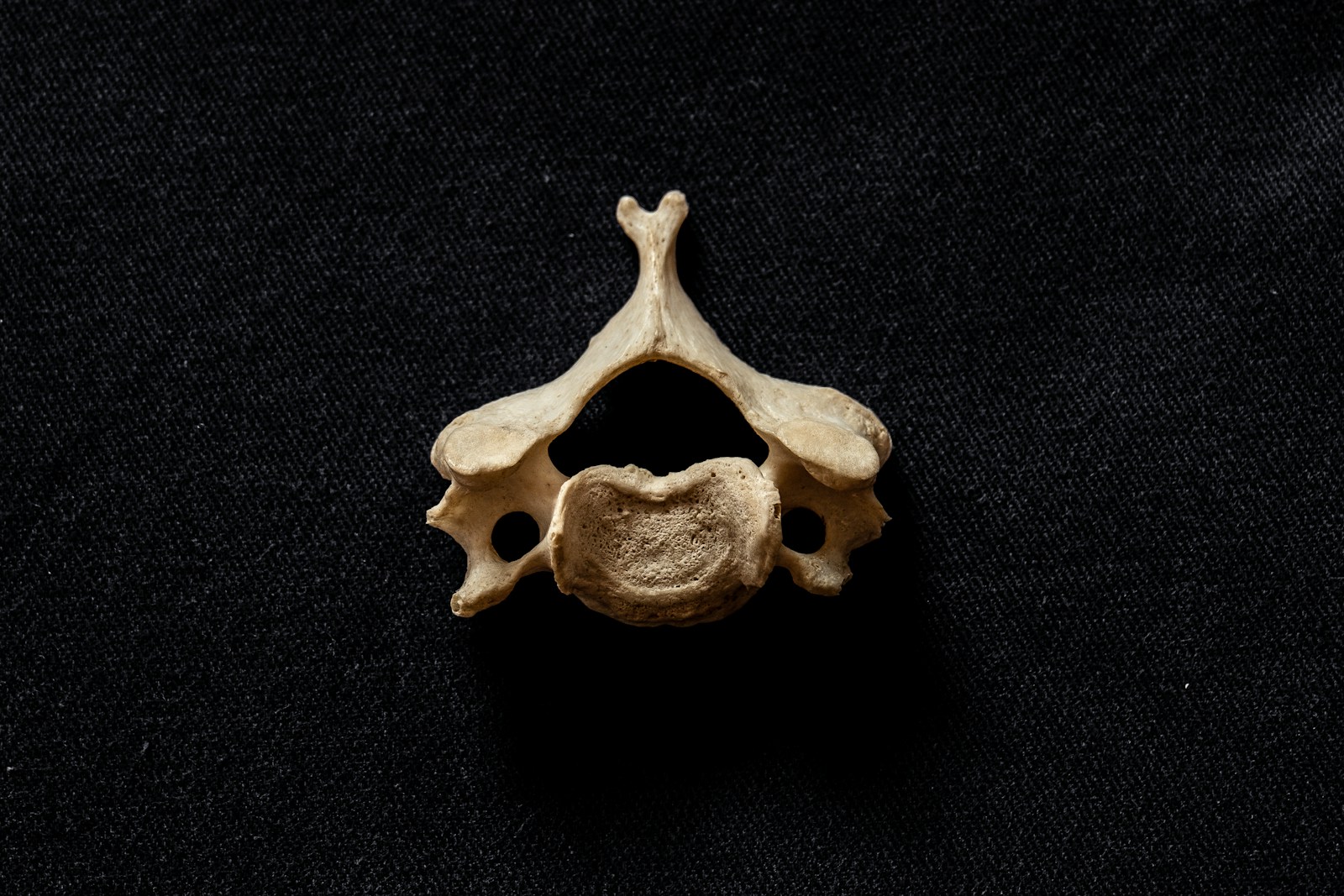
The human spinal column, a masterful blend of form and function, is an intricate structure that begs for a deeper understanding. It performs the dual tasks of providing structural support and housing the delicate spinal cord, all while facilitating movement. Comprising a series of interconnected bones, discs, and soft tissues, each component of the spine has its unique role and intricacies. It is fascinating to explore how these elements work in concert to create a dynamic, flexible yet robust system. This understanding could illuminate pathways for innovative treatments and preventive strategies for spinal disorders.
Understanding Spine Anatomy
Unraveling the complexity of spine anatomy is essential to understanding how this central pillar of the human body supports movement, protects the spinal cord, and maintains structural balance. The spine’s flexibility, a product of its intricate structure, plays a pivotal role in enabling a wide range of movements while simultaneously withstanding significant loads.
The evolution of the spine has been a prolonged process, with changes driven by the requirements of bipedal locomotion, leading to its unique S-shaped curvature in humans. This evolutionary development has enhanced our ability to walk upright and maintain balance, but it also imposed additional stresses, making the spine more susceptible to structural issues.
The specialized nature of each region of the spine contributes to its overall flexibility and strength. For instance, the cervical region is designed for mobility, the thoracic region for stability, and the lumbar region for load-bearing. The intervertebral discs, spinal muscles, and ligaments further contribute to spine flexibility, allowing for bending, twisting, and extension movements.
In essence, understanding spine anatomy requires a thorough grasp of its evolutionary development, structural design, and biomechanical functions, which are all vital to achieving and maintaining spinal health.
The Vertebral Column
The vertebral column, a critical aspect of spine anatomy, encompasses numerous key components that contribute to its fundamental functioning and potential disorders. This discussion will primarily focus on the intricate structure of the vertebral column, its essential role in the human body, and common abnormalities that may affect its operation. Our analysis will provide an in-depth understanding of the framework, functionality, and pathologies associated with the vertebral column.
Vertebral Column Components
Comprising a series of interconnected bones and discs, the vertebral column, also known as the spine, serves as the central axis of the human skeletal system. This complex structure consists of approximately 33 individual bones, called vertebrae, which are notably different in shape and size, demonstrating considerable vertebral variations. These vertebrae are divided into five regions: cervical, thoracic, lumbar, sacral and coccygeal. Over the course of spinal evolution, these regions have developed distinct curvatures that enhance balance and flexibility. Each vertebra is separated by intervertebral discs, which provide cushioning and facilitate movements. Ensconced within this column is the spinal cord, a key component of the nervous system, which transmits signals between the brain and the rest of the body.
Spine Functionality and Disorders
Beyond its structural role, the vertebral column performs several critical functions, and its health is essential for overall well-being, but disorders can greatly impair its functionality. The vertebral column provides support for the body, facilitates movement, and protects the spinal cord. Disorders like herniated discs, spinal stenosis, or spondylolisthesis can cause pain, numbness, and reduced mobility. Spinal Surgery Options, such as discectomy, laminectomy, or spinal fusion, can alleviate these symptoms. Post-surgery, Spinal Trauma Recovery may involve physical therapy and pain management strategies. Early diagnosis and treatment of spine disorders are crucial to maintain its functionality and improve the quality of life. Hence, a thorough understanding of spine anatomy is essential for effective treatment and patient care.
Intervertebral Discs Explained
The intervertebral discs, structurally composed of a soft inner core (nucleus pulposus) and a tough outer ring (annulus fibrosus), serve a critical function in the spinal column by providing cushioning and facilitating movement. Disc-related health complications arise when these structures become compromised, leading to conditions such as disc herniation or degenerative disc disease. In the following sections, we will elucidate the anatomical structure of these discs, their role in the spine, and the health issues associated with them.
Disc Function and Structure
Intervertebral discs, acting as shock absorbers in the spine, demonstrate a unique and complex structure designed for supporting weight and enabling movement. This dynamic function is dependent upon disc hydration and the natural spinal curvature.
- Disc hydration: Water is essential for maintaining disc health and function. The nucleus pulposus, the disc’s inner core, relies heavily on hydration for its gel-like consistency, which in turn enables it to bear spinal load effectively.
- Spinal curvature: The spine’s natural curves assist in weight distribution. These curves are dependent on the discs’ shape and size, which variate between different spinal regions.
- Disc structure: Comprising an outer annulus fibrosus and inner nucleus pulposus, the structure of the disc is integral to its shock-absorbing properties, enabling flexibility while providing necessary support.
Disc-related Health Issues
How do intervertebral disc disorders, such as disc degeneration or herniation, impact the spine’s overall health and functionality? Disc degeneration, a result of aging, can limit spinal mobility, increase pain and reduce overall quality of life. Herniation, or disc prolapse, occurs when the soft inner part of the disc bulges through the outer ring, compressing spinal nerves and inducing severe pain. Preventing disc prolapse involves maintaining a healthy weight, regular exercise, and proper lifting techniques. Disc degeneration treatments range from non-surgical options, such as physical therapy and medication, to surgical interventions like discectomy or spinal fusion. Both conditions have a significant impact on the spine’s function, underlining the importance of early detection and treatment.
Spinal Cord and Its Importance
Serving as the primary conduit for transmitting messages between the brain and the rest of the body, the spinal cord holds a pivotal role in the complex network of our nervous system. The spinal cord acts as a critical link, ensuring a seamless nervous system connection, and any disruption can lead to severe consequences, such as spinal cord injuries.
- Communication: The spinal cord is a major pathway for transmitting signals between the brain and body parts. This allows us to respond to external stimuli and coordinate our movements.
- Reflexes: The spinal cord is responsible for reflex actions. These are automatic responses to specific stimuli, bypassing the brain’s conscious control, providing a rapid response to potential harm.
- Homeostasis: The spinal cord plays an essential role in maintaining homeostasis. It controls autonomic functions like heart rate, blood pressure, and body temperature.
Spinal cord injuries are thus devastating, often resulting in loss of sensation, movement, and function below the level of the injury. Therefore, understanding the anatomy and importance of the spinal cord is critical in preventing and managing such injuries. This is the cornerstone to developing effective treatments and interventions for spinal cord disorders.

Role of Spinal Muscles
The functionality of spinal muscles plays a paramount role in the overall spine anatomy. These muscles, grouped into multiple layers, contribute greatly to movement, stability and protection of the spinal cord. Their influence extends to posture as well, with the condition and strength of these muscles directly impacting an individual’s alignment and movement patterns.
Spinal Muscles Functionality
In the intricate ballet of human movement, spinal muscles perform critical roles, ranging from providing stability to the vertebrae, facilitating movement, and protecting the spinal cord from injury. The importance of muscle strength and the significance of spinal flexibility cannot be overstated.
- Stability: Spinal muscles provide necessary support to the vertebral column, preventing any undue stress or strain on the skeletal system.
- Movement: These muscles facilitate a wide range of movements, from simple bending and twisting to complex physical activities.
- Protection: They serve as a protective barrier for the spinal cord, cushioning it from any potential harm that could lead to debilitating conditions.
Understanding these functionalities is crucial for maintaining excellent spinal health and preventing potential injuries.
Muscles Impact on Posture
Beyond their role in stability, movement, and protection, spinal muscles profoundly influence our posture, shaping the alignment and balance of the body. Weak or imbalanced muscles can lead to poor posture, causing strain on the spine and potentially leading to discomfort or injury. Muscle Strengthening Techniques help to build and balance these critical muscles, promoting healthier, more robust spinal support. Techniques may include resistance training, isometric exercises, and dynamic movements. Additionally, Postural Correction Exercises aim to rectify deviations in posture by targeting specific muscle groups. These exercises can enhance muscle endurance and flexibility, along with promoting better body awareness. Hence, a well-planned regimen of Muscle Strengthening Techniques and Postural Correction Exercises plays a crucial role in maintaining excellent spinal health and posture.
Ligaments in the Spine
A critical component of the spine’s structural integrity, ligaments provide essential support and stability, connecting bones and controlling their range of motion. Ligaments are tough bands of fibrous tissue, designed to withstand significant stress while limiting the movement of the vertebrae to prevent injury. Ligament injuries, such as sprains or tears, can have a profound impact on this function, leading to instability, pain, and reduced mobility.
Ligament healing is a complex, multi-stage process involving three key stages:
1. The inflammatory stage, where damaged cells and debris are removed.
2. The proliferative stage, involving the production of collagen and the formation of new blood vessels.
3. The remodeling stage, where collagen is organized and matured to restore strength and flexibility to the ligament.
Critically, ligament healing is often slower than that of other tissues, due to their relatively poor blood supply. Hence, addressing ligament injuries promptly and correctly is of utmost importance to prevent chronic instability or osteoarthritis in the future. Understanding the role and function of ligaments in the spine is thus essential to maintaining spinal health and ensuring effective recovery from injury.
The Cervical Spine
Comprising the uppermost part of the vertebral column, the cervical spine consists of seven vertebrae that provide essential support and flexibility to the neck. These vertebrae, denoted as C1 through C7, are smaller in size compared to other spinal vertebrae, owing to their pivotal role in supporting the weight of the head.
Due to its critical function and location, the cervical spine is susceptible to a variety of injuries, collectively referred to as cervical spine injuries. These can range from minor strains and sprains to more severe conditions such as cervical radiculopathy, disc herniation, and spinal stenosis. Cervical spine injuries can result from an array of causes such as sporting accidents, motor vehicle collisions, falls, and degenerative diseases.
Cervical spine manipulation, a form of treatment performed by healthcare professionals, is often employed to alleviate pain and improve functional mobility in patients with cervical spine disorders. This form of manual therapy, however, should be conducted judiciously, considering potential risks such as vertebral artery dissection. It is essential to have a thorough understanding of the cervical spine’s intricate anatomy to prevent injury and optimize therapeutic outcomes.
Anatomy of the Thoracic Spine
Moving downwards from the cervical spine, we encounter the thoracic spine, a complex structure that forms the middle segment of the vertebral column and plays a significant role in the overall stability and function of the spine. Comprised of twelve vertebrae, it supports the rib cage and provides attachment points for several muscles, enabling a range of movements such as bending and twisting.
The thoracic spine’s structure is unique. To clarify, here are three key features: 1. Vertebrae: The thoracic spine consists of twelve vertebrae, labeled T1 to T12. These vertebrae are larger and stronger than the cervical vertebrae, reflecting their weight-bearing function. 2. Rib Attachments: Each thoracic vertebra has a pair of ribs attached to it, contributing to the ribcage positioning impact on our respiration and posture. 3. Limited Mobility: Despite its strength, the thoracic spine has limited mobility compared to other spinal segments, emphasizing the importance of thoracic mobility exercises to maintain flexibility.
Understanding the thoracic spine’s anatomy is essential for maintaining spinal health. By performing relevant thoracic mobility exercises and considering the ribcage positioning impact, we can better manage our overall spinal function.
The Lumbar Spine Structure
Descending further along the vertebral column, we encounter the lumbar spine, a robust segment of the spinal anatomy that bears the majority of the body’s weight and facilitates a variety of complex movements. Comprising five larger, thicker vertebrae (designated L1-L5), it is these structures that give the lumbar region its characteristic strength and flexibility.
The lumbar spine’s vertebrae are separated by intervertebral discs, whose purpose is to act as shock absorbers and to allow for spinal movement. Facet joints at the back of the spine enable sliding movements, while the muscular structures surrounding the lumbar spine aid in rotation and stability. Lumbar mobility exercises focus on these areas, aiming to improve flexibility, increase range of motion, and alleviate discomfort.
A common site for injuries due to its load-bearing function and range of motion, the lumbar spine can suffer from a variety of issues. Lumbar spine injuries often result from excessive force or repetitive stress, leading to conditions such as herniated disks, spondylolisthesis, and spinal stenosis. Understanding the intricate structure of the lumbar spine is crucial in diagnosing, treating, and rehabilitating these conditions.
Spine Conditions and Disorders
While the spinal column is a marvel of natural engineering, its complexity renders it susceptible to a range of conditions and disorders that can compromise both structure and function. Conditions such as spinal stenosis and scoliosis are among the most prevalent and can drastically affect the individual’s quality of life.
- Spinal Stenosis: This condition, characterized by the narrowing of the spinal canal, is increasingly common, especially in the aging population. Spinal Stenosis prevalence has been noted to increase with age, often leading to significant pain, numbness, and in some cases, motor function impairment.
- Scoliosis: This disorder is marked by an abnormal curvature of the spine, typically developing during adolescence. Scoliosis treatments are multifaceted and can range from bracing and physical therapy to surgical interventions in severe cases.
- Degenerative Disc Disease: This is a condition not uncommon as people age, where spinal discs break down, often resulting in pain and other complications.
Understanding these and other conditions is vital in managing spinal health effectively. However, it’s important to remember that, while these disorders are common, they are not inevitable, and numerous strategies exist to promote spine health and prevent these conditions.
Advancements in Spine Health
In light of these prevalent spine conditions, it is encouraging to observe the remarkable strides being made in the field of spine health, with a multitude of innovative treatments and preventive strategies emerging in recent years. Particularly, spine surgery innovations have dramatically improved the prognosis for many patients. Minimally invasive procedures, such as endoscopic discectomy and percutaneous pedicle screw fixation, have greatly reduced recovery times and minimized post-surgical complications. Additionally, advances in spinal fusion techniques and materials are contributing to improved stability and functionality post-surgery.
Physical therapy advancements are also playing an instrumental role in enhancing spine health. High-intensity laser therapy is now being utilized to alleviate pain and inflammation and promote tissue regeneration. Furthermore, the application of cutting-edge technologies such as virtual reality and robotics in physical therapy is paving the way for more effective and personalized treatment plans. These advancements, in conjunction with a deeper understanding of spine anatomy and mechanics, are making it possible to manage and prevent spine conditions more effectively. The future of spine health looks promising, with continual research and development in this field set to further improve patient outcomes.
Frequently Asked Questions
What Lifestyle Habits Can Affect Spine Health Negatively?
Smoking effects, such as reduced blood flow, can negatively impact overall health, including the spine. Additionally, excessive alcohol consumption may lead to osteoporosis, which weakens the spine, increasing the risk of fractures and other injuries.
How Does Aging Impact the Health of the Spine?
Aging imposes significant impacts on spinal health, primarily through processes like spinal degeneration and age-related disc problems. These can lead to conditions such as osteoarthritis, spinal stenosis, and disc herniation, necessitating preventive measures for peak health.
Can Yoga or Pilates Improve the Strength of My Spine?
Yes, yoga and pilates can enhance spinal flexibility and strength, which is essential for maintaining posture and injury prevention. Regular practice can promote spinal health by improving alignment and reducing strain on the spine.
What Are Some Non-Surgical Treatments for Spinal Disorders?
Non-surgical treatments for spinal disorders include physical therapy, spinal bracing, and acupuncture. Spinal bracing benefits include improved stability and posture, while acupuncture is effective in relieving pain and improving overall spinal health.
How Does Poor Posture Affect the Anatomy of the Spine?
Poor posture can lead to spinal deformities impacting its natural alignment. This may cause chronic discomfort and functional impairments. Posture correction techniques can help mitigate these issues by promoting ideal spinal health and reducing related symptoms.