall wellness.
What Qualifications Should a Medical Professional Have to Administer Epidural Injections?
To administer any specialized medical procedures, professionals must possess extensive training. Specifically, Epidural Injection Training is needed, ensuring they understand Epidural Administration Risks and are capable of effectively mitigating potential complications for the patient’s safety.
Can Epidural Injections Interact With Other Medications I Might Be Taking?
Yes, interactions can occur depending on injection timing and medication type. It’s crucial to inform your healthcare provider about all medications you’re currently taking to guarantee the safety and effectiveness of the treatment plan.