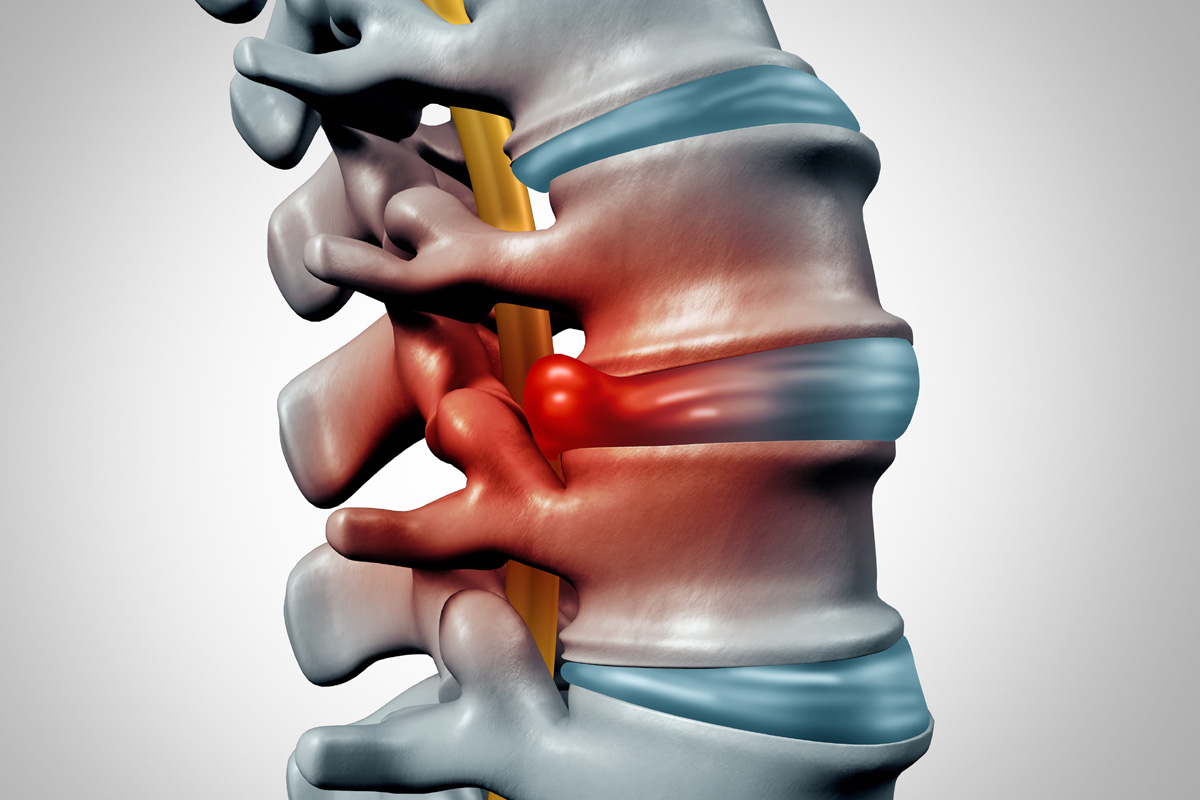
Spinal stenosis, a condition characterized by the narrowing of spinal spaces, poses consequential implications for the patient’s mobility and overall quality of life. The condition is primarily associated with aging, genetic predispositions, and past injuries, presenting symptoms ranging from mild discomfort to debilitating pain. Further exploration into the detailed anatomy of the spine, the gradual progression of the condition, and the varying treatment avenues can provide a thorough understanding of spinal stenosis. The complexity of the condition and the necessity for early diagnosis and tailored treatment plans emphasize the importance of continued discourse in this field.
Understanding Spinal Stenosis
Despite being a common condition, spinal stenosis, a narrowing of the spaces within your spine, requires a profound understanding due to its complex nature and potential impact on the nervous system. This degenerative condition often progresses slowly, with stenosis progression often linked to the natural aging process, although other factors such as genetic predisposition, spinal injury, and certain health conditions may influence its progression.
The stenosis progression primarily affects the spinal canal, compressing the nerves and causing symptoms ranging from mild discomfort to debilitating pain. Additionally, it can lead to neurogenic claudication, characterized by pain and cramping in the legs during walking or prolonged standing.
Understanding spinal stenosis is not just about recognizing its pathophysiology, but also about exploring alternative therapies. These may include physical therapy, acupuncture, and chiropractic care, which can complement conventional treatments like medications and surgery. Physical therapy, for example, strengthens the muscles to support the spine better, while acupuncture and chiropractic care can help alleviate pain and improve mobility. Alternative therapies offer non-invasive options for patients, potentially reducing the need for surgical interventions or easing the symptoms for those who cannot undergo surgery.
The Anatomy of the Spine
To fully comprehend the condition of spinal stenosis, an in-depth knowledge of the spine’s intricate anatomy—comprising vertebrae, intervertebral discs, spinal cord, and nerve roots—is fundamentally essential.
The spine is a complex structure with an essential role in vertebral function and nervous system integration. It’s composed of various components, each with a specific and critical role. Some of the key elements include:
- Vertebrae: These are the bony structures that make up the spine, providing both structure and protection. They house the spinal cord and facilitate vertebral function by allowing movements like bending and twisting.
- Intervertebral discs: These are the cushion-like structures located between each vertebra. They act as shock absorbers, preventing damage from everyday activities or sudden impacts.
- Spinal Cord: This is the main pathway for information flowing back and forth between the brain and the rest of the body, playing a pivotal role in nervous system integration.
- Nerve Roots: These are the points where nerves branch off from the spinal cord, extending to various parts of the body.
Understanding the functional anatomy of the spine is key to grasping how spinal stenosis can have a significant impact on a person’s daily living activities.
Common Symptoms of Spinal Stenosis
Manifestations of spinal stenosis, a condition typified by the narrowing of the spinal canal, are varied and often greatly impede the afflicted individual’s daily activities. The Stenosis Impact on Mobility is important, as it often results in pain, numbness, or muscle weakness, particularly in the legs. These physical symptoms, in turn, can lead to difficulties in walking or maintaining balance.
Moreover, spinal stenosis can cause neurogenic claudication, a constriction of the nerves in the lower spine. This condition often manifests as discomfort or cramping in the legs that intensifies with standing or walking and alleviates when sitting or leaning forward.
In addition to these physical symptoms, the Psychological Effects of Stenosis should not be overlooked. Chronic pain and the resultant loss of mobility can lead to feelings of frustration, anxiety, and depression. The constant struggle with pain and impaired mobility can greatly diminish the quality of life, leading to a sense of helplessness and hopelessness.
In summation, spinal stenosis manifests as a complex interplay of physical symptoms and psychological impacts. Recognizing these common symptoms is important for early diagnosis and effective management of the condition.
Causes and Risk Factors
Understanding the causes and risk factors for spinal stenosis is essential in prevention, early detection, and effective treatment of the condition. Spinal stenosis is primarily caused by changes in the spine due to aging. However, certain factors increase the risk of developing the condition.
The following are the significant causes and risk factors for spinal stenosis:
- Genetic predisposition: Some people might be born with a narrow spinal canal or have structural deformities of the vertebrae that predispose them to spinal stenosis.
- Degenerative changes: Age-related changes in the spine such as herniated disks, thickened ligaments, bone spurs, and osteoarthritis can lead to spinal stenosis.
- Occupational hazards: Jobs involving heavy lifting, repetitive bending or twisting, or prolonged periods of vibration can cause wear and tear on the spine, leading to stenosis.
- Previous injury or surgery on the spine: A severe injury, or a previous surgery on the spine can cause inflammation and pressure on the spinal cord or nerves, resulting in stenosis.
Understanding these factors can help in the early detection and prevention of spinal stenosis, thereby improving the effectiveness of treatment strategies.
Spinal Stenosis in the Neck Vs Lower Back
While spinal stenosis can occur in any part of the spine, it is most frequently seen in the neck (cervical stenosis) and the lower back (lumbar stenosis), each presenting distinct symptoms and requiring differing treatment approaches due to anatomical variances.
The cervical stenosis impact is mainly on the upper body, as the spinal cord is compressed leading to pain, numbness, or weakness in the neck, arms, and hands. Additionally, coordination and balance issues can arise due to the disruption of nerve signals to the brain, sometimes leading to a staggering gait.
Lumbar stenosis, on the other hand, typically affects the lower body. Sciatica, characterized by pain, tingling, or numbness radiating down the legs, is a common symptom. The discomfort often exacerbates while standing or walking and can be somewhat relieved by bending forward or sitting down.
Lumbar stenosis management requires a more conservative approach initially, employing pain medications, physical therapy, or epidural steroid injections. If these fail to provide sufficient relief, surgical interventions may be considered to decompress the spinal canal. In contrast, cervical stenosis often necessitates surgery earlier due to the risk of severe neurological complications.
How Spinal Stenosis Is Diagnosed
The process of diagnosing spinal stenosis involves a thorough medical history assessment, meticulous physical examination, and the utilization of advanced imaging techniques. The primary goal is to identify the site and severity of the stenosis and to rule out other potential causes of the patient’s symptoms.
The diagnostic methods for spinal stenosis are multi-faceted and can include:
- A detailed medical history assessment: The clinician will gather in-depth information about the patient’s symptoms, their severity and duration, previous treatments, and the presence of any other health conditions.
- A thorough physical examination: This will typically include evaluation of the spine’s alignment, mobility, strength, reflexes, and sensations.
- Medical imaging: Techniques such as X-ray, Magnetic Resonance Imaging (MRI), and Computed Tomography (CT) scans are commonly used to visualize the spine and identify any narrowing of the spinal canal.
- Diagnostic tests: In some cases, additional tests like nerve conduction studies or electromyography may be required to further assess the impact of the stenosis on nerve function.
These detailed measures ensure an accurate diagnosis, which is essential for the development of an effective treatment plan.
Non-Surgical Treatment Options
In managing spinal stenosis, a range of non-surgical treatment options is available, each meticulously designed to relieve symptoms, improve mobility, and enhance the patient’s quality of life. These include both essential interventions like physical therapy and medication, as well as Alternative Therapies such as acupuncture, chiropractic adjustments, and massage.
Physical therapy is an essential component in the non-surgical management of spinal stenosis, focusing on strengthening the muscles that support the spine, improving flexibility, and promoting better posture. The use of analgesics, non-steroidal anti-inflammatory drugs (NSAIDs), and epidural steroid injections can effectively manage pain and inflammation.
Alternative Therapies can complement conventional treatments, providing additional symptomatic relief. Acupuncture, for instance, can alleviate pain by triggering the release of endorphins, the body’s natural painkillers. Chiropractic adjustments can align the spine, reducing pressure on the spinal cord or nerves.
Moreover, Decompression Techniques such as positional therapy and mechanical traction can alleviate the pressure on the spinal nerves, offering symptomatic relief. Positional therapy involves specific exercises or postures to open up the spinal canal, while mechanical traction uses a system of weights and pulleys to stretch the spine, creating space for the nerves.
Surgical Interventions for Spinal Stenosis
The surgical interventions for spinal stenosis represent a crucial aspect of patient management, especially when conservative measures fail to provide relief. Discussion of surgical options necessitates a thorough understanding of the procedures, their associated risks and complications, and the recovery process post-surgery. The following content will provide a detailed overview of these essential aspects to provide a clear understanding of the surgical interventions for spinal stenosis.
Understanding Spinal Stenosis Surgery
Exploring the complex web of surgical interventions for spinal stenosis, one must comprehend the intricate procedures, their potential outcomes, and the associated risks. Surgical alternatives might vary depending on the severity and location of the stenosis. Patient experiences also play an important role in understanding the effectiveness of these surgical interventions.
Some of the commonly performed procedures include:
- Laminectomy: Removal of the back part (lamina) of the affected vertebra.
- Foraminotomy: Enlargement of the vertebral foramen where nerve roots exit the spinal canal.
- Spinal fusion: Joins two vertebrae together to limit motion and relieve pain.
- Interspinous process devices: Placement of a spacer between spinous processes to alleviate pressure on spinal nerves.
Understanding these procedures can help patients make informed decisions about their treatment.
Risks and Complications
While surgical interventions for spinal stenosis often provide significant relief, they are not without potential risks and complications, ranging from infection and nerve damage to unexpected reactions to anesthesia. Stenosis progression may persist postoperatively, leading to recurrent symptoms. In addition, surgery can introduce new complications, such as dural tears, hematoma formation, or even spinal instability requiring additional intervention. Complication management is an essential part of the surgical plan, involving meticulous surgical technique, vigilant postoperative monitoring, and prompt response to adverse events. Additionally, patients may experience pain, numbness, or weakness post-surgery, which could affect their quality of life. It is essential that patients understand these risks and work closely with their healthcare providers to mitigate them.
Post-Surgery Recovery Process
After undergoing surgical intervention for spinal stenosis, patients enter a recovery phase that requires diligent attention to promote best results and minimize postoperative complications.
This phase encompasses various aspects, including:
- Pain Management: Appropriate analgesics are prescribed to control postoperative pain, facilitating physical rehabilitation.
- Physical Therapy: Customized exercise programs are initiated to improve mobility and strengthen back muscles.
- Follow-up Appointments: Regular consultations with the surgeon make sure the healing process is progressing as expected.
- Emotional Wellness: Psychological support may be needed to cope with anxiety or depression that can accompany long-term recovery.
Ultimately, the post-surgery recovery process is multifaceted and tailored to each patient’s needs, ensuring top-notch health outcomes following spinal stenosis surgery.
Living With Spinal Stenosis
Adapting to life with spinal stenosis requires a comprehensive understanding of the condition, along with an implementation of lifestyle modifications, therapeutic exercises, and medical treatments as necessary. Mental Health is an essential component in this adaptation process. Individuals may experience mood swings, anxiety, or depression due to the chronic pain and associated lifestyle changes. As a result, cognitive-behavioral therapy or counseling could be beneficial.
Emotional coping is another significant aspect. Techniques such as mindfulness, relaxation, or stress management can help patients deal with the emotional impact of the disease. Patients should also maintain open communication with their healthcare provider about the severity and frequency of symptoms, which can aid in tailoring an appropriate treatment plan.
Physical adaptations can involve the use of assistive devices such as braces, canes, or walkers, as well as home modifications to minimize the strain on the spine. Regular, low-impact exercises, like swimming or cycling, can help maintain mobility without exacerbating the condition.
Nutrition also plays a vital role. A balanced diet rich in calcium and vitamin D supports bone health, while maintaining a healthy weight reduces stress on the spine. Adequate hydration helps maintain disc health, further mitigating symptoms.
Preventing Spinal Stenosis
While the onset of spinal stenosis can be influenced by genetic predispositions, certain preventative measures may impede the progression of this condition. A significant focus is on the adoption of healthy lifestyle choices, which include maintaining a balanced diet and refraining from smoking or excessive alcohol consumption. Concurrently, regular physical exercise, especially routines that strengthen the back and improve flexibility, plays a pivotal role in maintaining spinal health and reducing the risk of spinal stenosis.
Healthy Lifestyle Choices
In the domain of spinal stenosis prevention, the adoption of certain healthy lifestyle choices plays a fundamental role in maintaining the structural integrity of the spine and mitigating the risk factors associated with this condition.
Key elements include:
- Dietary Impact: Consuming a diet rich in anti-inflammatory foods, such as fruits, vegetables, and lean proteins can help reduce inflammation in the body and protect the spine.
- Stress Management: Chronic stress can exacerbate existing spinal conditions and contribute to the development of spinal stenosis. Mindfulness techniques, meditation, or therapeutic exercises can be effective stress-relief strategies.
- Healthy Weight: Maintaining a healthy weight can help reduce pressure on the spine and lower the risk of spinal stenosis.
- Avoiding Tobacco and Alcohol: These substances contribute to inflammation and degeneration of spinal structures. Abstaining can greatly aid in prevention.
Regular Physical Exercise
Engaging in regular physical exercise constitutes a critical strategy for the prevention of spinal stenosis, as it promotes flexibility, strengthens the musculature supporting the spine, and aids in maintaining a healthy body weight. Exercise modifications are often necessary to accommodate individual capabilities and to avoid straining the spinal area. Low-impact activities such as swimming and walking, for instance, can be beneficial without causing undue stress on the spinal column. The aerobic benefits that such activities offer include increased blood flow to the back, promoting healing and reducing stiffness. Additionally, exercises focusing on core strengthening can bolster the muscles around the spine, providing additional support and lessening the likelihood of developing spinal stenosis. A consistent, well-designed exercise regimen is instrumental in spinal health.
Latest Research on Spinal Stenosis
Recent advancements in spinal stenosis research have sparked a plethora of innovative therapeutic approaches, each aiming to revolutionize the management and treatment of this debilitating condition. The exploration of Stenosis Genetics has unmasked important genetic risk factors, providing a new target for therapeutic intervention. Simultaneously, the potential of Alternative Therapies is being scrutinized, offering a promising avenue for non-surgical management.
The latest research on spinal stenosis has unearthed several enlightening findings:
- A study by The Spine Journalindicated an association between certain gene variants and an increased risk of lumbar spinal stenosis, paving the way for gene-targeted treatments and preventive strategies.
- A surge in the exploration of alternative therapies has led to the recognition of the beneficial effects of therapies such as acupuncture and chiropractic in relieving symptoms.
- The potential role of stem cell therapy in regenerating damaged tissues in the spine is being explored, with initial studies showing promising results.
- The development and enhancement of minimally invasive surgical techniques continue to revolutionize the surgical management of spinal stenosis, resulting in better patient outcomes with fewer complications.
These breakthroughs have the potential to reshape our understanding and treatment of this condition, providing hope for those affected by spinal stenosis.
Frequently Asked Questions
What Is the Recovery Timeline After Spinal Stenosis Surgery?
The recovery timeline following surgery varies, typically lasting several weeks to months. This is influenced by post-surgery complications and the efficacy of rehabilitation techniques employed to restore function and mobility.
Can Exercises Worsen My Spinal Stenosis Condition?
Certain exercises, if not performed correctly, may exacerbate your condition. However, a well-designed program focusing on stenosis prevention and pain management can effectively aid in improving overall health and symptom management. Always consult your healthcare provider.
Does Spinal Stenosis Qualify as a Disability for Insurance Purposes?
Determining if a condition meets the criteria for a disability under insurance purposes relies on the specific Disability Criteria established by the insurance provider. Consult with your insurer regarding their guidelines on Insurance Coverage.
Are There Any Recommended Dietary Changes for Managing Spinal Stenosis?
Certain dietary modifications can aid in managing stenosis. Consuming anti-inflammatory foods and stenosis supplements, rich in Omega-3 fatty acids, Vitamin D and calcium, can potentially alleviate symptoms and support overall spinal health.
Can Spinal Stenosis Affect Pregnancy or Childbirth?
Pregnancy and childbirth can be influenced by various conditions, including stenosis. Stenosis prevention and maintaining appropriate pregnancy posture are essential to mitigate potential risks related to spinal compression during these significant life events.