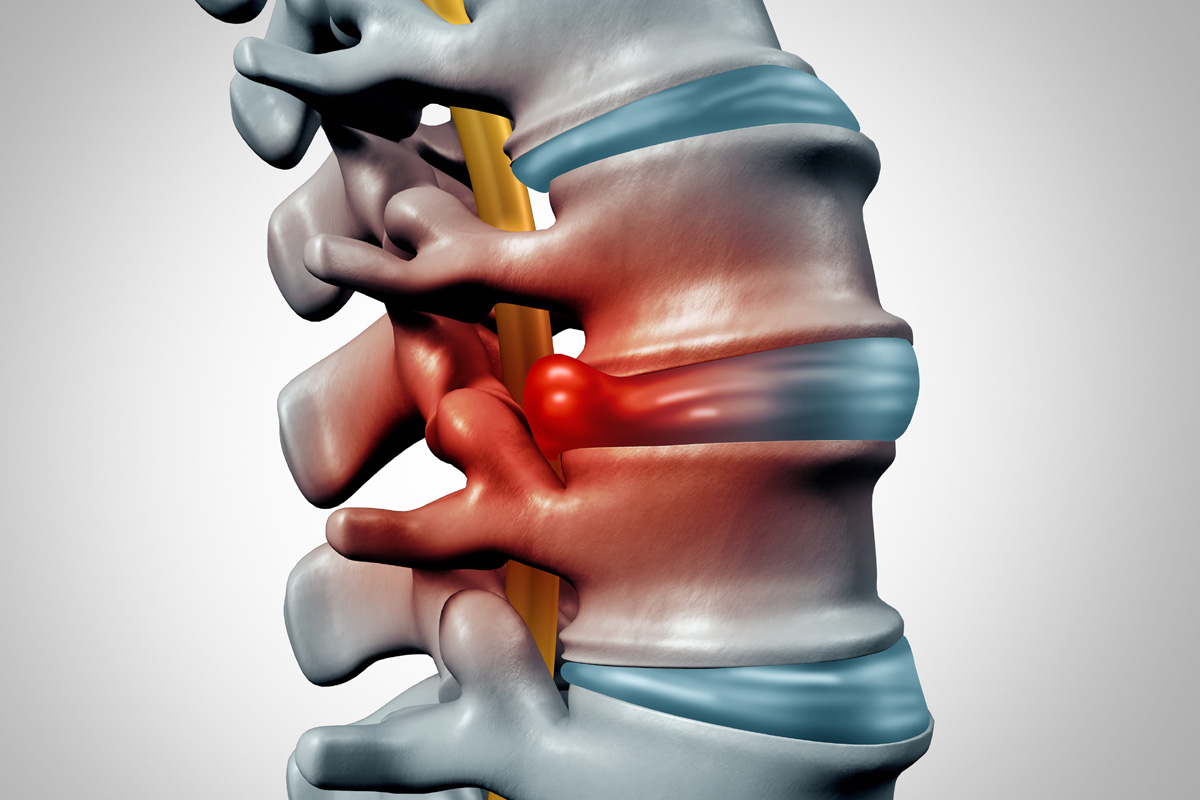
In the domain of back pain, the intricacies of facet pain and disc pain often stir debate among professionals. They, while being distinct in origin and presentation, continue to be intertwined in the overall narrative of spinal health. The nuances in understanding their causes, symptoms, and treatment options become critical for effective patient management. Indeed, the question that arises is how best to differentiate and manage these two conditions? The answer lies in a detailed exploration of their unique characteristics.
Understanding Facet Pain
To fully understand facet pain, it is essential to explore the anatomy and functions of the facet joints in the human body, primarily focusing on their role in the spine’s stability and movement. Facet joints, small stabilizing joints located between and behind adjacent vertebrae, provide the spine with both stability and flexibility, allowing for a wide range of movements.
Facet inflammation triggers can occur through several channels, the most common of which include physical strain or injury, and aging, which leads to wear and tear of these joints. The inflammation results in facet pain, a discomfort usually felt in the neck, back, or lower back regions, depending on the affected facet joints.
Preventive measures for facet pain revolve around maintaining good spinal health. Regular physical activity, maintaining a healthy weight, and practicing good posture can greatly reduce the risk of developing facet pain. In addition, lifestyle modifications such as avoiding smoking and incorporating a balanced diet rich in calcium and vitamin D can also play a significant role in preventing facet pain. Importantly, these preventive measures are not only beneficial for facet pain but also contribute to overall spinal health.
Common Causes of Facet Pain
Delving further into the etiology of facet pain, it is essential to identify the common causes that lead to such discomfort, ranging from degenerative disorders to traumatic injuries. The facet joints, much like any other joints in the body, are susceptible to wear and tear, primarily due to aging. This progressive degeneration can result in facet joint arthritis, one of the leading causes of facet pain.
In addition to aging, traumatic injuries to the spine – such as those obtained from falls or vehicular accidents – can lead to facet pain. These injuries may cause sudden and severe inflammation, one of the major facet inflammation triggers, resulting in acute pain.
Lifestyle plays an integral role in the onset of facet pain. Sedentary habits, obesity, and poor posture are significant contributors. Lifestyle modifications, hence, are often recommended in the management of facet pain. Regular exercise, maintaining a healthy weight, and adopting a good posture can help reduce the strain on the facet joints and ameliorate the associated discomfort.
Symptoms Associated With Facet Pain
Having explored the common causes of facet pain, we now turn our attention to the symptoms that are typically associated with this condition. The most common symptom of facet pain is a localized, sharp discomfort in the back. This can be accompanied by a radiating ache that extends into the buttocks and down the back of the legs. The pain is often exacerbated by specific movements, such as twisting, bending, or standing up from a seated position.
Pain management techniques are vital in mitigating these symptoms. Nonsteroidal anti-inflammatory drugs (NSAIDs) and physical therapy are usually the first line of treatment. Interventional procedures like facet joint injections may also be considered for more severe or persistent cases.
Moreover, lifestyle modifications play a significant role in managing facet pain. Patients are encouraged to maintain a healthy weight, as excess body mass can put considerable strain on the facet joints. Regular exercise, particularly activities that strengthen the core muscles, can help support the spine and alleviate pressure on the joints. Additionally, proper posture, both when standing and sitting, is essential to minimize stress on the facet joints.
Understanding these symptoms and management strategies can help patients lead a comfortable life despite their condition.
Diagnosis Procedures for Facet Pain
The diagnosis of facet pain involves a meticulous process, typically commencing with an in-depth evaluation of the patient’s symptoms. This is followed by a thorough medical examination aimed at discerning the source of discomfort. The use of advanced imaging techniques further augments this diagnostic procedure, providing detailed insights into the patient’s condition.
Identifying Facet Pain Symptoms
To accurately identify facet pain symptoms, medical professionals employ a variety of diagnostic procedures, ensuring precise detection and subsequent treatment. These symptoms often emanate from facet joint degeneration, a condition that can be managed effectively with the right diagnosis and facet pain prevention strategies. Patients typically present with signs such as discomfort while leaning backwards, pain on one side of the spine, and difficulty in twisting the body. These symptoms can intensify with standing or increased activity. Other signs may include tenderness in the lower back region or radiating pain down the legs. Recognizing these symptoms early is critical in slowing down the degenerative process and implementing appropriate preventive measures. Hence, the importance of a thorough and meticulous approach to diagnosis cannot be overstated.
Medical Examination for Facet Pain
In the field of medical practice, a thorough assessment for facet pain typically involves a series of diagnostic procedures designed to accurately pinpoint the source of the discomfort. These processes are essential to formulating effective pain management techniques. A detailed clinical examination is the first step, where a detailed patient history is taken, followed by a physical examination focusing on the spine. This can help ascertain if the pain is stemming from the facet joints. Another vital part of the examination is the pain pattern analysis, which can provide valuable insights into the cause of the pain. Alternative therapies may also be explored, depending on the patient’s condition and response to conventional treatments. These diagnostic methods contribute to a robust and holistic approach to treat facet pain.
Imaging Techniques in Diagnosis
Harnessing the power of modern imaging techniques, medical professionals can further refine their diagnosis and treatment plans for patients suffering from facet pain. Radiographic advancements have greatly enhanced the precision of these diagnostic procedures. Techniques such as computed tomography (CT) provide detailed images of the spinal anatomy, aiding in the identification of facet joint abnormalities. Contrast MRI benefits are particularly remarkable in this scenario. It allows for the visualization of soft tissues and nerves, granting a more detailed overview of the patient’s condition. This can help pinpoint inflammation or degeneration within the facet joints. By combining these techniques, clinicians can establish a more precise diagnosis, ultimately leading to targeted and effective treatment plans for facet pain.

Treatment Options for Facet Pain
While managing facet pain can be challenging, various treatment options exist, ranging from conservative methods like physical therapy and medication to more invasive procedures such as nerve blocks or surgery. Physical therapy often forms an integral part of pain management, aiming to strengthen the back muscles and improve flexibility. Medication, including non-steroidal anti-inflammatory drugs or corticosteroid injections, can reduce inflammation and pain.
Alternative therapies, such as chiropractic manipulations, acupuncture, and yoga, have also shown promise in managing facet pain by promoting overall well-being and reducing stress, which can exacerbate pain. These therapies can be used in conjunction with traditional treatments to enhance their effectiveness.
More invasive options are considered when conservative treatments fail to provide relief. Nerve blocks involve injecting an anesthetic near the spinal nerves to block pain signals. If the pain persists, surgery, such as a facet rhizotomy or spinal fusion, may be considered. These procedures aim to permanently alleviate pain by removing or immobilizing the problematic facet joint. However, as with all surgical procedures, they carry potential risks and complications and hence, are generally considered as a last resort.
Living With Facet Pain
Despite the availability of various treatment options, it is an unfortunate reality that some individuals must learn to navigate daily life with persistent facet pain. This chronic pain, originating from the facet joints in the spine, can have a substantial impact on an individual’s quality of life. However, through a combination of pain management techniques and lifestyle adaptations, it is possible to mitigate the impact of facet pain on daily activities.
Pain management techniques, such as physical therapy, medication, and nerve block injections, can be utilized to reduce the intensity of pain. A detail-oriented approach to physical therapy, focusing on strengthening the muscles that support the spine, can help alleviate pressure on the facet joints, thereby lessening pain. Similarly, medications can be prescribed to reduce inflammation and provide relief.
Lifestyle adaptations also play a critical role in managing facet pain. These can range from maintaining a healthy weight, which reduces pressure on the spine, to adopting ergonomically sound practices in daily routines. For instance, using a chair that provides proper lumbar support can make a significant difference. Additionally, incorporating low-impact exercises like swimming or cycling can also help in managing facet pain.
Understanding Disc Pain
Disc pain, a prevalent cause of back discomfort, warrants a thorough examination of its origins, manifestations, and therapeutic strategies. This will encompass an in-depth exploration of causative factors, an examination of the symptoms and diagnostic methods, followed by an evaluation of the available treatment options. Understanding these elements is crucial to facilitate effective management and mitigation of disc pain.
Causes of Disc Pain
Understanding the causes of disc pain requires a thorough exploration of the complex structure and function of the spinal disc. Disc pain often results from conditions that put pressure on the spinal cord or nerves, such as herniated discs and degenerative disc disease.
Here are some key causes of disc pain:
– Degeneration: As we age, our discs naturally degenerate and lose flexibility, elasticity, and shock-absorbing characteristics.
– Injury or Trauma: A sudden fall, a car accident, or any heavy strain can cause discs to herniate or rupture.
– Lifestyle Factors: Poor posture, lack of regular exercise, and unhealthy habits like smoking can accelerate disc degeneration.
Disc pain prevention and disc pain exercises are essential in managing these conditions. Proper understanding of the causes can help in formulating targeted treatment plans.
Symptoms and Diagnosis
Recognizing the symptoms of disc pain and ensuring an accurate diagnosis are vital steps in formulating appropriate and effective treatment strategies. Symptoms often manifest as recurrent, localized lower back pain, potentially radiating to the buttocks, thighs, and even the feet. Patients may also experience tingling or numbness, indicating neural involvement. Pain management techniques, such as patient education and physical therapies, are typically employed during the diagnostic process, providing temporary relief while clinicians work to pinpoint the precise cause of the discomfort. Imaging studies, such as MRI or CT scans, are often used in conjunction with clinical findings. Alternative therapies, such as acupuncture or chiropractic interventions, may also provide valuable diagnostic clues. A detailed and thorough diagnosis is essential to inform subsequent treatment plans.
Disc Pain Treatments
Having established the importance of accurate diagnosis in the management of disc pain, we now turn our attention to the various treatment modalities available for this condition.
The treatment of disc pain generally involves a multi-pronged approach, which can include:
- Disc Pain Prevention: This primarily involves lifestyle modifications such as maintaining a healthy weight, regular exercise, and avoiding activities that strain the back.
- Disc Pain Medication: These are often the first line of treatment, and can include over-the-counter pain relievers, narcotics, muscle relaxants, and even some types of antidepressants.
- Non-Surgical and Surgical Interventions: These can range from physical therapy and chiropractic adjustments to more invasive procedures like spinal injections or surgery.
With the right treatment protocol, disc pain can be effectively managed, improving patient’s quality of life.
Common Causes of Disc Pain
Disc pain, a pervasive issue in modern society, primarily stems from a variety of conditions such as herniated discs, degenerative disc disease, and disc desiccation. These conditions commonly result from the wear and tear of daily life, poor posture, and injury.
Herniated discs, also known as slipped or ruptured discs, occur when the soft inner portion of the disc protrudes through its tough outer layer. This can cause pressure on surrounding nerves, leading to disc pain. Degenerative disc disease is a condition characterized by the gradual deterioration of the discs due to aging or injury, causing them to lose their cushioning ability. Disc desiccation, on the other hand, refers to the dehydration of the discs, making them more prone to damage and pain.
Understanding these causes is essential for disc pain prevention and rehabilitation. Preventive measures primarily focus on maintaining a strong and flexible spine through regular exercise, proper posture, and a healthy diet. In contrast, rehabilitation techniques target the underlying cause of disc pain and often involve physical therapy, medication, and in some cases, surgery. Together, these strategies can alleviate disc pain and improve the quality of life for those affected.
Symptoms Associated With Disc Pain
Understanding the symptoms associated with disc pain is crucial for accurate diagnosis and effective treatment. This discussion will focus on the identification of disc pain symptoms and strategies to manage them. The aim is to provide a thorough understanding of disc pain, which can be complex and varied, to foster effective patient care.
Identifying Disc Pain
In the domain of spinal health, differentiating between disc pain and other types of back pain is essential, with disc pain typically manifesting through specific symptoms such as radiating or sharp pain, numbness, and weakness in the extremities.
- Radiating or sharp pain: This is often experienced in the lower back, buttocks, and down the legs. It can be particularly intense during certain movements or postures.
- Numbness: This may occur in areas that correlate to the affected disc, such as the lower back, thighs, or calves.
- Weakness in the extremities: This symptom frequently accompanies disc pain and can hinder normal activities, including ‘Disc pain exercises’ aimed at ‘Disc pain prevention’.
Effective identification of these symptoms can facilitate early intervention and appropriate therapy, preventing further complications.
Managing Disc Pain Symptoms
While managing disc pain symptoms can be challenging, early detection and proper treatment can greatly alleviate discomfort and improve the quality of life for those affected. Disc Pain Prevention starts with lifestyle adjustments such as maintaining a healthy weight, regular physical activity, and proper lifting techniques to mitigate strain on the spine. It’s important to understand that these proactive measures not only manage existing pain but also prevent potential disc issues. Over-the-counter medications, physical therapy, and in some cases, surgical interventions may be part of a thorough treatment plan. Nonetheless, the role of lifestyle modification remains essential. Balancing rest with activity, adopting a nutrient-rich diet, and managing stress can play a significant role in managing disc pain symptoms effectively.
Diagnosis Procedures for Disc Pain
Discerning the cause of disc pain often requires a thorough diagnosis procedure that includes medical history review, physical examination, and advanced imaging techniques. Understanding the patient’s medical history can provide insight into potential causative factors, such as previous injuries or conditions that may predispose an individual to disc pain.
During the physical examination, the physician may test for pain points, range of motion, and any neurological symptoms. This can help identify whether disc pain is a result of a herniated disc, degenerative disc disease, or other spinal disorders.
Advanced imaging techniques, such as MRI and CT scans, are instrumental in confirming the diagnosis. These techniques provide detailed images of the spinal cord and surrounding structures, enabling doctors to pinpoint the exact location and nature of the disc issue.
Incorporating disc pain prevention strategies and disc pain exercises at this stage is essential to promote future health and well-being. These could include:
- Regular physical activity to maintain spine health and flexibility
- Proper posture to avoid unnecessary strain on the discs
- Weight management to reduce pressure on the spine
Each step in the diagnosis procedure is vital in determining the most effective treatment plan for disc pain, tailored to each individual’s needs and condition.
Treatment Options for Disc Pain
After a thorough diagnostic procedure has pinpointed the nature and location of disc pain, the next step involves exploring the various treatment options available to manage and alleviate the discomfort. Treatment strategies are typically multi-faceted, combining pain management techniques with restorative procedures to promote healing and restore functionality.
Pain medication is often the first-line treatment for disc pain. These medicines range from over-the-counter analgesics, such as ibuprofen, to prescription drugs like opioids for severe pain. However, their role is extremely important, mitigating symptoms without addressing the root cause of the pain.
In cases where conservative treatments fail to provide adequate relief, surgical interventions may be considered. Disc replacement is one such option. This procedure involves removing the damaged disc and replacing it with an artificial one. The aim is to preserve motion in the spine while eliminating the source of the pain. It is important to note that disc replacement is typically reserved for patients who have not responded to conservative treatments, as it carries more risks and requires a longer recovery period than non-surgical treatments.
Frequently Asked Questions
Can Facet Pain and Disc Pain Occur Simultaneously?
Yes, facet pain and disc pain can occur simultaneously, necessitating thorough pain management techniques. Depending on severity, both conditions might require surgical interventions to alleviate discomfort and improve overall musculoskeletal health.
What Lifestyle Changes Can Prevent Facet and Disc Pain?
Lifestyle changes such as maintaining a balanced diet, reducing dietary impact by limiting inflammatory foods, and implementing a regular exercise regime can greatly influence the prevention of these types of musculoskeletal pains.
How Does Age Affect the Likelihood of Developing Facet or Disc Pain?
Age notably influences the likelihood of developing pain due to age-related degeneration. As individuals age, the risk of disc and facet degeneration increases, necessitating more effective pain management techniques to maintain quality of life.
Can Facet or Disc Pain Lead to Permanent Disability?
Yes, both facet and disc pain can potentially lead to permanent disability if not properly managed. Pain management strategies are key in preventing disability implications and maintaining quality of life.
What Is the Long-Term Prognosis for People With Chronic Facet or Disc Pain?
The long-term prognosis for individuals with chronic pain varies greatly. It largely depends on the effectiveness of pain management techniques, patient’s overall health, and the potential need for surgical interventions.