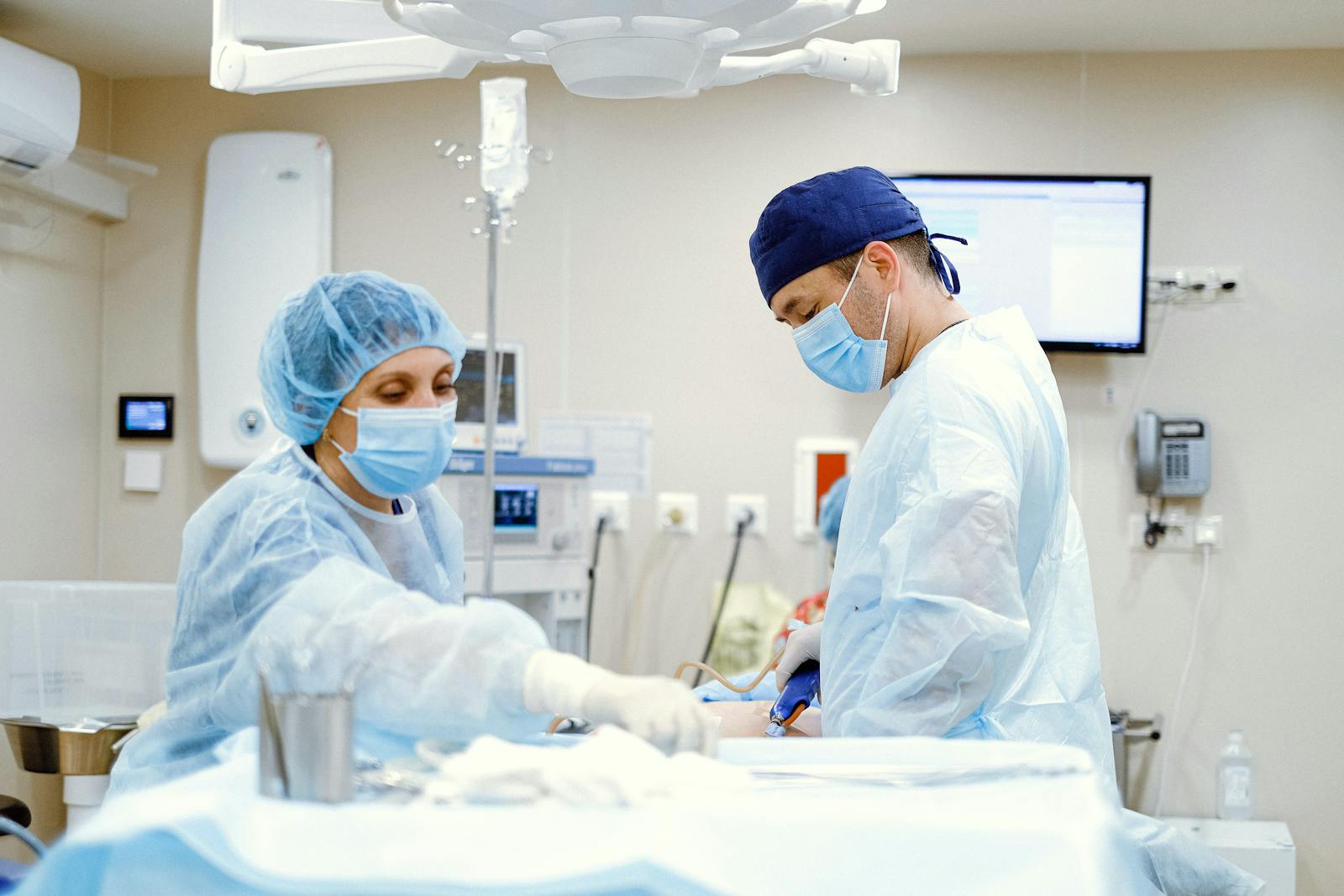
In the domain of neurosurgery, Rhizotomy stands as a beacon of hope for those burdened by chronic pain or muscle hyperactivity. This intricate procedure, involving the selective severing of spinal cord nerve roots, has evolved greatly over the years, providing an enhanced level of precision and safety. The far-reaching implications of Rhizotomy, spanning conditions such as spastic diplegia and trigeminal neuralgia, underscore its potential in transforming lives. Yet, the success of this procedure hinges on meticulous patient evaluation, preparation, and postoperative care. How does this process unfold, and what factors contribute to its success?
Understanding Rhizotomy
Rhizotomy, a surgical procedure often utilized in the neurosurgical field, involves the selective severing of problematic nerve roots in the spinal cord to alleviate chronic pain or muscle hyperactivity. This process requires a profound understanding of the anatomical and physiological intricacies of the nervous system. It is a procedure laden with potential misconceptions that necessitate clarification.
One common Rhizotomy misconception is the belief that it could lead to total loss of sensation or movement. While the procedure does involve severing nerve roots, it is a highly targeted process. Only the faulty nerves causing pain or abnormal muscle activity are severed, leaving healthy nerves intact. The process aims to maintain as much function and sensation as possible.
Recent Rhizotomy advancements have further improved the precision and safety of the procedure. Developments in imaging technology, such as high-resolution magnetic resonance imaging (MRI), have provided neurosurgeons with detailed, three-dimensional images of the nervous system. This allows for more accurate identification of problematic nerves. Additionally, advancements in surgical tools and techniques have enhanced the ability to perform minimally invasive Rhizotomies, reducing potential risks and promoting faster recovery.
History of Rhizotomy
The history of rhizotomy, a surgical procedure to sever nerve roots in the spinal cord, spans from ancient origins to modern advancements. Early implementations of this technique can be traced back to ancient civilizations, where it was used as a rudimentary form of pain management. The development and refinement of rhizotomy in contemporary medicine, however, has seen significant enhancements in precision, safety, and efficacy.
Rhizotomy’s Ancient Origins
Delving into the annals of medical history, it becomes evident that the inception of rhizotomy traces back to the ancient civilizations, where primitive versions of this surgical procedure were already being practiced. Rooted within ancient methodologies and cultural practices, the history of rhizotomy is indeed fascinating and illuminating.
- The procedure was first performed in ancient Egypt, as depicted in papyrus medical texts.
- In ancient Greece, Hippocrates, often referred to as the father of medicine, made references to early forms of rhizotomy.
- A similar procedure was known to be practiced in ancient India, as evidenced by Sanskrit texts.
- There are also records of such procedures in ancient Chinese medical literature.
- The early Romans, too, were known to have performed rudimentary forms of rhizotomy.
This historical perspective helps us understand the evolution of this medical procedure.
Modern Rhizotomy Development
Despite its ancient origins, it was not until the late 19th and early 20th centuries that rhizotomy underwent significant advancements, as medical understanding and surgical techniques evolved. Rhizotomy advancements were facilitated by the development of precise neuroimaging techniques, especially magnetic resonance imaging (MRI) and computed tomography (CT) scans. These technologies allowed for accurate targeting of the nerve roots, minimizing complications and enhancing patient outcomes. Additionally, the advent of electrophysiological monitoring techniques has been instrumental in identifying and preserving necessary sensory functions. Technology’s role in this evolution cannot be overstated; it has not only improved the precision and effectiveness of rhizotomy procedures but has also widened the scope of conditions that can be treated, thereby significantly benefiting patients afflicted with chronic pain or spasticity.
Rhizotomy Procedure Explained
Performing a rhizotomy involves a carefully orchestrated series of steps designed to selectively sever problematic nerve roots in the spinal cord, thereby alleviating chronic pain or spasticity. Despite some rhizotomy misconceptions, this procedure’s efficacy is well-documented, even though alternative treatments may also be considered depending on the individual’s condition.
The rhizotomy procedure is typically executed as follows:
- Initial assessment and diagnosis: Determining the appropriateness of rhizotomy as treatment based on patient’s symptoms and medical history.
- Preoperative preparations: Includes acquiring informed consent, performing any necessary diagnostic tests, and planning the surgical approach.
- Intraoperative procedure: The surgeon uses fluoroscopy to guide a needle to the specific nerve root, then electrical stimulation is employed to confirm correct placement before the nerve is cut.
- Postoperative care: Close monitoring of patient’s vital signs, pain levels and nerve function is done. Rehabilitation exercises are often prescribed to maximise recovery.
- Follow-up evaluations: Regular assessments are performed to monitor the patient’s progress after the procedure.
Each step in the process is integral to the overall success of the treatment, and any changes or deviations can impact the outcome. It’s important for patients to consult with experienced medical professionals when considering rhizotomy.
Types of Rhizotomy
Branching from the main topic of rhizotomy, there are several distinct types of this procedure, each of which targets different nerve roots and offers unique benefits and potential drawbacks based on the specific medical condition being addressed.
The types of rhizotomy include, but are not limited to, the Selective Dorsal Rhizotomy (SDR), the Percutaneous Rhizotomy, and the Radiofrequency Rhizotomy. Each employs different techniques and technologies to sever nerve roots and alleviate pain or spasticity. For instance, the SDR is often utilized in cases of spastic diplegia, a form of cerebral palsy, while the Radiofrequency Rhizotomy uses thermal energy to disrupt nerve function and is typically indicated for trigeminal neuralgia.
Despite the effectiveness of these procedures, some rhizotomy misconceptions persist, primarily arising from a lack of understanding or misinformation about the procedure’s risks and benefits. It is essential to dispel these misconceptions through patient education and consultation with experienced neurosurgeons.
Alternatives to rhizotomy, such as neuromodulation or pharmacological treatments, might be considered when the risks of rhizotomy outweigh the potential benefits, or if the patient’s condition does not align with the specific indications for rhizotomy. These alternatives, however, have their own unique benefits and drawbacks that need to be carefully evaluated against the patient’s specific needs and medical condition.
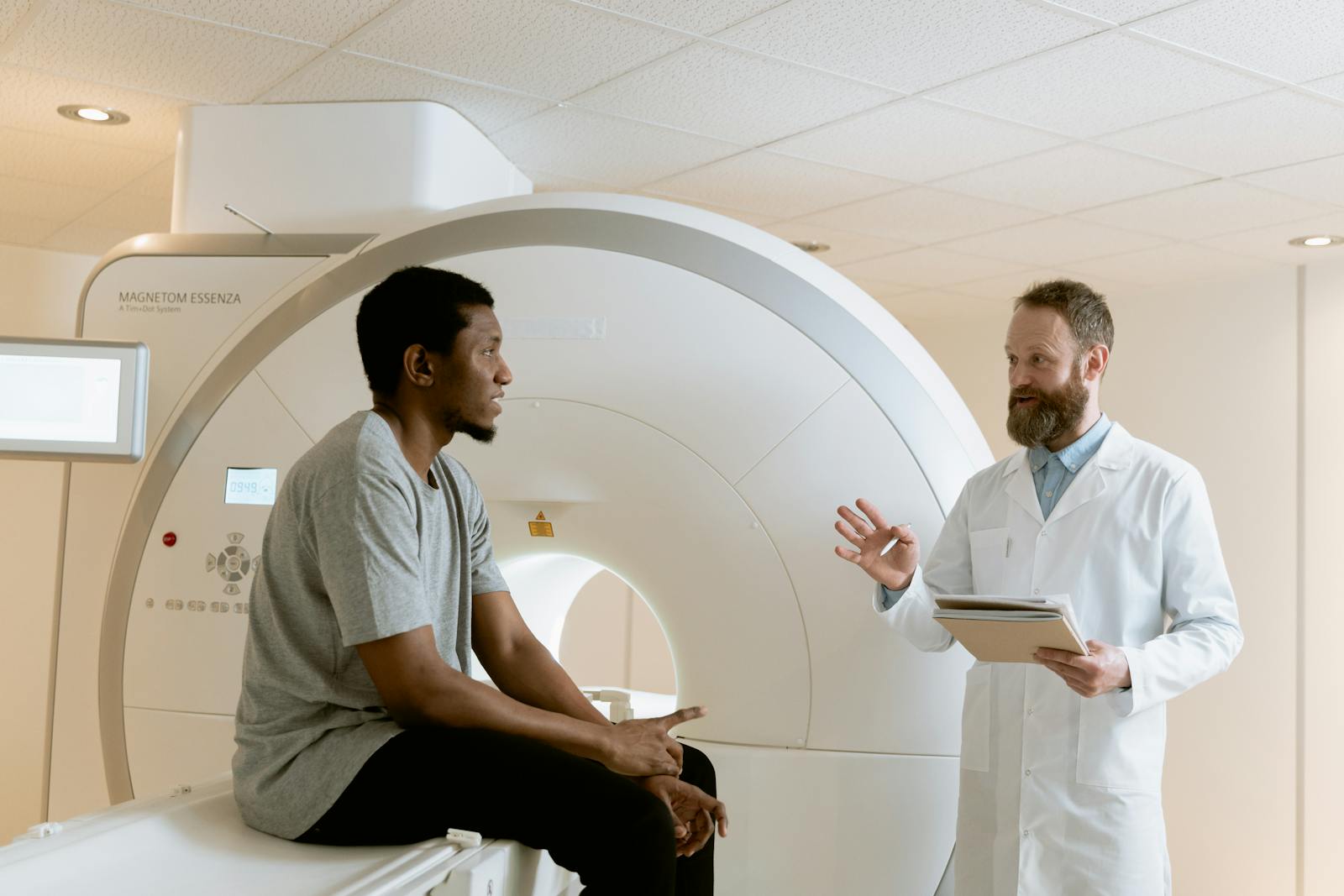
Evaluating Patient Suitability
After considering the different types of rhizotomy and potential alternatives, it becomes evident that not all patients are suitable candidates for this procedure; hence, a detailed evaluation process is indispensable to identify those who would benefit most. This process comprises multiple steps that address a range of factors, including medical, financial, and lifestyle considerations.
A thorough patient suitability assessment for rhizotomy includes:
- Detailed medical history and physical examination: These initial steps are important to evaluate the severity of symptoms, patient’s overall health status, and potential risks associated with the procedure.
- Neurological assessment: To determine the nerve roots involved and the potential effectiveness of rhizotomy.
- Rhizotomy cost analysis: A complete financial evaluation is required to assess the affordability of the procedure for the patient.
- Alternative treatment comparisons: Comparing the effectiveness, risks, and costs of alternative treatments can help to make an informed decision.
- Psychological assessment: Understanding the patient’s expectations, willingness to undergo the procedure, and capacity to manage potential postoperative challenges are also crucial.
Benefits of Rhizotomy
When appropriately administered, rhizotomy can offer significant relief from chronic pain, dramatically improving the quality of life for patients suffering from conditions such as spinal disorders or cerebral palsy. This surgical procedure, which involves the selective severing of nerve roots near the spinal cord, has been found effective in reducing spasticity and enhancing mobility.
In comparison to rhizotomy alternatives, this intervention often provides more durable and longer-lasting relief. While methods like nerve blocks or injections may offer temporary relief, they generally require ongoing maintenance and repeated procedures. Rhizotomy, on the other hand, can result in sustained alleviation of symptoms, making it a preferred option for many patients and clinicians.
Furthermore, given its proven efficacy, rhizotomy is often covered by insurance plans, making it financially accessible for a broader population. Though the exact degree of insurance coverage varies depending on the individual’s policy, the procedure is typically recognized as a valid and necessary medical intervention. As a result, patients considering this treatment can often secure financial assistance, mitigating the burden of healthcare costs.
Potential Rhizotomy Risks
While rhizotomy can offer significant relief from chronic pain, it is essential to contemplate the potential risks associated with the procedure. This discussion will cover the complications that could arise during or after a rhizotomy, the factors that could increase the risk of such complications, and the potential hazards that may present post-procedure. Providing a thorough understanding of these risks is vital in making informed decisions about undergoing rhizotomy.
Understanding Rhizotomy Complications
Despite its proven benefits, rhizotomy, like any surgical procedure, is not without potential complications and risks that need careful consideration. These complications can range from minor to severe and may require immediate complication management or exploration of rhizotomy alternatives.
Some potential complications include:
- Nerve Damage: This could result in loss of sensation or motor function.
- Infection: As with any surgical procedure, there’s a risk of infection.
- Bleeding: This is a potential risk, especially if the patient has a clotting disorder.
- Allergic Reaction: Patients may have adverse reactions to anesthesia or other medications used.
- Increased Pain: In some cases, the procedure may lead to an increase in pain rather than the intended relief.
Understanding these potential complications is vital for patients and medical professionals alike.
Pre-Rhizotomy Risk Factors
Before undergoing a rhizotomy procedure, it is important to identify and understand certain preoperative risk factors that could potentially increase the likelihood of complications. Risk assessment methods are employed to evaluate a patient’s overall health status, including cardiovascular fitness and neurological stability. Conditions such as obesity, diabetes, or heart disease can pose significant risks during the procedure. Pre-existing neurological conditions could also elevate the chances of negative outcomes. As a result, non-surgical alternatives are often considered for high-risk patients. These alternatives could include pain management through medication, physical therapy, or lifestyle changes. Consequently, a thorough evaluation of these pre-rhizotomy risk factors is essential to mitigate potential risks and ensure the best possible outcomes for patients.
Post-Procedure Potential Hazards
Following the rhizotomy procedure, patients may encounter certain postoperative hazards, which can range from minor discomfort to more serious neurological complications. These potential complications can be broadly categorized into physical and psychological effects.
- Post rhizotomy infections: Despite sterile surgical procedures, there’s a risk of infection at the surgical site.
- Hematoma: Blood may collect outside blood vessels, leading to swelling and discomfort.
- Nerve damage: The procedure involves the manipulation of nerve roots, which can result in temporary or permanent nerve damage.
- Pain or discomfort: Despite being a procedure to alleviate pain, some patients may experience increased pain postoperatively.
- Psychological impact: The prospect of enduring these risks can cause emotional distress and anxiety, which can affect the patient’s overall recovery and quality of life.
These risks underline the need for careful patient evaluation and meticulous surgical technique.
Preparing for a Rhizotomy
In anticipation of a rhizotomy, a detailed and meticulous preparation process is important to guarantee the success and safety of the procedure. The initial stage of preparation involves a thorough rhizotomy cost analysis. This allows patients to understand the full financial implications of the procedure. Being a complex neurological procedure, expenses can be substantial, encompassing surgeon’s fees, facility costs, anesthesia, and post-operative care.
To mitigate these costs, an exploration of insurance coverage is necessary. Patients should contact their insurance provider to verify the extent of coverage for the rhizotomy procedure. Some insurance companies may require a pre-authorization, necessitating the submission of medical documentation to justify the medical necessity of the procedure. In some cases, insurance may only cover a portion of the costs, leaving the patient responsible for the remaining balance.
Prior to the procedure, a thorough medical evaluation is conducted, including imaging studies such as MRI or CT scans to provide clear visualization of the nerve roots targeted for the procedure. Additionally, a complete blood count, coagulation profile, and other lab tests may be required to assess the patient’s overall health and readiness for the surgery.
The patient is also educated about the procedure, its benefits, potential risks and alternatives, enabling informed decision-making.

Rhizotomy Recovery Process
The post-operative period of a rhizotomy, often pivotal in determining the procedure’s success, typically involves a thorough recovery process to guarantee ideal healing and functionality. The recovery process is multifaceted, focusing not only on physical healing but also addressing post rhizotomy diet and emotional support needs.
The key elements of a successful rhizotomy recovery process include:
- Physical Therapy: This is often required to improve mobility and strength in the affected areas post-procedure.
- Post Rhizotomy Diet: Proper nutrition is critical for the body to heal. A diet rich in proteins, vitamins, and minerals is typically recommended.
- Emotional Support: Given the intensity of the procedure, emotional support is paramount. This can be provided by mental health professionals, family, or support groups.
- Pain Management: This is usually achieved through a mix of medications and alternative therapies like heat or cold application.
- Regular Follow-ups: To monitor healing progress and address any complications promptly, regular check-ups with the healthcare provider are essential.
Each patient’s recovery process will be individualized, depending on their specific needs and circumstances. The ultimate goal is to restore function and improve the patient’s quality of life.
Life After Rhizotomy
Adjusting to life post-rhizotomy often necessitates a comprehensive approach that addresses physical, psychological, and lifestyle changes to facilitate best patient outcomes. Pain management alternatives become a significant part of the process. These may include physical therapy, over-the-counter medications, or complementary therapies like acupuncture, yoga, or mindfulness meditation. These strategies can help manage residual pain and improve overall wellbeing, fostering a higher quality of life post-procedure.
Equally important is addressing the emotional impact post rhizotomy. Patients may experience a range of emotions, from relief due to pain reduction, to anxiety about potential recurrence or procedure-related complications. Psychological interventions, including cognitive-behavioral therapy (CBT) or counseling, can be beneficial in helping manage these emotional responses.
Further, lifestyle modifications may also be necessary, depending on the patient’s condition and recovery progress. These could involve changes in daily activities, work schedules, or even leisure pursuits, all aimed at ensuring optimal recovery and health maintenance. Regular follow-ups and consultations with the healthcare team are also integral to monitor progress and make necessary adjustments.
Rhizotomy Success Stories
Often, individuals who have undergone rhizotomies provide compelling narratives of significant pain reduction and improved quality of life. These stories, steeped in patient resilience, are a proof of the enduring hope and tenacity exhibited by those who choose to undergo this procedure.
- Case 1: A 45-year-old male with chronic back pain reported a 90% reduction in pain after the procedure. His improved mobility allowed him to return to work and engage in regular physical activities, greatly enhancing his quality of life.
- Case 2: A woman suffering from severe facial spasms underwent a rhizotomy. Post-procedure, she reported complete cessation of spasms, allowing her to regain her social life.
- Case 3: A 60-year-old woman with debilitating pain due to lumbar spinal stenosis reported a marked reduction in pain, allowing her to walk without assistance for the first time in years.
- Case 4: A young man suffering from spastic cerebral palsy underwent rhizotomy. The procedure significantly reduced his muscle stiffness, enabling better mobility and independence.
- Case 5: A patient with trigeminal neuralgia reported a near-complete elimination of facial pain after rhizotomy, restoring his ability to eat and speak without discomfort.
These stories of success illuminate the potential benefits of rhizotomy, instilling hope in prospective patients.
Frequently Asked Questions
Is Rhizotomy Covered by Most Health Insurance Plans?
Coverage for medical procedures varies widely among health insurance plans. Factors such as specific procedure costs and insurance limitations often determine whether a particular service, like rhizotomy, is included in an individual’s coverage.
Are There Any Alternatives to Undergoing a Rhizotomy?
Yes, there are alternatives to invasive procedures. These include physical therapy, nerve blocks, and medication management. It is essential to explore these options, given the potential risks associated with procedures such as rhizotomy.
Can a Rhizotomy Be Performed on Children?
Yes, a rhizotomy can be performed on children, especially those with cerebral palsy. The success rate is high, but it requires thorough evaluation before surgery and post-rhizotomy rehabilitation to guarantee excellent outcomes.
Is the Rhizotomy Procedure Performed Worldwide?
Indeed, the rhizotomy procedure is performed globally, with varying success rates and potential complications. Its adoption is widespread due to its efficacy in alleviating chronic pain, despite the risk of potential postoperative complications.
What Are the Qualifications of a Surgeon Performing a Rhizotomy?
A surgeon performing this procedure should possess extensive neurosurgical training, experience in stereotactic neurosurgery, and a thorough understanding of potential rhizotomy risks and necessary patient preparation. Board certification is also typically required.